Items
Creator is exactly
Rima Krisst
-
 2021-03-26
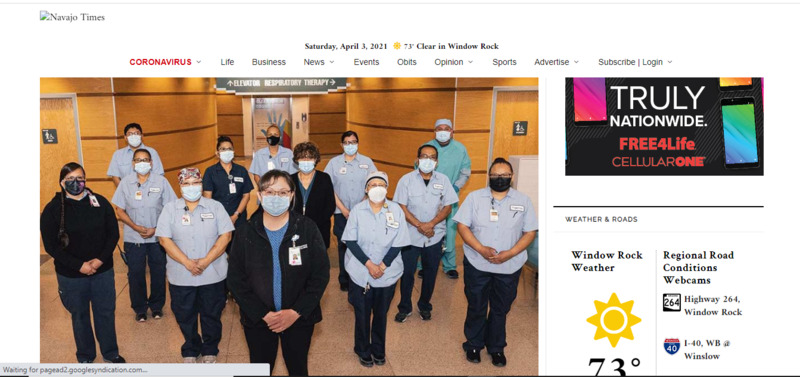
2021-03-26‘They became warriors’: Reflections from the front lines as Tséhootsooí Medical Center workers share experiences
By Rima Krisst | Mar 26, 2021 | CORONAVIRUS, People | Tséhootsooí Medical Center workers share experiences Wilberta “Billy” Jackson, public health nurse III This pandemic has been the longest roller coaster of stress, grief, and loss. I’ve kept my routine simple – sleep, eat, and exercise. And, more sleep. This has been and will probably be the most challenging time of our lives. I could focus on all the bad, but so much good has come from this, from community members stepping up, leaders rolling their sleeves up and getting dirty, how we came together to care for our elders, and so much more. Professionally, we’ve adjusted and readjusted a million times over and completely changed how we deliver health care. We’ve had information, guidance, and policies being added or changing every day and we still were able to deliver health care in a safe, efficient manner. At the beginning of the pandemic, our leaders were warning everyone about the health care system being overwhelmed. Most people thought about it in terms of hospitals running out of beds, but they didn’t think of it in terms of how an underfunded and shorthanded public health force would respond to a pandemic in a rural area with limited resources, and where a population’s most basic physiological and safety needs are not being met. When you don’t have access to clean water, food, shelter and security, you’re not able to prioritize prevention measures until your basic human needs are addressed. The resiliency of the Diné people is unrivaled. The days I’m struggling or feel like giving up, I hear my grandmother’s words, and that’s what keeps me going. And my mother’s surprise delivery of Navajo soul food meals. I’m a public health nurse, so it won’t come as a surprise that I’m excited about the COVID vaccines. We’ve already seen a substantial decline in cases, hospitalizations, and deaths, so we know it’s working. My hope is that our response to the next pandemic or health care crisis won’t be complicated by politics, lack of national strategy, lack of preparation, and misinformation. Stacey Burnside, Primary Care registered nurse What I have learned from this pandemic is to cherish every day and every person that you love. COVID-19 has impacted my family and me profoundly. I lost an uncle and an aunt to COVID-19, and to this day, it is surreal that they are gone. As a primary care nurse, it is difficult to hear about losing a patient to COVID-19, and at the peak, it was almost a daily occurrence… The challenges that I faced during this pandemic were adapting to the changes in work roles and being separated from the people I love. The clinic that I worked in was closed when the pandemic hit the first peak, and I, along with my coworkers, was informed that we had to work in the Emergency Room. The moment that I saw a patient who needed me to be their nurse, despite having COVID-19, humbled me. That moment in the ER humanized COVID-19 for me and made me realize that I was put there for a reason. No matter what the situation is, nurses adapt, and the teamwork and strength we draw upon each other are phenomenal. A huge hit to me personally and professionally was losing a friend to suicide … dealing with grief, loss, and stress has been a daily thing. What has helped me is drawing strength from my God, husband and son, and family. There are many negatives to the pandemic, but one positive that many have seen is the love and strength we have found among our families. I am thrilled that we are at a point of a high vaccination rate in the Navajo Nation. I remember when I administered my first COVID-19 vaccine to a patient, it brought tears to my eyes, and I cried after work. Leah Chattin, respiratory therapist I’ve been a respiratory therapist since 2003. What I experienced throughout the first surge of COVID-19 here on Dinetah is not what you prepare for. I see the impact on my life as deep internal scars that I buried and to resurface those experiences is a nightmare. Imagine the inability to fully take a deep breath, something so simple we take for granted. Supporting my patients with breathing treatments, providing chest physical therapy, changing breathing devices constantly because the demand for oxygen escalates all in a 12-hour or more shift. All these specialized techniques to avoid the last option of intubation, allowing an artificial airway introduced to your trachea with an opening at the tip to provide mechanical breaths from a mechanical ventilator. Fear expressed from my patients was a frequent emotion. You are alone, isolated from your family, your loved ones, no familiar face to embrace, to celebrate your improvement or the worst, a decline despite the battle