Items
Tag is exactly
Healthcare
-
 2021-03-18
2021-03-18Disparities in Healthcare during Covid-19
This article is about the disparities in populations that have been impacted by Covid-19. The CDC found that American Indian, Alaska Native, African American, and Latino people were almost three times higher than non-Hispanic white people in hospitalizations during the pandemic so far. These numbers are, unfortunately, more a reflection on our healthcare system as a whole, not just specific to Covid. Dr. Felicia Collins, a distinguished graduate of Harvard Medical School, is the keynote speaker at the 2021 Alvin F. Poussaint, MD Visiting Lecture and will be discussing these healthcare inequalities. On top of having an MD, Dr. Collins also has a Master's in Public Health (also from Harvard), which gives her a unique perspective into healthcare at the individual and population levels. Analyzing healthcare data through the lens of a physician must give her the ability to contextualize healthcare disparities in a way that others would not. This sounds like it will be an interesting lecture on a very important topic, and will of course be held over zoom. -
 03/13/2021
03/13/2021Covid-19's Effect on LGBTQ+ Community in NYC
Interview with Krystal McRae -
 2021-03-01
2021-03-01Native Hawaiians and Pacific Islanders, Vaccinations
When we say end violence against our elders, this means demanding accessible, equitable and culturally responsive healthcare services for them. Here are some community-based resources who have been doing this work: @pacificislandercovid19 @picawashington @empoweredpi Thank you Seattle Times for amplifying how COVID and inequitable health care services impact our communities in Washington. The impacts are detrimental and NHPI communities are impacted at disproportionate rates. Check out the entire article @seattletimes. Some things this article highlights - vaccine services provided need to be inclusive of different cultural lifestyles and practices, lumping Asian and NHPI data together invisiblizes NHPI needs, there is a great need to bring community-based groups to the table to build accessible systems and solutions. (Image description: a carousel of 9 slides from an article by Seattle Times. 1. A front page article that reads to fight covid-19 with vaccines, native Hawaiians and Pacific Islanders in Washington first need to be seen. 2. A quote in simple black text that reads "that is one of the things that we continue to think about How do we honor those that have passed during the pandemic? Our elders have so many stories, so much knowledge and they're essentially the wisdom keepers of our culture" seia Said. 3. The numbers tell the devastating story. Native Hawaiians and Pacific Islanders make up about 1% of Washington state's population but account for 2% of cases in the state according to the State department of health native Hawaiians and Pacific Islanders have the highest average rate of any race and ethnicity in the state at $7,132 per 100,000 people and also lead in deaths per 100,000 with an average of 151 as of February 21st, according to the UCLA Center for health policy research" Captions continues in comments. #InSolidarity #AAPIWomenLead #COVID19 -
 2020
2020Caulfield Elementary School
A socially distanced classroom at Caulfield Elementary School in British Columbia, where in-person classes are allowed to take place in a modified fashion -
 2020
2020British Columbia Mask Mandate
Sign outside a Chilliwack business stating that masks must be work upon entry -
2021-03-06
This is not how this is supposed to go.
Friday, March 13, 2020, was my last full day in the office before the shutdown. We came home that night not knowing what was next. Then my sister called. Things hadn't been right for a couple of weeks, she said, and when she had been to the doctor that morning he ordered her directly to the MRI lab. And there it was. Cancer. The exact same kind that had taken our mother a few years ago. And our grandmother several decades ago. Dammit. So what do you do? You get on a plane, you go there tomorrow, and you face this thing together, as family, right? Except no. It's COVID time, and only one person was even allowed to accompany her to the hospital for surgery three days later. We all decided that my other sister should be there, since she has medical expertise and also a more flexible schedule. But yeah. Here I am, on the other side of the country, not knowing whether my sister would live through the day and not able to go be with her. It's a year later, and I'm very relieved to say that she's still with us, lasting far longer with this diagnosis than either our mother or grandmother did. Still very much in the fight. But thanks to this damned disease, and to everyone whose stupidity has caused it to last longer and be worse than it had any need to be, I have seen her exactly once in the last year. For about ten minutes. Right before her second surgery. Will I get to see her again? Who knows? We have a trip planned in a few months, if things get better with this pandemic. And if she lasts that long. It's sad and exhausting and infuriating and unchangeable. -
