Items
topic_interest is exactly
healthcare
-
 2021-04-11
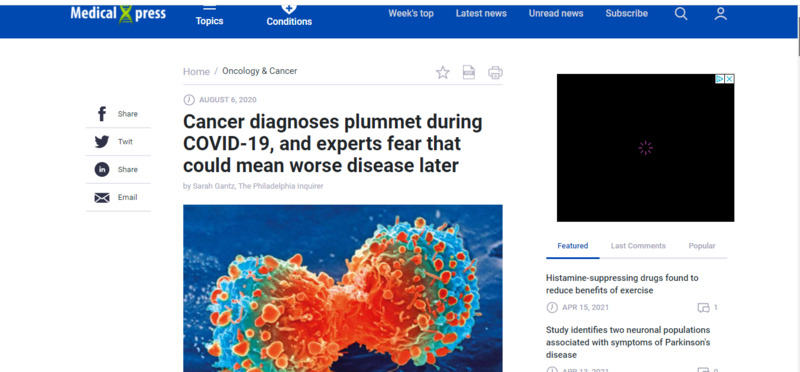
2021-04-11Cancer diagnosis rates go down!
I know I have presented a pretty eye catching and exciting title, but the fact of the matter is, they aren't going down. The amount of people who have cancer has not plummeted, as the title suggests. Rather, the statistics have gone down. As the article states, "new findings offer grim evidence of the consequences of delayed care: A rise in undetected cancers that, when eventually diagnosed, may be more advanced and difficult to treat." I think this is a great reminder that statistics are not the people they represent, and many things effect the numbers. This is relevant to my research on the unintended consequences of the COVID-19 pandemic. -
 2021-04-11
2021-04-11Postponing Basic Health Care During the Pandemic
I have been researching the unintended consequences of the COVID-19 pandemic. One consequence that interests me the most is people missing important specialist appointments for things like heart disease or cancer. I would have assumed that it would be the lower class skipping these appointments the most due to the fact that is many cases it is already harder for lower class people to get to regular appointments. But this article proves my thought wrong, and states that the lower and middle class people have less opportunity to miss these appointments. They tend to have more healthcare problems, according to the article, and therefore need the appointments more. In addition, the numbers might reflect the fact that lower income people don't go to the doctor as much as higher income people in general, therefore the numbers were low to begin with. The article is a very interesting read and I highly suggest it. -
 2021-04-07
2021-04-07Indian Health Services COVID-19 Infections by Service Area through 04/07/2021
Indian Health Services is an agency of the United States federal government that oversees and administers healthcare to that nation's Native American populations and tribal reservations. This webpage from the Indian Health Services has three sections that address general Coronavirus (COVID-19) information and links, COVID-19 Vaccine Distribution and Administration by IHS Area, and COVID-19 Cases by IHS Area. it also includes a hyperlink to an interactive map for up-to-date COVID-19 Cases by IHS Area: https://maps.ihs.gov/portal/apps/StoryMapBasic/index.html -
 2021-04-03
2021-04-03Oral Interview with Toni Downs
Toni Downs is in a lead position at a hospital in Kansas. In this interview, Toni tells me about changes that have occurred at the hospital as a result of the COVID-19 pandemic. She also discusses the long term changes she suspects will stay in effect, such as visitation regulations to the hospital. Toni tells me about similarities and differences between this pandemic and the start of the AIDS pandemic. She also discusses how the number of people going to the emergency room have dropped significantly, more than 75% at the start of the pandemic. Toni believes if we all work together at stopping the spread, we will get this under control. However, she thinks many things may stay around for a while in the hospital setting, such as the before mentioned visitation rules, and even mask wearing, in order to protect hospital staff and the patients. I am researching the unexpected consequences of the COVID-19 pandemic, such as people skipping mammograms for fear of catching COVID at the doctors office. I chose to interview Toni for my research, due to her insider knowledge of the inner workings of a hospital. -
 04/03/2021
04/03/2021Brittni Smith Oral History, 2021/04/03
Brittni Smith lives in a small town in Kansas. Here, I interview her about her experiences during the COVID-19 pandemic. She talks about what it was like getting a COVID test. Brittni also tells me about what it was like to have family hospitalized during a pandemic. Her work furloughed her for a few months at the beginning of the pandemic, which she also tells me about. I am researching the unexpected consequences of the pandemic; a good example would be people not going to the doctor for checkups for fear of catching COVID. I interviewed Brittni for this research. -
 2021-01-21
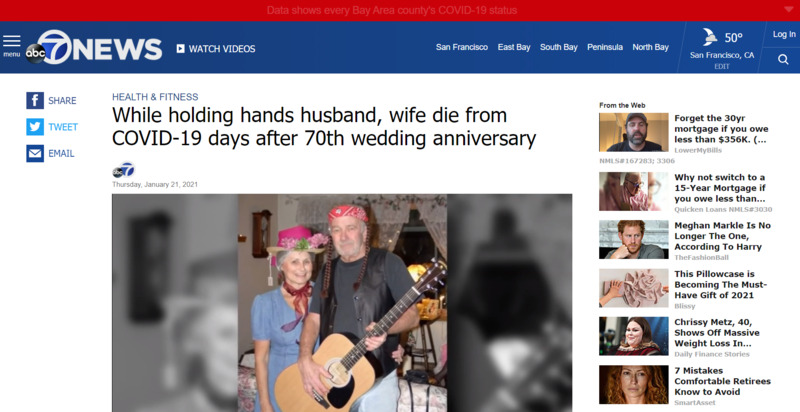
2021-01-21While holding hands husband, wife die from COVID-19 days after 70th wedding anniversary
The increasing death toll from COVID-19 has devastated many families on a personal level. One instance illustrates that like no other. An Ohio couple that had recently celebrated their 70th wedding anniversary both passed away minutes apart, leaving behind seven decades of memories, five children, 13 grandchildren and 28 great-grandchildren. Dick and Shirley Meek celebrated their anniversary on Dec. 22. It was then when they innocuously told their children they were feeling a little under the weather. "They said to all us kids, 'we think we're getting colds,'" said Kelly Meek. But suddenly, things got bad and it was evident this was no mere cold. On Jan. 8, they both tested positive for COVID-19. When things started to worsen for both of them, the family asked for them to be together for their final moments. Hospital staff found a room for two beds and the necessary equipment. Dick and Shirley died in each other's arms on Jan. 16. They were due to get the COVID-19 vaccine on Jan. 19. -
 2021-01-15
2021-01-15My Grandma Made Front Page Again
My grandma Pauline Bell made the front page of our local paper again. This time, she was one of the first in the area to receive the vaccine. We were all so happy for her and what this might mean for all of us who miss her. -
 2021-03-11
2021-03-11Healthcare providers honor Covid-19's One Year Anniversary
This article is about the one-year anniversary of Covid-19 and how healthcare providers are celebrating and honoring the occasion. Healthcare workers and EMS providers have spent the past year on the front-lines of the Covid response. They have sacrificed much and have seen unprecedented horrors during this pandemic. This article features several social media posts from various healthcare agencies. In all of these posts, they acknowledge the patients and providers that we have lost in the past year, but also celebrate the efforts of the providers in trying to help the public during this pandemic. -
