Items
topic_interest is exactly
spread
-
 2022-06-16
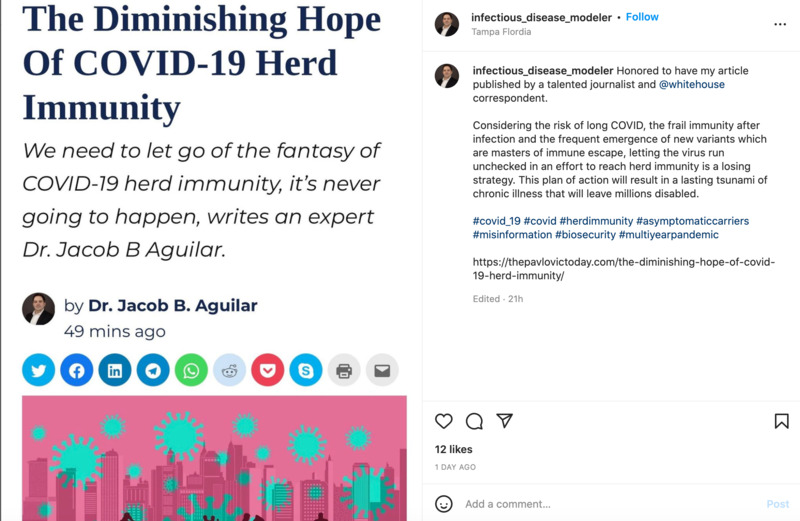
2022-06-16The Diminishing Hope of COVID-19 Herd Immunity
This is an Instagram post from infectious_disease_modeler (Dr. Jacob B. Aguilar).He wrote an article about how herd immunity doesn't work with COVID as well as it could due to new variants that keep on happening. He says that if vaccines had a 100% effectiveness rates across all situations, this would not really be an issue. Since the vaccines are not entirely effective, the solution, Dr. Aguilar proposes that the way to help mitigate the issue is mass regular testing to slow the spread of new variants. -
 2022-04-21
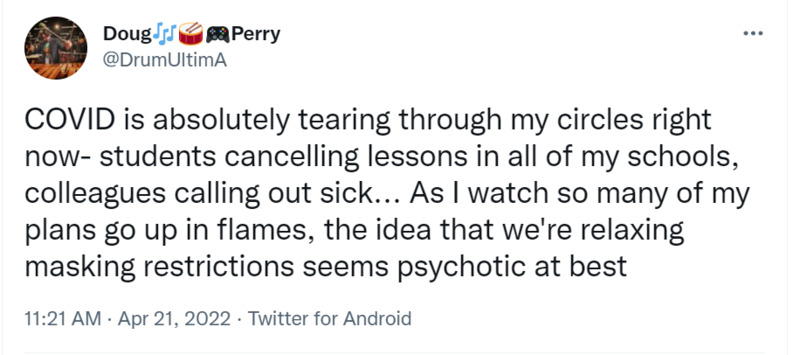
2022-04-21Effects of COVID - even in April 2022
This a screenshot of a Twitter post. In the post, @DrumUltimA describes how even in April 2022, COVID-19 is still having major effects on different aspects of his life. He also points out that he disagrees with so many precautionary measures being dropped. These viewpoints are important as it shows that even though many mandates, regulations, and laws meant to prevent COVID-19 have been lifted, COVID-19 is still around and causing many problems for people. -
 2021-05-26
2021-05-26Covid: Russia starts vaccinating animals
Russia has started vaccinating animals against coronavirus, officials say. In March, Russia announced it had registered what it said was the world's first animal-specific jab. Several regions have now started vaccinations at veterinary clinics, Russia's veterinary watchdog, Rosselkhoznadzor, told local media. Interest has been shown in the Carnivak-Cov vaccine by the EU, Argentina South Korea and Japan, the agency said. While scientists say there is currently no evidence that animals play a significant role in spreading the disease to humans, infections have been confirmed in various species worldwide. These include dogs, cats, apes and mink. -
 2021-07-23
2021-07-23First Race in a Pandemic World
Terrified, I put on my shoes and walked over to the canyon. I’m always nervous before a race - where will I place? What if I can’t finish? It’s adrenaline talking. This time, it was different. For the first time since early 2020, I was competing in a race, outside, with other people. When I signed up, the case count was the lowest it had been since the original shut down. I was nervous, but excited. Then Delta exploded. As the numbers climbed, I tried running with a mask that week. Two days before the race, I made it 3 miles and had to take it off. This was the Hot and Hilly 10K I was prepping for. It’s over 90 degrees and the course is all hills. I knew I wouldn’t be able to do the mask the whole time. I also knew the course had narrow parts, wide enough for only one runner. What happened if I got in a group? Was being outside enough to dissipate the virus, like current advice suggests? Or is Delta more potent? And is there a difference between standing outside unmasked and running full speed unmasked in a group of other people roughly and heavily drawing air in and out? As I waited for the gun, I wore my mask. I was the only one and that didn’t bother me. In fact, I was a little self conscious that I would be judged but I think everyone was just focused on the trail. When the race began, there was a natural small bottleneck. I left my mask