you have endured. I’d remind my patients not to give up… Instinct took over because I’m a mother too, a nurturer. I can remember softly stroking their hair, holding their hands, shedding tears, praying, putting myself in that empty place at bedside where your family should be gathered, processing the grief. Accepting loss was tremendously difficult. I lost myself because I did not decompress my emotions. My spirit slivered away slowly each time my patients faced rejection of our efforts to sustain life. How I endured and sustained my sanity was prayer requests. Prayer was undoubtedly my saving grace. This virus is fluidic, the path it took was unpredictable. I strongly believe we need to continue wearing a mask, following the CDC guidelines and begin or sustain our health and wellness. Putting into words my experience was not an easy effort, however it’s a pathway for healing. Every COVID patient I battled for will forever have a place in my heart. Sandra Fouser, nurse executive of the Primary Care and Specialty Clinics Seeing the virus cross the ocean and hit the heart of the Navajo Reservation forever changed our lives. As a health professional, I knew venturing into the unknown with limited protection meant some would survive and some wouldn’t. What I have learned working on the front lines – compassion, cohesiveness, companionship, strength, sadness and mental stress. We have been battered, beaten, praised, comforted and have also received recognition from all walks of life. I am proud to be a nurse. I believe the strength to endure comes from resiliency and the people we work with and the support of our families at home. As nurses, we cannot stand still. I feel it is in our blood to help and move forward. I have lost friends, coworkers, relatives and patients. The grief I feel is palpable, almost more than I can handle. Seeing my family, staff and patients suffer through illness and grief has been very challenging and heartbreaking. As a team, I believe when something happens to one of us, we all feel the effects, we grow closer and find comfort in each other. I see the vaccine as a progression toward eradicating the detrimental effects of this virus and giving us hope that there is a better tomorrow and that Hózhó will be restored. Dr. Karen Williams, hospitalist physician I am a Native physician (Mountain Maidu/Apache) and Indian Health Service Professional Scholar. When the pandemic started our hospitals were suddenly overwhelmed with large numbers of very ill patients needing oxygen. Some patients who worsened were placed on a “life support” or ventilators since they could no longer breathe on their own. Despite our best medical management efforts, including use of high-flow oxygen, there were patients who did not survive. I witnessed more death in a year than I have ever experienced in my career. This was traumatic for me because every day I came to work I felt like I was coming into a war zone. We saw people struggling to breathe and fighting for their life. We heard family members saying their goodbyes to their loved ones and crying over the phone. We held hands of those who took their last breath and witnessed co-workers not able to control their tears. If it were not for our team efforts, almost a military-style mentality, we could not have managed. As a hospitalist physician, the biggest challenge was ensuring that I had the most up-to-date medical knowledge to save a patient’s life. During the beginning of the pandemic many doctors throughout the country did not feel prepared. This was quickly overcome by learning medical strategies used by doctors throughout the world. The treatments used included steroids, anticoagulant medications, and high-flow oxygen. We had the support of our hospital’s incident command leadership and adapted to the changes. This included being able to offer our patients who needed oxygen a federal Drug Administration-approved “emergency use” medication called Remdesivir, and more recently Bamlavinimab for non-hospitalized patients My experiences on the front lines were psychologically and physically overwhelming … I sought support from elders and used my Native spirituality for strength. I also sought protection support from traditional Indian practitioners who set up a tipi and hogan outside the hospital for employees. I sometimes thought twice about the danger I was in. However, I acknowledged that I would never walk away. This is a result of my obligation to the Native community and the hundreds of patients I had gotten to know for so long. I “warriored up” in my mind and sought to do the best I could. I do not foresee an end to mask wearing, and now recognize how careful we all must be to protect each other. I saw too many elders get severely ill and even pass away from COVID as a result of young family members not being careful and bringing it home. I have encouraged community members and