 2021-03-12
2021-03-12Long-term Vaccine Effect Research Project
This article is about the Healthcare Worker Exposure Response and Outcomes (HERO) research project. They are trying to understand the long-term effects of the Covid-19 vaccine. The population that they are using is first-responders, who were among the first group to receive the vaccine in most states. The project plans to conduct periodic surveys over a 2 year period. Since this vaccine was produced in record time, and especially the lack of available data to the long term effects, it is an important project. The project also surveys the first responders regarding their mental health during the pandemic. It includes fire fighters, EMS providers, and law enforcement. -
 2020-06-20
2020-06-20For LGBTQ Patients, the Coronavirus Brings New Challenges
This article by John Hopkins Medicine is talking about how the COVID-19 pandemic has impacted the LGBTQ+ community. The doctor points out that community members are more likely to be smokers and so they are higher proportionately to have complications with COVID-19. The doctor also points out that gender-affirming surgery in the Transgender community has been delayed or is not being done at all which has impacted that community greatly. It is important that the doctor gives the advice to not isolate ourselves in the LGBTQ+ community throughout the pandemic. -
 2021
2021The Lives and Livelihoods of Many in the LGBTQ Community are at Risk Amidst COVID-19 Crisis
The story speaks about how many people in the LGBTQ community are at risk while the COVID-19 crisis is occurring. The study shows that people within the community have less access to healthcare, a greater risk of health complications due to COVID-19, and do not have paid leave. -
 2021-03-26
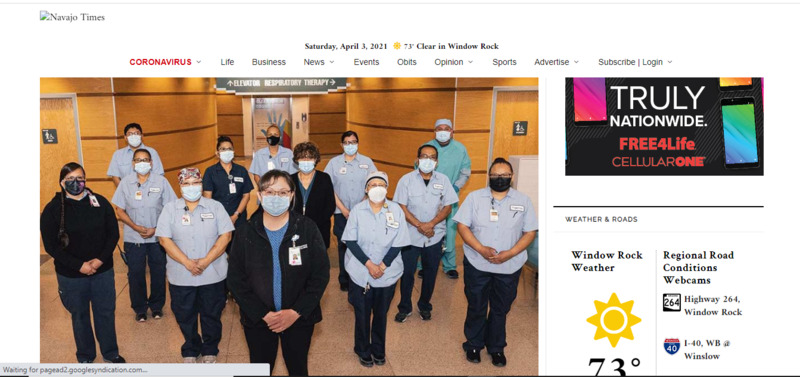
2021-03-26‘They became warriors’: Reflections from the front lines as Tséhootsooí Medical Center workers share experiences
By Rima Krisst | Mar 26, 2021 | CORONAVIRUS, People | Tséhootsooí Medical Center workers share experiences Wilberta “Billy” Jackson, public health nurse III This pandemic has been the longest roller coaster of stress, grief, and loss. I’ve kept my routine simple – sleep, eat, and exercise. And, more sleep. This has been and will probably be the most challenging time of our lives. I could focus on all the bad, but so much good has come from this, from community members stepping up, leaders rolling their sleeves up and getting dirty, how we came together to care for our elders, and so much more. Professionally, we’ve adjusted and readjusted a million times over and completely changed how we deliver health care. We’ve had information, guidance, and policies being added or changing every day and we still were able to deliver health care in a safe, efficient manner. At the beginning of the pandemic, our leaders were warning everyone about the health care system being overwhelmed. Most people thought about it in terms of hospitals running out of beds, but they didn’t think of it in terms of how an underfunded and shorthanded public health force would respond to a pandemic in a rural area with limited resources, and where a population’s most basic physiological and safety needs are not being met. When you don’t have access to clean water, food, shelter and security, you’re not able to prioritize prevention measures until your basic human needs are addressed. The resiliency of the Diné people is unrivaled. The days I’m struggling or feel like giving up, I hear my grandmother’s words, and that’s what keeps me going. And my mother’s surprise delivery of Navajo soul food meals. I’m a public health nurse, so it won’t come as a surprise that I’m excited about the COVID vaccines. We’ve already seen a substantial decline in cases, hospitalizations, and deaths, so we know it’s working. My hope is that our response to the next pandemic or health care crisis won’t be complicated by politics, lack of national strategy, lack of preparation, and misinformation. Stacey Burnside, Primary Care registered nurse What I have learned from this pandemic is to cherish every day and every person that you love. COVID-19 has impacted my family and me profoundly. I lost an uncle and an aunt to COVID-19, and to this day, it is surreal that they are gone. As a primary care nurse, it is difficult to hear about losing a patient to COVID-19, and at the peak, it was almost a daily occurrence… The challenges that I faced during this pandemic were adapting to the changes in work roles and being separated from the people I love. The clinic that I worked in was closed when the pandemic hit the first peak, and I, along with my coworkers, was informed that we had to work in the Emergency Room. The moment that I saw a patient who needed me to be their nurse, despite having COVID-19, humbled me. That moment in the ER humanized COVID-19 for me and made me realize that I was put there for a reason. No matter what the situation is, nurses adapt, and the teamwork and strength we draw upon each other are phenomenal. A huge hit to me personally and professionally was losing a friend to suicide … dealing with grief, loss, and stress has been a daily thing. What has helped me is drawing strength from my God, husband and son, and family. There are many negatives to the pandemic, but one positive that many have seen is the love and strength we have found among our families. I am thrilled that we are at a point of a high vaccination rate in the Navajo Nation. I remember when I administered my first COVID-19 vaccine to a patient, it brought tears to my eyes, and I cried after work. Leah Chattin, respiratory therapist I’ve been a respiratory therapist since 2003. What I experienced throughout the first surge of COVID-19 here on Dinetah is not what you prepare for. I see the impact on my life as deep internal scars that I buried and