on. About a mile in, I had to take it off. Luckily, the crowd had thinned. Since I am not an elite runner, I wasn’t doing the 7 minute miles of the head of the pack. On the flip, I also am not slow. I was able to find a sweet spot where I could see the front of the pack in the distance, but was far enough ahead of the average runners that I was not in a crowd. Overall, it was amazing to be racing again. I love competition. For over a year, I ran only on the treadmill. There was part of me that wondered if my ability have disappeared during the quarantine. I came in 4th place in my division and am beyond excited with that placement. I also was relieved knowing I was done with the crowds for the day. I spent two weeks secretly nervous I contracted COVID and am happy to report that the vaccine seems to have worked for me. I have another race scheduled for October and am already feeling nervous. Our hospitalization rate has shot to nearly 500 and the ICU is two away from 100. Will my next race being outdoors be enough to protect my family, especially my two unvaccinated kids at home? Will my vaccine even still be effective by October? My second shot will have been administered seven months prior at that point. -
 2020-04-07
2020-04-07Bronx Zoo Tiger Is Sick With the Coronavirus
A tiger at the Bronx Zoo has been infected with the coronavirus, in what is believed to be a case of what one official called “human-to-cat transmission.” “There is no evidence that other animals in other areas of the zoo are showing symptoms,” the Agriculture Department said. A pet cat in Belgium recently tested positive for the coronavirus, but the American Veterinary Medical Association said that not enough was known to change the current view that neither cats nor dogs appear to be able to pass the virus to people. The World Organisation for Animal Health says that there is no evidence that cats or dogs spread the disease to humans, but that anyone who is sick should take precautions in contact with their animals as they would with people. -
 2021-07-28
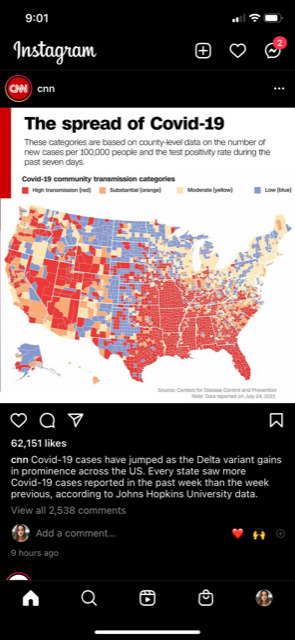
2021-07-28The spread of Covid-19
"cnn Covid-19 cases have jumped as the Delta variant gains in prominence across the US. Every state saw more Covid-19 cases reported in the past week than the week previous, according to John Hopkins University data." -
 2021-07-14
2021-07-14En sólo un día contagios de covid-19 aumentan de 20 a 108 en Coahuila [In just one day covid-19 infections increase from 20 to 108 in Coahuila]
La tercera ola de contagios de covid-19 parece haber llegado a Coahuila, toda vez que de golpe los nuevos casos subieron en las últimas 24 horas de 20 a 108, según el reporte diario de la Secretaría de Salud estatal. En estos nuevos casos se incluyen 9 defunciones, ocurridas en 4 municipios del estado, que son liderados por Torreón en donde se registraron 5 de los decesos; en tanto que Saltillo reportó 2 y los municipios de Nava y Piedras Negras, uno en cada lugar; de ellos, sólo uno no estaba reportado como persona enferma. The third wave of covid-19 infections appears to have reached Coahuila, as new cases suddenly rose in the last 24 hours from 20 to 108, according to the daily report of the state health department. These new cases include 9 deaths, occurring in 4 municipalities of the state, that are led by Torreón where 5 of the deaths were recorded; while Saltillo reported 2 and the municipalities of Nava and Piedras Negras, one in each place; of them, only one was not reported as a sick person. -