my own family to get the vaccine as soon as possible. I received two doses of the Pfizer vaccine and said a prayer in my Native way each time for protection. Natasha Topaha, certified medical assistant, Mobile Unit Overall, this year has been extremely challenging, but also has reinforced my personal strength and resiliency. I have had ongoing concerns throughout the epidemic regarding my kids’ isolation and their mental health. It has been difficult, but doable, to manage both working in health care and supporting my family both emotionally and physically. I had constant worry about bringing the virus home and infecting my family given that I was working in high risk areas and providing COVID testing, vaccines and social and mental health support to patients. I found that doing outdoor activities with my family, such as bike riding and hiking, helped me ease my stress and helped teach my children some healthy coping skills. And we could spend time together! I feel very happy and grateful in both receiving the vaccine and being able to provide it to patients and the community. I feel safer at work and at home now. Johnny Willeto Jr., facility manager/logistics chief The strength to endure comes from within yourself. For me this began in my childhood as the son of Delphine Damon Willeto and Johnny Willeto Sr., who nurtured me to become a great human being. They taught me to be a courageous, productive worker and know my limitations. As a facilities manager, my main focus and responsibilities are the protection in the physical environment of all who walk through the doors of Fort Defiance Indian Health Board’s facilities. All we knew is that COVID-19 was airborne and surface communicated. I treated it as you would tuberculosis and ensured that my staff had adequate PPE to help protect them when they are tasked with working in the patient care areas. This responsibility was a big challenge when trying to procure medical equipment such as masks, gloves, safety glasses, gowns, scrubs, and so forth. Having an MBA has allowed me to flourish in this high stress environment and to adjust with adaptations to finding supplies and creating new relationships with trustworthy suppliers. Being in close proximity to patients who are struggling with getting well can be heart wrenching. Being able to fulfill my duties in the support role to the best of my ability for my community and teammates has allowed me to sleep well at night knowing that I gave it my all. I have lost a brother-in-law who contracted the virus in the Scottsdale area of Arizona. These were very difficult times because as Navajos we are accustomed to comforting each other by a hug or handshake. With COVID, gatherings are not safe, so having family meetings for planning the funeral is off and also the funeral usually consists of 10 minutes before the burial with only a few close family in attendance. One of the biggest assets I have gained is the spiritual belief in God and keeping the communication open by saying my prayers often – to be thankful for the blessings that have come my way or when asking for strength to endure the hardships. In my free time I isolate on the Willeto Sheep Ranch in Goatsprings Valley, Arizona, where I tend 120 sheep and goats. Being able to separate the everyday stress and recharge is paramount to going forward with courage and mental sharpness to make the right choices for the organization, patients and employees. The vaccines are an effective tool to help reduce the mortality of the virus on us and give us protection to this invisible enemy. Corinne Legah, Environmental Service supervisor Personally, I was scared when I first heard of the spread of the virus overseas. It was shocking how fast the virus traveled. In the beginning our team was needed to help keep the hospital sanitized and safe for patients. We reinforced training on the cleaning process for the airborne/droplet virus. I constantly stressed wearing PPE and hand washing. I am so proud of the team for stepping up by protecting our patients. They became warriors to fight the virus. I believe without my husband’s support and God I would not have been able to cope. I have lost friends and family from this virus. It saddens me that many of our people are now in the spirit world. Being a Native and growing up with Navajo beliefs, I had to be strong. My ancestors went through so much and our people are resilient. Prayer is our strength. I cried when I watched the news when the vaccine was given to the first person in the U.S. If everyone gets their vaccine we will be able to interact with family again. I am looking forward to that day! -
 2021-03-09
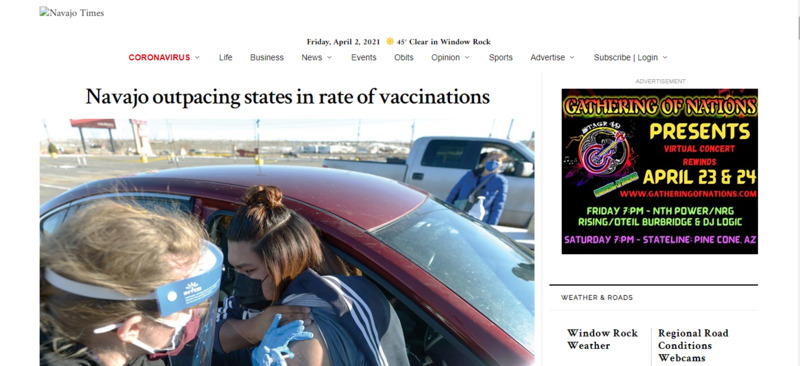
2021-03-09Navajo Nation outpacing states in rate of vaccinations