to resurface those experiences is a nightmare. Imagine the inability to fully take a deep breath, something so simple we take for granted. Supporting my patients with breathing treatments, providing chest physical therapy, changing breathing devices constantly because the demand for oxygen escalates all in a 12-hour or more shift. All these specialized techniques to avoid the last option of intubation, allowing an artificial airway introduced to your trachea with an opening at the tip to provide mechanical breaths from a mechanical ventilator. Fear expressed from my patients was a frequent emotion. You are alone, isolated from your family, your loved ones, no familiar face to embrace, to celebrate your improvement or the worst, a decline despite the battle you have endured. I’d remind my patients not to give up… Instinct took over because I’m a mother too, a nurturer. I can remember softly stroking their hair, holding their hands, shedding tears, praying, putting myself in that empty place at bedside where your family should be gathered, processing the grief. Accepting loss was tremendously difficult. I lost myself because I did not decompress my emotions. My spirit slivered away slowly each time my patients faced rejection of our efforts to sustain life. How I endured and sustained my sanity was prayer requests. Prayer was undoubtedly my saving grace. This virus is fluidic, the path it took was unpredictable. I strongly believe we need to continue wearing a mask, following the CDC guidelines and begin or sustain our health and wellness. Putting into words my experience was not an easy effort, however it’s a pathway for healing. Every COVID patient I battled for will forever have a place in my heart. Sandra Fouser, nurse executive of the Primary Care and Specialty Clinics Seeing the virus cross the ocean and hit the heart of the Navajo Reservation forever changed our lives. As a health professional, I knew venturing into the unknown with limited protection meant some would survive and some wouldn’t. What I have learned working on the front lines – compassion, cohesiveness, companionship, strength, sadness and mental stress. We have been battered, beaten, praised, comforted and have also received recognition from all walks of life. I am proud to be a nurse. I believe the strength to endure comes from resiliency and the people we work with and the support of our families at home. As nurses, we cannot stand still. I feel it is in our blood to help and move forward. I have lost friends, coworkers, relatives and patients. The grief I feel is palpable, almost more than I can handle. Seeing my family, staff and patients suffer through illness and grief has been very challenging and heartbreaking. As a team, I believe when something happens to one of us, we all feel the effects, we grow closer and find comfort in each other. I see the vaccine as a progression toward eradicating the detrimental effects of this virus and giving us hope that there is a better tomorrow and that Hózhó will be restored. Dr. Karen Williams, hospitalist physician I am a Native physician (Mountain Maidu/Apache) and Indian Health Service Professional Scholar. When the pandemic started our hospitals were suddenly overwhelmed with large numbers of very ill patients needing oxygen. Some patients who worsened were placed on a “life support” or ventilators since they could no longer breathe on their own. Despite our best medical management efforts, including use of high-flow oxygen, there were patients who did not survive. I witnessed more death in a year than I have ever experienced in my career. This was traumatic for me because every day I came to work I felt like I was coming into a war zone. We saw people struggling to breathe and fighting for their life. We heard family members saying their goodbyes to their loved ones and crying over the phone. We held hands of those who took their last breath and witnessed co-workers not able to control their tears. If it were not for our team efforts, almost a military-style mentality, we could not have managed. As a hospitalist physician, the biggest challenge was ensuring that I had the most up-to-date medical knowledge to save a patient’s life. During the beginning of the pandemic many doctors throughout the country did not feel prepared. This was quickly overcome by learning medical strategies used by doctors throughout the world. The treatments used included steroids, anticoagulant medications, and high-flow oxygen. We had the support of our hospital’s incident command leadership and adapted to the changes. This included being able to offer our patients who needed oxygen a federal Drug Administration-approved “emergency use” medication called Remdesivir, and more recently Bamlavinimab for non-hospitalized patients My experiences on the front lines were psychologically and physically overwhelming … I sought support from elders and used my Native spirituality for strength. I also sought protection support from traditional Indian practitioners who set up a tipi and hogan outside the hospital for employees. I sometimes thought twice about the danger I was in. However, I acknowledged that I would never walk away. This is a result of my obligation to the Native community and the hundreds of patients I had gotten to know for so long. I “warriored up” in my mind and sought to do the best I could. I do not foresee an end to mask wearing, and now recognize how careful we all must be to protect each other. I saw too many elders get severely ill and even pass away from COVID as a result of young family members not being careful and bringing it home. I have encouraged community members and my own family to get the vaccine as soon as possible. I received two doses of the Pfizer vaccine and said a prayer in my Native way each time for protection. Natasha Topaha, certified medical assistant, Mobile Unit Overall, this year has been extremely challenging, but also has reinforced my personal strength and resiliency. I have had ongoing concerns throughout the epidemic regarding my kids’ isolation and their mental health. It has been