 2020-03-15
2020-03-15COVID-19 And Pet Birds
As a parrot owner, I was initially concerned at the start of the pandemic that the virus could be transferred to my avian companions. While I know that viruses are often species-specific, mutations can allow them to jump species. Birds have incredibly delicate respiratory systems, so a respiratory illness in a bird is often deadly. This article from bird food producer Lafaeber explains why caution is warranted by not panic. It is now more than a year since this article has been written, and I am no longer concerned about my parrots catching COVID-19. I belong to many bird groups on social media and have yet to hear of a pet bird who caught the disease. -
 2021-04-04
2021-04-04News Article: How a local response to COVID-19 helped slow deaths on the White Mountain Apache nation
By Amanda Morris of the Arizona Republic: When someone on the Fort Apache Indian Reservation receives a confirmed diagnosis of COVID-19, health care workers from the Whiteriver Indian Hospital jump into action. They personally visit the individual's home to test other household members, perform health evaluations on everyone there and trace any other potential contacts at risk for COVID-19 exposure. Health care workers in the community say that could be one reason why, even though the rate of confirmed COVID-19 cases among White Mountain Apache tribal members is nearly triple the state's rate, the death rate is much lower and continues to fall. Over 90% of COVID-19 cases in the White Mountain community are investigated within 24 hours of testing, according to Ryan Close, the director of the Department of Preventative Medicine at the Whiteriver hospital, which is the only hospital on the 1.67 million-acre reservation. "I feel like what we did made a huge difference," Close said. "We evaluated and admitted people aggressively and early. The tribe deserves an incredible amount of credit for mobilizing staff ... to make this response possible, because at some point it would have been very difficult to maintain without their considerable help." The quick response may have also helped the tribe turn the tide against rapid community spread of the virus, which scientists say could have been fueled by a single variant found only in the White Mountain tribal communities. The variant carried a mutation in the spike protein, which scientist theorize could have made it spread more rapidly than other strains of the virus. The number of confirmed COVID-19 cases among White Mountain Apache tribal members accounts for 24% to 28% of their population, according to Close, but the cumulative death rate among known cases is only 1.2%. By comparison, the statewide rate of infection was 11.5% with a 2% death rate among known cases. And over the winter, Close said the rate for the tribe dropped even lower, to about 0.5%. In a community with a high number of individuals with underlying health conditions, the low death rate and work of the tribe has been "remarkable," said David Engelthaler, director of the Translational Genomics Research Institute's infectious disease division in Flagstaff. The death rate also stands out as unusually