By Rima Krisst | Mar 9, 2021 | CORONAVIRUS, News | WINDOW ROCK President Jonathan Nez proudly said last week that the Navajo Nation had exceeded its goal of administering 100,000 COVID-19 vaccine shots by end of February, crediting tireless health care workers who have been serving seven days a week to plan vaccinations and administer the vaccines. On Tuesday, the president’s office reported that 135,161 COVID-19 vaccine shots have gone into arms on the Navajo Nation, which represents 92% of the total 146,980 doses received and includes 48,800 persons who have had their second shots. This means that over 26% of the approximately 327,000 enrolled Navajos have gotten a shot through the Navajo Area Indian Health Service and tribal health care system, which is an amazing feat. By comparison, in New Mexico 22.4% of the population (738,705) has been given at least one shot. Arizona has administered at least one shot to 17.1% of the population (1,847,750), with Utah trailing behind at 12.2% receiving at least one shot (687,925), according to the CDC data vaccine tracker. And as of March 2, 15.3% of the U.S. population had received at least one shot, with 76.9 million shots administered, including 25.4 million receiving the second dose. Approximately 1.8 million vaccines per day are being administered daily in the U.S. So, percentage-wise, Navajo is outpacing both neighboring states and the general U.S. population. ‘Amazing partnership’ On a Feb. 25 IHS media call, IHS Chief Medical Officer Rear Adm. Michael Toedt reported that as of Feb. 18 the IHS had also achieved its goal of administering 400,000 doses of COVID-19 vaccine “across IHS, tribal, and urban Indian Health programs,” representing 16% of the “target population,” with 6.3% receiving two doses. “This milestone was reached ahead of schedule despite severe weather, making travel to health facilities difficult across much of Indian Country and leading to shipping delays,” said Toedt. Toedt said most IHS facilities have now vaccinated the majority of their priority populations and are moving into Phase 2, which includes those who work in higher risk settings such as schools and prisons. “Very shortly we expect that everyone who needs a vaccine will be able to receive it,” he said. Toedt credited IHS and tribal health care employees across the country who are committed to ensuring the protection of tribal communities in 11 geographic areas covering 26 states and 349 health facilities, many in rural and remote locations. “We have had an amazing partnership with our tribes to use all available resources to help with delivery of vaccine,” said Toedt. This included distribution and redistribution of vaccines by ground and air transportation as needed. Toedt said the IHS has also conducted over 2 million COVID-19 tests at a higher per capita than most states and is reporting a seven-day average test positivity rate of 4.5%, below the 5.6% all-races rate in the U.S., despite the fact that COVID-19 has had a disproportionate impact on American Indians/Alaska Natives. The Navajo Nation has conducted 245,085 COVID-19 tests resulting in 29,774 positive cases. ‘Developing trust’ Coordinated public relations campaigns in partnership with tribes have been key to the success of the vaccine rollout, said Toedt. Navajo Area IHS Chief Medical Officer Loretta Christensen agreed, saying public messaging has been critical. “This collaboration is one of the reasons we’ve been extremely successful,” said Christensen. “Honesty and transparency, developing that trust with the people you are serving is vital. We have spent a great deal of time on that relationship with our Navajo people to encourage them to be vaccinated.” She said the communication process has been very unified across Navajo and with the president’s office, using social media, radio, and a bilingual approach. “This is constant public education,” she said. “We encourage people in a very personal way that we would like them to be safe, keep their families, their communities safe. We feel very fortunate and grateful that our population has really stepped up.” Toedt acknowledged there has been some vaccine hesitancy relating to how quickly the vaccines were developed and whether or not they are completely safe, which has made some people distrustful. According to IHS Public Affairs Specialist Joshua Barnett, a recent IHS-funded survey by the Urban Indian Health Institute reported that 75% of Native Americans were willing to get a vaccine and 74% believe that doing so is their responsibility to help protect their community. “I’m confident that the process for vaccine development has the full integrity and completeness of time necessary to make sure these vaccines are safe, but it’s our job as healthcare providers to communicate that in a way that’s acceptable and trusted by our population,’ said Toedt. “We know our efforts are working and we’re seeing good delivery and acceptance of these vaccines in our communities.” Reaching the homebound Christensen said one of the strongest assets in