difficult, but doable, to manage both working in health care and supporting my family both emotionally and physically. I had constant worry about bringing the virus home and infecting my family given that I was working in high risk areas and providing COVID testing, vaccines and social and mental health support to patients. I found that doing outdoor activities with my family, such as bike riding and hiking, helped me ease my stress and helped teach my children some healthy coping skills. And we could spend time together! I feel very happy and grateful in both receiving the vaccine and being able to provide it to patients and the community. I feel safer at work and at home now. Johnny Willeto Jr., facility manager/logistics chief The strength to endure comes from within yourself. For me this began in my childhood as the son of Delphine Damon Willeto and Johnny Willeto Sr., who nurtured me to become a great human being. They taught me to be a courageous, productive worker and know my limitations. As a facilities manager, my main focus and responsibilities are the protection in the physical environment of all who walk through the doors of Fort Defiance Indian Health Board’s facilities. All we knew is that COVID-19 was airborne and surface communicated. I treated it as you would tuberculosis and ensured that my staff had adequate PPE to help protect them when they are tasked with working in the patient care areas. This responsibility was a big challenge when trying to procure medical equipment such as masks, gloves, safety glasses, gowns, scrubs, and so forth. Having an MBA has allowed me to flourish in this high stress environment and to adjust with adaptations to finding supplies and creating new relationships with trustworthy suppliers. Being in close proximity to patients who are struggling with getting well can be heart wrenching. Being able to fulfill my duties in the support role to the best of my ability for my community and teammates has allowed me to sleep well at night knowing that I gave it my all. I have lost a brother-in-law who contracted the virus in the Scottsdale area of Arizona. These were very difficult times because as Navajos we are accustomed to comforting each other by a hug or handshake. With COVID, gatherings are not safe, so having family meetings for planning the funeral is off and also the funeral usually consists of 10 minutes before the burial with only a few close family in attendance. One of the biggest assets I have gained is the spiritual belief in God and keeping the communication open by saying my prayers often – to be thankful for the blessings that have come my way or when asking for strength to endure the hardships. In my free time I isolate on the Willeto Sheep Ranch in Goatsprings Valley, Arizona, where I tend 120 sheep and goats. Being able to separate the everyday stress and recharge is paramount to going forward with courage and mental sharpness to make the right choices for the organization, patients and employees. The vaccines are an effective tool to help reduce the mortality of the virus on us and give us protection to this invisible enemy. Corinne Legah, Environmental Service supervisor Personally, I was scared when I first heard of the spread of the virus overseas. It was shocking how fast the virus traveled. In the beginning our team was needed to help keep the hospital sanitized and safe for patients. We reinforced training on the cleaning process for the airborne/droplet virus. I constantly stressed wearing PPE and hand washing. I am so proud of the team for stepping up by protecting our patients. They became warriors to fight the virus. I believe without my husband’s support and God I would not have been able to cope. I have lost friends and family from this virus. It saddens me that many of our people are now in the spirit world. Being a Native and growing up with Navajo beliefs, I had to be strong. My ancestors went through so much and our people are resilient. Prayer is our strength. I cried when I watched the news when the vaccine was given to the first person in the U.S. If everyone gets their vaccine we will be able to interact with family again. I am looking forward to that day! -
 2021-03-28
2021-03-28Vaccinated
I know the LGBTQ+ Community has a higher chance to have depression, anxiety, and other health ailments like many other minority communities. This Friday I got my second dose of the vaccine. I have been encouraging others in my LGBTQ+ Community to get the vaccine so this is one less health ailment they have to worry about. -
 2021-03-22
2021-03-22BIDMC and Long-term Covid Patients
This article is about the new team at Beth Israel Deaconess Medical Center in Boston whose purpose will be to study and support Covid-19 patients with long-term symptoms. These "long-haulers" have an array of physical and mental problems after their recovery from Covid-19. Unfortunately, since research on this virus and it's effects are quite new, experts are still finding out more everyday. This team at BIDMC is one of a few multi-disciplinary teams in the country that is specifically established to provide comprehensive care to these "long-haulers." With so many people contracting Covid-19, teams like this will be critical in how we move forward. As a matter of public health, we need to better understand if there are physiological changes to things like our lung and airway structures, brains, and other organs from having Covid, and if they are permanently damaged or not. This team will not only help these patients, but also help discover important answers for the public as a whole. -
 2021-03-18
2021-03-18Disparities in Healthcare during Covid-19