low when compared with death rates in other Indigenous communities. Indigenous populations have been disproportionally affected by the pandemic. CDC data shows that Indigenous people are 3.5 more likely to be diagnosed with COVID-19 and almost twice as likely to die from COVID-19 than white people. Close credits a proactive strategy to combat COVID-19 that involved rapid contact tracing, in-person health evaluations and frequent outreach to high-risk COVID-19-positive individuals as well as early treatment with monoclonal antibodies and other antiviral therapies. Volunteers and health workers from the White Mountain Apache community were on the Whiteriver hospital's contact tracing team and high-risk COVID-19 outreach team, which Close said helped the team connect better with the people and work faster. One essential part of the team are the tribe's community health representatives, or CHRs, who are members of the community that serve as a cultural bridge between patients and medical establishments. JT Nashio, director of the Community Health Representatives for the tribe, said the "visceral connection" that CHRs have to the community helps them bring cultural awareness to the way questions are asked for contact tracing, which makes the process more effective and allows officials to better distribute information. "On top of that, quite simply, they know how to get around. It’s a big reservation and not all homes are easy to find," Nashio said. "But when you’ve lived here your whole life, you know where to find people. That became invaluable during the tracing and testing push during case surges." Virus mutation may have made it more transmissible When COVID-19 hit the White Mountain Apache nation, it spread rapidly. The community's first documented case was on April 1, 2020, from someone who had likely recently visited the Phoenix area, unknowingly caught COVID-19 and returned, according to Engelthaler. Within the first few weeks, Close said the community experienced a handful of deaths. "We soon had incidence rates that were skyrocketing. Case counts were going up very, very quickly," Close said. It's unclear why the disease spread so rapidly in the community, but the initial strain of COVID-19 that hit the community carried a mutation that Engelthaler believes could have made it more transmissible. "They were seeing the virus just rip through and have an 80 to 90 to 100 percent attack rate," he said. TGen partnered with the tribe and the U.S. Indian Health Services early on to provide tests to diagnose a case of COVID-19 and provide genetic analysis of the virus from each case. It showed one strain of the virus circulating in the tribal community that wasn't present anywhere else in the state. "This virus moved much faster than anything else we were seeing in Arizona at the time," Engelthaler said. "So we actually believe that we had one of these variant strains in Arizona that was causing very large numbers of cases, but it was secluded and maintained really only in that tribal population." The mutation, called the H245Y mutation, occurred in the spike of the virus, which Englethaler said is a "very sensitive" part of the virus where mutations can have a significant impact. Because of the low death rate, Engelthaler said TGen researchers would like to investigate the mutated strain of coronavirus seen among tribal members to see if it is also associated with a lower fatality rate. He acknowledged that other strains of the virus have since entered the community and that the actions of health care workers in the community and at the Whiteriver hospital is also responsible for the lower death rates. 