the Navajo vaccination campaign has been the collaboration between public health nurses and community health representatives in reaching out to community members at the local level, including homebound elders and persons with disabilities. “These are the people out in the rural areas that know the families, that know the homes,” said Christensen. “We rely on them for that person-to-person contact out in the communities.” She said between 4,000 to 5,000 homebound individuals have actually been vaccinated at home or close to home. Moving forward with the goal of getting the Navajo population vaccinated and achieving “community immunity,” Navajo Area IHS wants to make sure that all 27,000 square miles of the Nation have been penetrated, said Christensen. “We want to be able to target any communities, populations or subgroups that have perhaps maybe not been able to get vaccinations,” she said. “So, our first step is to heat-map our whole area and then focus on those populations that are perhaps more rural or don’t have easy access to healthcare facilities.” “Our goal is to get every single person vaccinated and to keep our populations in Arizona, New Mexico and Utah safe,” she said. Christensen said her team will be working with chapters to identify anyone who might have been missed. They have also reached out to Navajos living off reservation and have established an online registry to help people find a place to get their vaccination. “We highly encourage them to come back if they need to and we will certainly take care of them and their families,” she said. Tracking variants In regard to surveillance for COVID-19 variants, Toedt said IHS does contribute its tests to state public health labs as well as different large lab corporations such as TriCore, LabCorp. and additional processes for genomic testing are in development. “The samples that are included through those mechanisms are sampled through the CDC’s processes to test for genomics,” said Toedt. Christensen said similarly the Navajo Area and the Health Command Center are working to establish more specific genomic surveillance within Navajo Nation. “In the meantime, we are participating in testing both in New Mexico and Arizona,” said Christensen. Christensen said the Navajo Epidemiology Center has also reached out to bordering states requesting any relevant information on variants be shared. “We all stand by ready to support this process and we are hopeful that we will have more specific information for Navajo Nation very soon,” she said. Christensen confirmed that she was not aware of any variants having been identified on the Navajo Nation from random sampling. “We have requested that information but we have not received it as of yet,” she said. Adverse events Any adverse events, or serious side effects, related to vaccinations within IHS are collected and reported to the same CDC system that collects the data nationally, said Toedt, but the data broken down by individual tribes is not publicly available. “We are part of that Vaccine Adverse Event Reporting System through the CDC,” said Toedt. “All adverse drug reactions are investigated by the CDC to determine what category it goes in and how they analyze data.” Navajo Area is gathering information on any adverse events on the Navajo Nation, but there are patient privacy issues when it comes to sharing that publicly, said Christensen. “We do, as (health care) institutions across Navajo Nation, share basic data with each other when we’re doing best practices,” she said. Christensen would not answer whether or not there had been any adverse events on the Nation. “I will say we have done very well with these vaccines,” she said. “There are certainly side effects which have been well defined, but we’ve had minimal significant adverse events. I cannot quantify that for you, but we are tracking those events across Navajo Nation.” Preventing transmission As far as keeping everyone safe after being vaccinated, Toedt said it’s still important to continue to wash your hands, stay six feet apart and to wear a mask. This is because vaccinated persons can theoretically still contract COVID-19 and spread it after being vaccinated, although they may not have any symptoms due to protection from the vaccine. There are also still many unknowns related to COVID-19 variants and to what extent they may evade vaccine protection, be more transmissible, or cause more serious disease. “We have been trying to report on possible variants most recently, explaining that we don’t have all the information yet on what the long term effects of those variants are,” said Christensen. “So we highly suggest that you still watch your distance, wash your hands and wear your mask.” Christensen said public messaging encouraging everyone to abide by the public health protocols in place, regardless of vaccination status, will continue until there is community immunity.