This article is about the disparities in populations that have been impacted by Covid-19. The CDC found that American Indian, Alaska Native, African American, and Latino people were almost three times higher than non-Hispanic white people in hospitalizations during the pandemic so far. These numbers are, unfortunately, more a reflection on our healthcare system as a whole, not just specific to Covid. Dr. Felicia Collins, a distinguished graduate of Harvard Medical School, is the keynote speaker at the 2021 Alvin F. Poussaint, MD Visiting Lecture and will be discussing these healthcare inequalities. On top of having an MD, Dr. Collins also has a Master's in Public Health (also from Harvard), which gives her a unique perspective into healthcare at the individual and population levels. Analyzing healthcare data through the lens of a physician must give her the ability to contextualize healthcare disparities in a way that others would not. This sounds like it will be an interesting lecture on a very important topic, and will of course be held over zoom. -
 03/13/2021
03/13/2021Paul Jason Baker-Nicholas Oral History, 2021/03/26
Paul Jason Baker-Nicholas gives an oral history interview about how COVID-19 has affected the LGBTQ+ Community. -
 03/13/2021
03/13/2021Covid-19's Effect on LGBTQ+ Community in NYC
Interview with Krystal McRae -
 2021-03-01
2021-03-01Native Hawaiians and Pacific Islanders, Vaccinations
When we say end violence against our elders, this means demanding accessible, equitable and culturally responsive healthcare services for them. Here are some community-based resources who have been doing this work: @pacificislandercovid19 @picawashington @empoweredpi Thank you Seattle Times for amplifying how COVID and inequitable health care services impact our communities in Washington. The impacts are detrimental and NHPI communities are impacted at disproportionate rates. Check out the entire article @seattletimes. Some things this article highlights - vaccine services provided need to be inclusive of different cultural lifestyles and practices, lumping Asian and NHPI data together invisiblizes NHPI needs, there is a great need to bring community-based groups to the table to build accessible systems and solutions. (Image description: a carousel of 9 slides from an article by Seattle Times. 1. A front page article that reads to fight covid-19 with vaccines, native Hawaiians and Pacific Islanders in Washington first need to be seen. 2. A quote in simple black text that reads "that is one of the things that we continue to think about How do we honor those that have passed during the pandemic? Our elders have so many stories, so much knowledge and they're essentially the wisdom keepers of our culture" seia Said. 3. The numbers tell the devastating story. Native Hawaiians and Pacific Islanders make up about 1% of Washington state's population but account for 2% of cases in the state according to the State department of health native Hawaiians and Pacific Islanders have the highest average rate of any race and ethnicity in the state at $7,132 per 100,000 people and also lead in deaths per 100,000 with an average of 151 as of February 21st, according to the UCLA Center for health policy research" Captions continues in comments. #InSolidarity #AAPIWomenLead #COVID19 -
 2020-04-22
2020-04-22Understanding the Corona Virus Through the Lens of Racial and Social Justice
The Institute for Research on Race and Public Policy and the Social Justice Initiative host a conversation on the Coronavirus Pandemic through the Lens of Racial and Social Justice. Moderated by Barbara Ransby from the Social Justice Initiative, panelists include Dr. Linda Rae Murray, Aislinn Pulley from Chicago Torture Project, Ald. Rossana Rodriguez, Ald. Jeanette Taylor, Detention Watch Network's Gaby Viera and Reyna Wences from Organized Communities Against Deportations. This program was edited by CAN TV -
 03/14/2021
03/14/2021Trisha Vaughn Oral History, 2021/03/18
Trisha Vaughn is the CPT Supervisor for a large Bay Area community hospital. In her spare time, Trisha hosts a podcast with her daughter, is an avid writer, and she is starting a small apothecary business to sell her skin care creations. In the oral history interview, Trisha shares how she has navigated through Covid-19 in both her personal life, and as an essential worker. She reflects on staying motivated and helping the people in her life stay motivated thought these hard times. Trisha describes how the social injustices and civil unrest in response to police brutality during the pandemic has affected her and those around her and about how the urgency of the pandemic has overshadowed the injustices faced by people of color across the nation. -
 03/14/2021
03/14/2021Michael Levesque Oral History, 2021/03/14
Michael Levesque was a paramedic working on an ambulance at the start of the pandemic. He had a pregnant wife at home and was in the process of switching his career into nursing. He recalls the memories of working on the ambulance and taking care of Covid patients, as well as how Covid impacted the EMS services overall. He also discusses how it felt to be starting his career as an Emergency Room nurse during a global pandemic. In both cases, his job put him directly on the front lines of medicine. He discusses the early problems of lack of knowledge and equipment to properly handle this pandemic. He also explains the mindset of an expecting father, working in a high risk environment, and then coming home to his pregnant wife. Michael’s unique life circumstances and career path gives his interview a perspective that few people experienced. -
 2021-03-02
2021-03-02North Dakota reminds vaccine providers about limits on out-of-state residents
As North Dakota continues COVID-19 vaccinations, it has been revealed that many doses have gone to out-of-state residents. Although the state isn't fully against this, they do have exceptions for some out-of-state residents that enables them to receive a COVID-19 vaccine in North Dakota. These exceptions are healthcare workers from out-of-state and patients of healthcare providers in North Dakota. There are a few other exceptions as well. -
 02/22/2021
02/22/2021Layne Williams Oral History, 2021/02/22
This interview is with medical profession Layne Williams who speaks about a positive aspect of the pandemic they noticed. -
 2020-08-05
2020-08-05Social Justice and Public Health in 2020