'The earlier you treat an illness, the better' Close's biggest concern was that an outbreak would cause a "tsunami" of sick COVID-19 patients that would run the risk of overwhelming the Whiteriver hospital, which does not have an intensive care unit. Any patients that require intensive care need to be transported to other hospitals in the state. "We're a small hospital, we cannot take a wave of all very acute patients because there aren't enough ventilators in the hospital," Close said. "There aren't enough helicopters in the state to transport people out from our facility to a higher level of care." Within the first few weeks, Close said the community experienced a handful of deaths, and patients who had the poorest outcomes were the ones who self-presented at the hospital — often meaning they waited until they felt sick enough to go to the hospital. "People don't always bring themselves in early enough," Close said. "The earlier you treat an illness, the better." In response to this phenomenon, the hospital started a high-risk outreach program the third week of April. Health care workers regularly visited the homes of anyone who tested positive for COVID-19 and was at high risk for a poor outcome. Close recalls multiple days when he evaluated patients and found their oxygen levels dangerously low, even though they felt fine. It's a condition associated with COVID-19 known as "silent hypoxia," or "happy hypoxia." "They had no sense that they were even ill. They went on to get pretty sick in the hospital, but they survived and you can't help but think to yourself, 'Yeah, that's a life saved,'" Close said. "That person, if they had stayed home another day or another two days would not have done as well. They would have ended up on a ventilator or something." The Arizona Republic previously reported that the effects of the high-risk outreach program and contact tracing led to a fatality rate among tribal members of 1.6% last June, which was less than the state's rate of 2.5% and country's at 2.7% at the time. But the effect of the outreach program became even more pronounced over the winter, as the tribe and health workers gained access to monoclonal antibody treatments, according to Close. He said the high-risk outreach team started referring patients for antibody treatment in December as part of their protocol after the therapy received emergency use approval from the Food and Drug Administration. Hospital staff at the Whiteriver hospital then administered the antibody treatment. "We give that to people who are asymptomatic or mildly ill to prevent hospitalization," Close said. "The evidence currently suggests that reduces the risk that they're going to get sicker and get hospitalized and reduces the risk that they're going to die." Though there's no data proving the antibody treatments made a difference, Close said that after health care workers started using them, the community's COVID-19 death rate fell to 0.5%. Hospital workers also gave antiviral therapies, such as remdesivir, to patients early and often. "We probably overtreated some people," he said. "But the good news is it definitely led to significant reductions in mortality." Lessons for the future Close believes the different programs were so successful because health care workers were often able to test, trace, diagnose and treat individuals all in the same day — a feat he said was only possible because of how closely integrated hospital workers and community health workers were. "There were no barriers in communication between the public health arm of our response and the clinical care arm of our response," Close said. "It's really a case for an integrated health care system." As the tribe emerges from the pandemic and tribal members get vaccinated against the virus, Close said the hospital may start exploring other health conditions where it can use the high-risk outreach team, which is already trained and experienced in clinical evaluations. "The goal is to take what we've learned from COVID and now apply it to things that are not COVID-related," Close said. Another valuable lesson Close hopes to carry forward is how much of a difference visiting residents in their homes can make and how important building trusting relationships with the community is. Nashio said going door to door to trace and monitor COVID-19 cases was a natural step for CHRs, who had already gone door to door in the past for other community health campaigns. "We know firsthand how difficult it can be to not only connect with patients over the phone but communicate effectively over the phone," Nashio said. "When the community sees their CHRs coming to their door, it helps decrease the stigma of the disease." In addition to performing checkup evaluations and providing information, Nashio said CHRs can also provide food, medical supplies, cleaning supplies or services like grocery shopping and running basic errands. Not every tribal member has reliable internet or phone service, nor access to transportation, so Close said going door to door can be a good way to reach, and help, everyone. "Meeting patients where they are is invaluable," Close said. Amanda Morris covers all things bioscience, which includes health care, technology, new research and the environment. Send her tips, story ideas, or dog memes at amorris@gannett.com and follow her on Twitter @amandamomorris for the latest bioscience updates. Independent coverage of bioscience in Arizona is supported by a grant from the Flinn Foundation. -
 2021-03-24
2021-03-24Mask Mandate
My personal feelings expressed through a meme about how the U.S. Government must have felt about a national mask mandate. -
 2020-12-25
2020-12-25Jesus will understand if you stay home during a pandemic
One of the first things my parents did when they retired and moved to Arizona was find a church. I was very vocal about wanting them to wait to return to large group gatherings but for some strange reason, they seemed to think that they couldn't get covid in church. My mom thought that after all the hardships brought on by the pandemic she needed to be back in church. A month later my dad got sick. We all naively thought it was the flu until I saw the shortness of breath. I told him to get sick and sure enough, he tested positive. Two weeks later my mom contracted Covid. I was hoping it wouldn't hit them too bad but my mom is a