From the article: The COVID-19 pandemic, caused by the spread of the novel coronavirus, has created an unexpected and unprecedented lifestyle shift for many people across the globe. Several months into the pandemic, the public has been exposed to a number of issues they might not have previously considered or thought possible, from hospitals rapidly reaching capacity and the lack of personal protective equipment (PPE) to the mental and social challenges of physical distancing and being quarantined. -
 2020-04-17
2020-04-17COVID-19 and Social Justice
From the article: The COVID-19 pandemic is a health and mental health crisis, to be sure. But it is also a crisis of social injustice, inequitably affecting vulnerable and marginalized populations that include, among others, individuals who earn low incomes, or are incarcerated, homeless, in foster care, over 65 (especially those in long-term care facilities), people of color, or undocumented. Social work practitioners, educators, and policy makers are working to address the needs of these populations despite the unpredictability of the virus’s secondary impact on systems. -
 2020-10-23
2020-10-23Social justice as a foundation for democracy and health
From article: Jennifer Prah Ruger uses the covid-19 pandemic to show the importance of countries implementing a justice framework for health and equality. This article is part of a collection launched at the World Health Summit, 25-27 October 2020, Berlin, Germany. Funding for the articles, including open access fees, was provided by a grant from Bloomberg Philanthropies to the Council on Foreign Relations, support from the Konrad-Adenauer-Stiftung to the Graduate Institute of International and Development Studies, and the Institute for Health Metrics and Evaluation. -
 2021-02-02
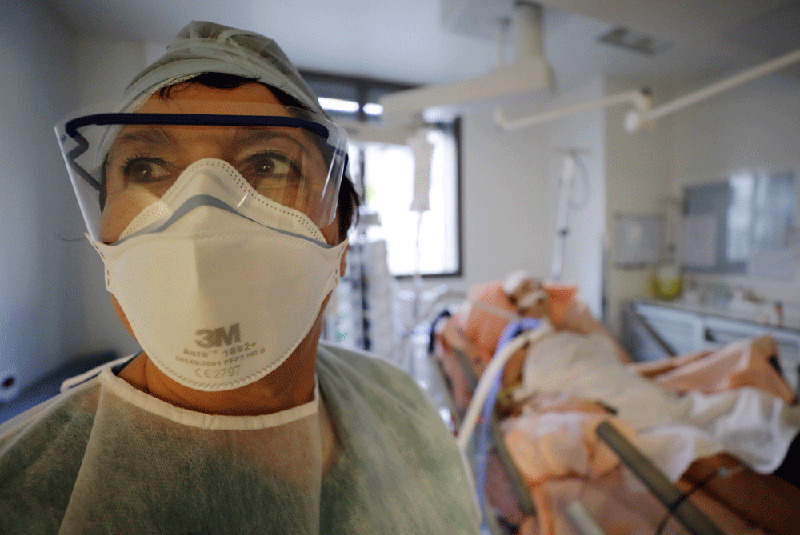
2021-02-02Inadequate Sick Leave Jeopardizes Canadian Health Workers and Patients
Due to inadequate medical supplies, lack of vaccines, and inability to slow down the spread of the virus, the pandemic rages on. To make matters worse, over half of Canadian workers lack sufficient sick leaves, which contribute to more outbreaks and the dangers of contracting COVID-19. -
 2021-02-07
2021-02-07Supporting Healthcare Workers with Meals & Food Services
Everyone can surely agree that healthcare workers are our everyday heroes. Healthcare workers are the ones who had voluntarily trained and continue to medically assist those who need it without discrimination. All this while risking their own safety and well-being during a deadly pandemic. They are no strangers to long work hours while also having to always stay alert and ready, because quality care can greatly influence someone’s life. Due to most of their time taking care of patients, one can easily see how it can drain their own health as well. Hospitals are not exactly known for their top tier food options either. For these reasons, organizations like Meals for Heroes had worked with food services to help these essential workers with their meals. With the COVID-19 pandemic closing many businesses as well due to safety regulations, we have also been seeing the same businesses (as well as bigger ones) pitch in with meals and more affordable meal plans. Some places are even giving healthcare workers food for free. https://www.uab.edu/fightcovid19/impact/meals-for-heroes https://alabamanewscenter.com/2021/01/20/meals-for-heroes-will-continue-serving-meals-to-frontline-health-care-workers-fighting-covid-19/ https://www.thrillist.com/news/nation/free-food-for-healthcare-workers -
 2021-02-05
2021-02-05Getting Sick during a Pandemic
I recently have struggled with a medical issue related to my back, quite possibly brought about by the stress of the pandemic. Getting sick during a pandemic is not only more common, due to stress, but also unnerving as you must go out to medical appointments, be around sick people, and worry about your sickness interfering with your body's work in fighting off the COVID-19 virus. -
 2021-01-07
2021-01-07THE COLOR OF CORONAVIRUS: COVID-19 DEATHS BY RACE AND ETHNICITY IN THE U.S.
This data sheet looks at the affects of Covid-19 mortality rates by race in North America. They do not interpret the data but the site says the following: We call on state and local health departments to release timely data about COVID-19 deaths with as complete racial and ethnic detail as is possible. As the data reporting improves, so too will our understanding of the devastating impact of this disease. This will inform states and communities about how to direct resources more equitably as well. -
 2020-03-16
2020-03-169 Biggest Social Justice Issues of 2020
This advertisement/article discusses nine different social justice issues North America is facing: voting rights, climate justice, healthcare, refugee crisis, racial injustice, income gap, gun violence, hunger, food insecurity, equality and how the Yeshiva University located in New York can help prepare people for the social work that can improve these issues. The article talks about how access to vital treatment during Covid-19 has impacted communities. -
2021-01-31
Volunteering Breaks Hearts
I volunteered at one of the County’s vaccination clinics last week. The health department ramped up their vaccination schedule, and we saw nearly 50% more traffic than the week prior, which was already 30% above its projections. Many of the folks over 65 (group 1C) here in Tucson are going up to Phoenix to be vaccinated as local health officials are still working their way through the 75+ crowd (Group 1B1). It has been both heartbreaking and frustrating that about a third of the vehicle occupants beg and plead for some special exemption for a family member who’s with them. Despite not yet being entitled to be vaccinated themselves, they hope someone lets them cut in line. Everyone has a special need and a special, unique circumstance that should enable them to jump ahead of their neighbors, and the selfishness of it agitates one of my few prejudices, especially when they don't take the initial 'no' for an answer. The public is so terrified, and many seem to fear they won’t manage to avoid illness in the coming weeks despite having done so for ten months now. It hurts my heart to see their suffering, to hear their fear and anxiety, to have to turn them away, and to know they’re asking for special treatment that might deny the delivery of vaccines to the most vulnerable populations. The hardest part has been, though, the number of elderly folks entitled to be vaccinated who can't navigate the online portal to get an appointment. The current vaccines are stored so cold that we can't deviate from the allotted appointments, but every day brings in elderly people who can't function in a digital world. The county can't spare personnel to offer immediate and realistic registration help to them, and many have complained of waiting on the phone for hours, only to have the county phone line hang up on them. The situation makes me want to find their grandchildren and ask why they don't give a damn about helping their grandparents. I also found out last night our organization's portion of the operation is winding down, and I do not expect to again be able to help facilitate vaccinations in my community. With time and eventual immunization, I hope to find other ways to serve my neighbors. -
2021-01-31
Suffering and Loss
I work as an investigations contractor assigned to assist my county health department with interviewing positive covid-19 patients. I recently spoke with an 85-year-old C19 patient who was hospitalized and awaiting surgery for a brain bleed at the time of our conversation. She explained that she had fallen in her backyard trying to retrieve her feral cat's bed from a rainstorm, tripped, and laid in the rain for almost two hours before anyone found her. Both she and her late husband contracted covid-19 around Christmas, and he died soon thereafter. The hospital where he received his final treatments allowed her to visit him just before he passed, which is an unusual and gracious blessing at this time. The medical interview that normally takes 30 minutes required almost two hours and tears from both of us. When we finished, I wished her well, offered that I looked forward to speaking with her soon, and asked God to bless her. I called her hospital gift shop and ordered a carved wooden angel to be delivered to her room, as she’s a woman of faith. I had the card signed from me and the Health Dept, so I suppose I’ll find out this week if anyone complained about it. More than anything else, I’m hoping her file shows a successful discharge and recovery by now. She told me she looked forward to trading in the cafeteria food for her son's gourmet cooking, and I pray she's already done that. -
 2020-01-28
2020-01-28IMMY Labs offers POD to help distribute Oklahoma vaccinations
IMMY Labs is a local company in my area that had previously offered free COVID testing to Oklahomans. Starting last week IMMY Labs created a POD at the Embassy Suites in Norman, Oklahoma. This offered senior citizens and healthcare workers the opportunity to receive the Pfizer vaccine and automatically sign up for the follow up vaccination. The POD is processing approximately 1200 people a day. Before many people in my area were driving up to 150 or more miles, roundtrip, to try to get vaccines. This has greatly improved availability for the elderly in my area. -
 2021-01-28
2021-01-28B.C. couple accused of flying to Yukon to get COVID-19 shots face six months in jail
Vancouver couple faces up to six months of jail or fines due to them traveling to the Yukon territory to get vaccinated, skipping the line. The vaccines were reserved for First Nations which have less access to healthcare. -
 2021-01-30
2021-01-30Round Valley Indian Tribes, COVID testing and welfare checks
This is a webpage hosted by the Round Valley Indian Tribes to present COVID-19 testing information (downloadable flyer), procedures to follow to help prevent the spread of COVID-19, and a form to request assistance related to COVID-19 impacts. -
2021-01-14
Vaccine Clinic and Personal Vaccine
I work at the Beth Israel Deaconess Medical Center in Boston, MA. My role is usually in education with a background in pre-hospital emergency medicine. Because of my background as a paramedic, I was asked to work in the vaccine clinic for the hospital staff as an observer. My position was to keep an eye on the hospital staff for 15 minutes after they received their Covid vaccine, just in case there were any reactions. Thankfully, my shifts have been very uneventful due to the safety of the vaccine. It was fascinating to talk with the staff when they came back for their second dose, as I was given insight into their experiences with the first dose. This meant that when I went in for my first dose in mid-January, I fully knew what to expect. I received the Moderna vaccine. About four hours after getting the shot, my arm felt quite sore. By the night of the vaccine, my shoulder was throbbing, but it was manageable. For the price of some shoulder pain, the opportunity to receive the shot during the first wave was well worth the discomfort. I get my second dose in early February, so I will see then if I feel as crummy as some of my friends and co-workers have after the second dose. -
 2020-09-10
2020-09-10Mental Health Care Was Severely Inequitable, Then Came the Coronavirus Crisis
This article describes how the Covid-19 pandemic has compounded the mental health disparity in the United States. As the title suggests, those suffering from mental illness already did not receive equitable treatment; the pandemic has widened this inequality through a variety of issues, chiefly, disruption of service that was already minimal. -
 2021-01-24
2021-01-24SE NM’s Hospital COVID-Bed Capacity
This information displayed on this webpage contains an interactive map with corresponding data summary of the dedicated COVID beds and general capacity of hospitals in southeastern New Mexico for January 24th, 2021. This snapshot demonstrates a reasonably live and present condition of the availability for urgent and emergent COVID medical care within that geographic region and at that date and time. -
 2021-01-23
2021-01-23Change of Life A Friends Story!