diabetic and they are older (late 50's and mid 60's) so I was a bit worried. As the days went by neither of them was getting better. My parents were sick through the holidays, I made Christmas dinner and we ate "together". I dropped off food at their front door then went to their back window where my kids and I ate picnic style. After three visits to the ER for my dad and four for my mom we finally started seeing the light at the end of the tunnel. I have lost many people to Covid, but it never hit me as hard as when I thought I was going to lose my parents. Thankfully, it was a massive lesson learned for my parents that covid spreads even in the church. -
 2020-10-21
2020-10-21masks
I saw this on my Facebook thread the other day and thought it was a funny take on masks and those who refuse to wear them. The cartoon shines a light on the argument about mask and peoples "right" not to wear them. I try to be objective and see situations from different angles but in the mask argument I am dumbfounded by those who refuse to wear them because they feel like its an infringement on their constitutional rights. This country has become so divided because of politics that something as simple as wearing a mask to slow the spread of COVID has become politicized. -
 2020-10-10
2020-10-10コロナ感染予防にリップクリームが効果(2020年10月10日) - Lip balm is effective in preventing corona infection (October 10, 2020)
This is a news talking how lip balms could be effective in the prevention of the spread of COVID-19 virus. 新型コロナウイルスの感染経路の一つであるつばの飛散防止について、リップクリームが効果的だとフランスの研究者らが発表しました。 研究はフランス・モンペリエ大学のアブカリアン教授らが行いました。会話中では特にPやBの発音の際、唇の間に唾液の糸ができ、それがつばとなって空気中に放出されます。しかし、リップクリームを塗ったところ唾液の糸はできにくくなり、人によっては飛散するつばの量が4分の1になったということです。 アブカリアン教授:「もし唇の表面の質を変えたらどうなるんだろうと思いました。研究では、保湿などに使うクリームを塗ると飛沫(ひまつ)の量が減ったんです」 音によって効果が異なるほか、効果自体も1分ほどしか持たないことから、リップクリームはマスクの代わりにはなりませんが、研究を続けていくとしています。 French researchers have announced that lip balm is effective in preventing the spread of the spit, which is one of the infection routes of the new coronavirus. The research was conducted by Professor Abcarian of the University of Montpellier, France. During conversations, especially when pronouncing P or B, a thread of saliva is formed between the lips, which becomes a spit and is released into the air. However, when lip balm was applied, it became difficult for the saliva threads to form, and for some people, the amount of scattered spit was reduced to one-fourth. Professor Abcarian: "I wondered what would happen if I changed the quality of the surface of my lips. In my research, applying a cream used for moisturizing reduced the amount of droplets (himatsu)." The effect differs depending on the sound, and the effect itself lasts only about 1 minute, so lip balm is not a substitute for a mask, but they will continue their research. -
 2020-10-13
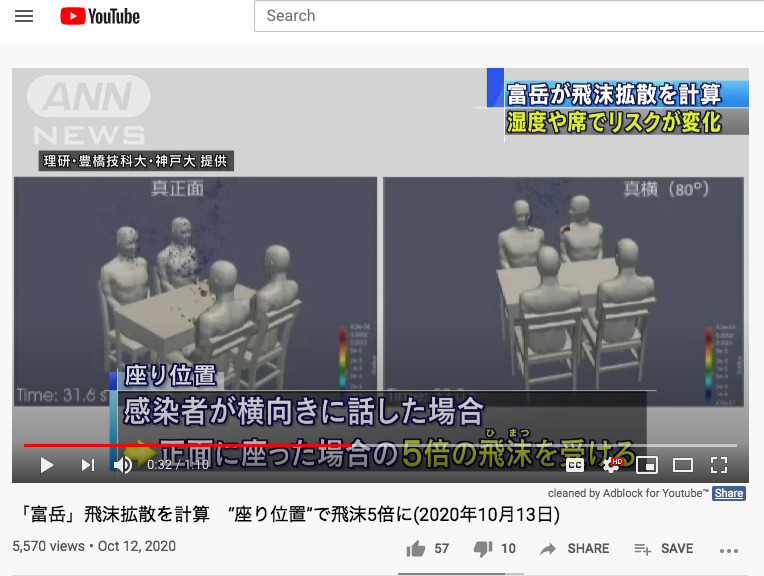
2020-10-13「富岳」飛沫拡散を計算 “座り位置”で飛沫5倍に(2020年10月13日) - "Tomitake" calculated that the depending on the position of the seat, the droplet could be 5 times more (October 13, 2020)