I realized the seriousness of the pandemic when I began an exercise program on February 6, 2020. There was not much noise being made about the pandemic yet. I got my nails and hair done on February 11-12, 2020. I would realize now that this would be the last time since I have done this in a year. As the pandemic progressed things were places shutting down and I left my exercise program on February 28, 2020. I early voted on March 2, 2020, and wore a mask. Saw my dentist on March 4, 2020, and got my hair done one last time. By May, I went practically to my doctors and my general physician via telehealth, and then finally I realized this was very serious. People I know began to test positive for Covid. One of these people came into direct contact with me so as a result I went and got a Covid Test as a safety precaution. I found out it was negative. I began to not leave the house now due to the rising cases in my community in Florida. In August cases began to surge even more as people returned to school since summer was over. The holidays came in December and the numbers continued to grow and caused me to not leave the house anymore. This has been a terrible year of isolation and has caused me to lose many dear friends due to the pandemics of isolationism and people's change in attitudes. I am blessed to have a great spouse and a home with a bed to sleep in. I got vaccinated in January 2021. While this brings hope I have to figure out what I am to do and how to move forward as a result of the ongoing pandemic while I have to still maintain safety protocols. I hope the end is in sight due to there now being federal government oversight. -
 2020-07-23
2020-07-23I need to learn not to take work home
A nurse copes with the loss of a patient. -
 2020-12-01
2020-12-01Melrose Wakefield Hospital COVID precautions
One of my coworkers tested positive for COVID-19, so all the employees got tested to ensure we were all being safe at work. I think the photos I captured at Melrose Wakefield Hospital tells a story about all the precautions to stay safe and healthy in an unprecedented time. These photos respond to the needs and considerations of an ethical archive because it shows what precautions are being taken both inside and outside a hospital. In The Ethical Archivist, the author wrote about the ethics of acquisition, which documents have permanent or evidentiary value. I think these pictures may be seemingly unimportant to most people, but to historians this is data that shows what types of mandates and precautions were put in place during a worldwide pandemic. -
 2020-12-10
2020-12-10Nurses in 2020
I think this is an important combination of sources depicting nurses at the beginning of this pandemic, in comparison to how they feel now. My sister, a nurse at a hospital in Los Angeles, California, sent this photo of her to me on March 21st, 2020, smiling and feeling good. 9 months later, she is exhausted, scared, and still working around the clock to help her patients. I think this collection item both demonstrates how significant social media has been with my generation under COVID, as well as being something of interest for future historians to see how devastating the year of 2020 has been. This video of her got 193.3K views on the TikTok app, showing how many people are using the app and watching videos surrounding COVID-19. -
 2020-12-12
2020-12-12Nurse Fighting for Racial Equality in Healthcare
This is a video of a nurse who volunteered to go to New York and help out with the COVID-19 pandemic in hospitals. She was overwhelmed at the number of patients she had that were Hispanic, Black, Latino, and Middle Eastern, and other people of color. It was clear to her that they were being disproportionately affected by this pandemic and chose to march in protests along with them. The acts of Becca Cooper, and the stories she told her audience about, amplify the voices of marginalized groups by speaking out about it and making people aware of these communities and how heavily they are being affected. I think 2020 has also been a year of protests to fight for equal rights and that speaks out to my generation as well. I know a lot of people who have participated in these protests and it goes to show how my generation is standing up for what we believe in, much like Becca Cooper did for her patients. -
 2020-11-24
2020-11-24Conditions in Hospitals
An article from the Globe and Mail about the conditions hospitals workers experience. -
 2020-09-24
2020-09-24Trudeau talks about the importance of health and safety of Canadians right now. Meanwhile...
Nunavut MP Mumliaaq Qaqqaq shares photos of toxic mould from local homes via. Twitter, an issue ignored by the federal government in the wake of other health concerns during the COVID-19 pandemic. -
 2020-12-13
2020-12-13Doctors Can Work From Home Too
A cartoon of a nurse assisting a remote check-up -
 2020-07-20
2020-07-20Nunavut to get $18.9M from feds for COVID-19 response
Health and Finance Minister of Nunavut George Hickes announced the federal government's plan to give $18.9M for testing, PPE, paid sick leave, and COVID relief. -
 2020-11-26
2020-11-26Liberal and Conservative governments have historically underfunded the people of Nunavut. With COVID-19 outbreaks, these historic inequities place them at increased risk.
Reddit post with video of New Democratic Party of Canada (NDP) leader Jagmeet Singh discussing growing COVID-19 crisis in Nunavut. -
 11/20/2020
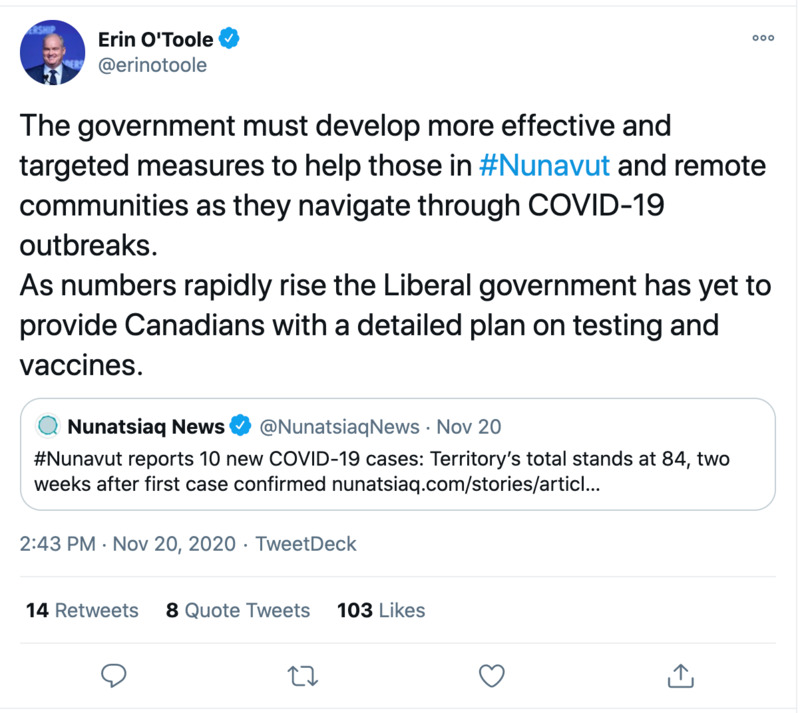
11/20/2020Progressive Conservative Party Leader Erin O'Toole on Twitter: The government must develop more effective and targeted measures to help those in #Nunavut and remote communities as they navigate through COVID-19 outbreaks.
Canadian Progressive Conservative Party (PC) leader Erin O'Toole responds to tweet from Nunatsiaq News reporting 10 new COVID-19 cases in Nunavut.