This is the news explaining how droplets travel and the risk of exposure. スーパーコンピューター「富岳」を使った新型コロナ感染リスクの検証で、飲食店で隣同士に座って会話した場合は正面で会話するよりも5倍の飛沫(ひまつ)を浴びることが分かりました。 富岳が4人が飲食店で1分程度話をした場合を計算した飛沫の広がり方です。理化学研究所のチームリーダーを務める神戸大学の坪倉誠教授によりますと、感染者が横に座っていて話をした場合は、正面に座った場合の5倍の飛沫を受けることが分かりました。さらに、飛沫そのものも湿度が低ければ低いほど、下に落ちずに空中に漂う量が急激に増えることが分かりました。湿度30%の場合は、60%の場合の2倍以上の飛沫が1.8メートル先まで到達したということです。また、コンサートホールなどで、合唱をする場合は飛沫は直進するため前方の人ほどリスクが高まるほか、合唱で生まれた気流によって飛沫がより遠くまで届くということです。 In the verification of the risk of new corona infection using the supercomputer "Tomitake", it was found that when sitting next to each other at a restaurant and talking, they are exposed to five times as many droplets (himatsu) compared to when sitting and talking in front of each other. “Tomitake” calculated how the droplets spread when four people talked at a restaurant for about one minute. According to Professor Makoto Tsubokura of Kobe University, who is the team leader of RIKEN, it was found that when an infected person sits next to an individual and talks, he/she is exposed to five times as many droplets as when he/she sits in front of him/her. Furthermore, it was found that the lower the humidity of the droplets themselves, the more the droplets will be floating in the air without falling down. At a humidity of 30%, more than twice as many droplets, compared to the humidity at 60%, reached 1.8 meters away. Also, when a choir is singing in a concert hall, the droplets go straight forwards and thus the risk increases for the person in front, and the airflow created by the chorus causes the droplets to reach farther. -
 2020-08-20
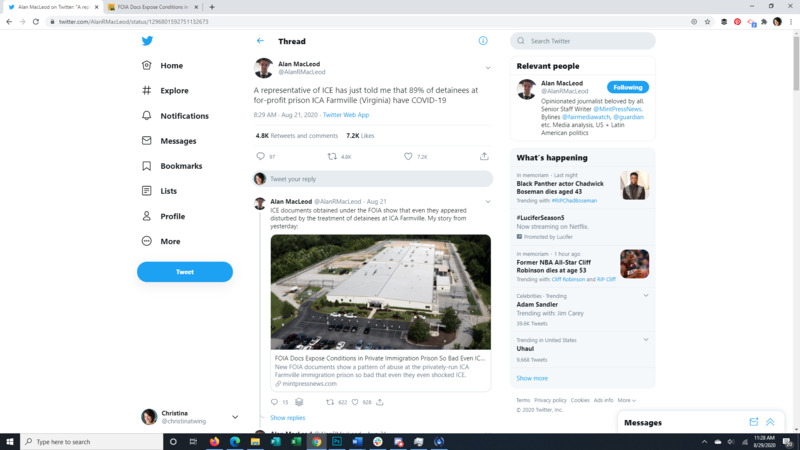
2020-08-20Almost All Detainees Have Covid at Farmville Detention Facility
This Tweet brings to light that almost all detainees at the Farmville Detention Facility, a for profit prison in Virginia, have Covid-19. The attached article discusses long running complaints of mistreatment at this facility, some so egregious that even ICE itself was appalled. It also points to the spread of Covid through facility transfers all over the US. The replies to the original Tweet give a good representation of the American public's response to the situation. -
 2020-07-09
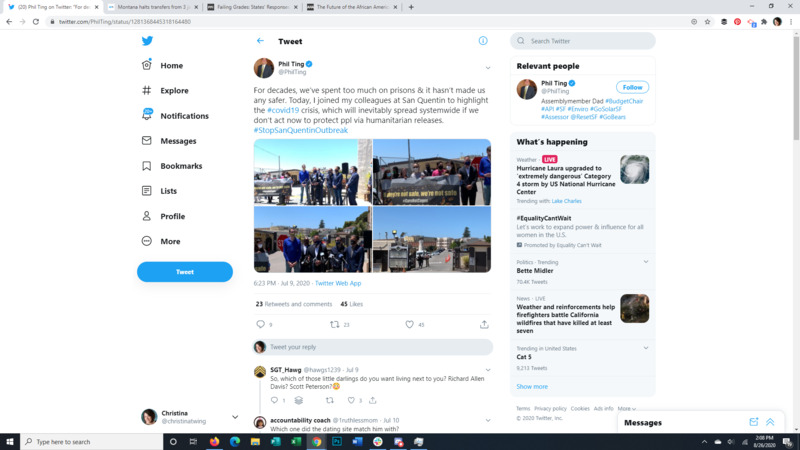
2020-07-09Covid Crisis at San Quentin
This Tweet highlights the activism around releasing incarcerated people to prevent the spread of covid and any sentence from turning into a death sentence. -
 2020-08-06
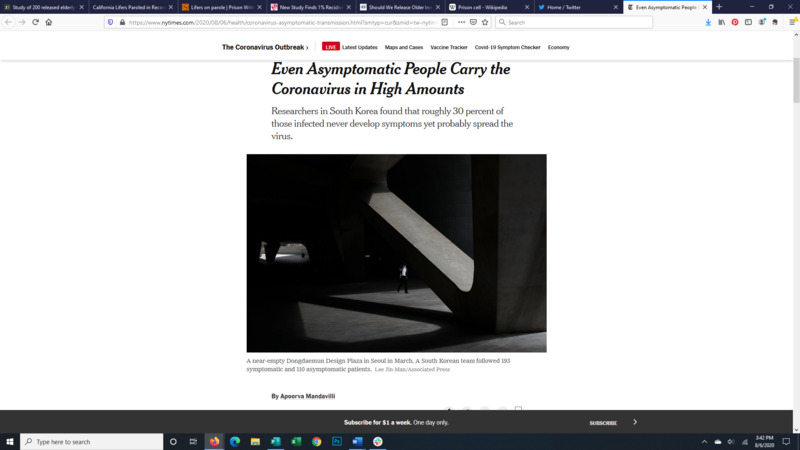
2020-08-06Even Asymptomatic People Carry the Coronavirus in High Amounts
This article discusses the findings of a report recently published in the Journal of American Medical Association explaining that asymptomatic carriers of Covid-19 carry as much virus in their nose and mouth as those with symptoms for about the same length of time. While previously the knowledge on asymptomatic spread was more anecdotal this study offers more direct evidence. -
 2020-06-27
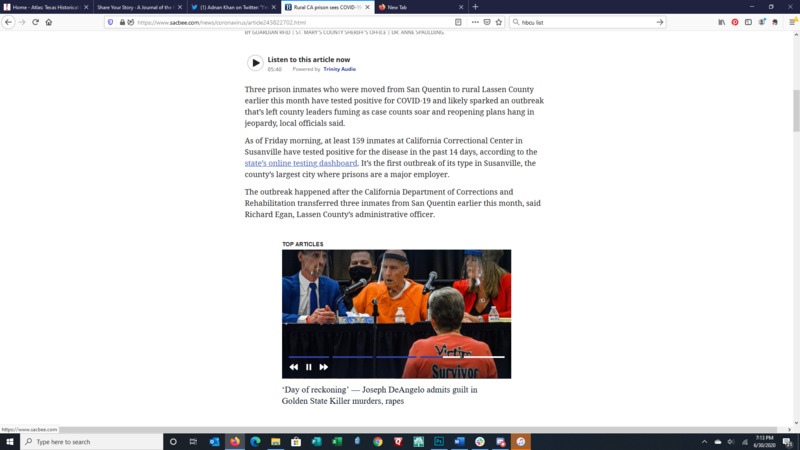
2020-06-27Did Inmates Transfered from San Quentin Spread Covid-19?
These images show a Twitter social media post and the replies it received surrounding the transfer of inmates from San Quentin to other facilities introduced the virus to the other facilities. The author of the Tweet also references an article from the Sacramento Bee entitled "Major COVID-19 outbreak at rural California prison. Officials blame state for inmate transfer" Read more here: https://www.sacbee.com/news/coronavirus/article243822702.html#storylink=cpy -
 2020-06-10
2020-06-10Positive Protest Tests Raises Concern
This article covers so much of what is going on, from protests to Nascar.