 2020-06-11
2020-06-11Taking Charge
COVID has definitely impacted all of our lives. Despite all the damage it has caused, the virus had some positive consequences. Some of us developed closer relationships with our families. Many of us found new hobbies and developed new passions. For myself, I found a passion for healthcare. Hearing stories and watching news reports on the chaos occurring in our hospitals, made me feel impotent. So, after 3 semesters away from school, I decided to come back and focus on finishing my bachelors so i can enroll in a nursing program. -
 2021-02-25
2021-02-25Disparities in Black Americans receiving the vaccine
As is common with many other facets of BIPOC receiving access to healthcare in westernized countries black people are falling behind their white counterparts in receiving the vaccine. Only 5.7% of black U.S. citizens have received the vaccine as compared to 11.3% of white U.S. citizens. The disparities reflect a general inability for black people to receive adequate care in the United States while white people are generally able to receive a higher level and more care. Vaccines are especially important with regard to COVID as it represents a path back to normal life. Black people are receiving the vaccine at a rate almost half of that of the next racial group. -
 02/22/2021
02/22/2021Layne Williams Oral History, 2021/02/22
This interview is with medical profession Layne Williams who speaks about a positive aspect of the pandemic they noticed. -
 02/21/2021
02/21/2021Nancy Carter Oral History, 2021/02/21
This is a mini oral history that I did with Nancy Carter, my mom, about silver linings -
 2020-04-17
2020-04-17COVID-19 and Social Justice
From the article: The COVID-19 pandemic is a health and mental health crisis, to be sure. But it is also a crisis of social injustice, inequitably affecting vulnerable and marginalized populations that include, among others, individuals who earn low incomes, or are incarcerated, homeless, in foster care, over 65 (especially those in long-term care facilities), people of color, or undocumented. Social work practitioners, educators, and policy makers are working to address the needs of these populations despite the unpredictability of the virus’s secondary impact on systems. -
 2021-02-15
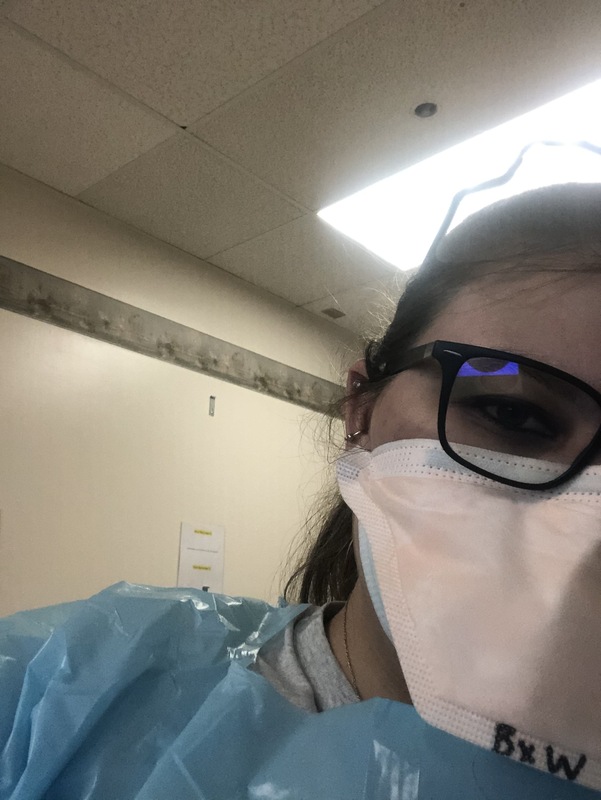
2021-02-15Getting My BSN in COVID Land
The start of the semester was like that of any other except last semester I managed to secure an internship for the summer of 2020. Nursing school was already a difficult major to be in and I really didn’t think that it could get more difficult than that of junior year. I truly didn’t know what was to come. I will never forget being at clinical and hearing everyone mention the start of the virus. COVID-19 was on the backburner when it came to the most interesting topics of January 2020, but it would soon prove to be the most prominent in the upcoming months. I distinctly remember shadowing a nurse in the ICU one day and hearing the nurses discuss what was going to happen. “It doesn’t seem like it is coming here but trust me it is and when it does, we will need all the healthcare workers we can get.” This was a statement from one of the nurses that I will never forget hearing. At the time I didn’t fully believe the things that I were being rumored and didn’t think that we would ever be where we are today. As February and March arrived, COVID came to be part of everyone’s lives. Turning on the news, checking your timelines, and most day to day conversation held the topic of corona virus. Before we knew it, our lives changed completely. Our clinicals and classes were held remotely, you couldn’t leave your house without a mask, and we weren’t sure if we were going to be able to attend our internships. One thing that worried a lot of us was working while the virus cases began to spike. I knew that I would continue working as I was if not more than usual. Over the course of my internship I watched as COVID began to impact all the healthcare workers I was surrounded by. Safety precautions in the hospital setting were changing and at first, a lot of people were afraid to come in for their illnesses for fear of encountering a positive COVID patient. As time went on people became less and less afraid to come seek help at hospitals. With a large influx of patients coming in I could see nurses, aides, and doctors among others all begin to take the toll of the virus. This wasn’t necessarily due to exposure but more so that our exhaustion kicked in. Health care providers were and still are working countless hours to help in high census situations. The most frustrating aspect of quarantine has been watching people be noncompliant with mask requirements and stay at home orders. I wake up for work everyday and risk the wellbeing of everyone in my home including myself to help take care of those who need it. As the media has portrayed us as frontline workers, it felt slightly misleading while some of the public wasn’t contributing to lessen the blow of the ongoing problem. I started my internship to gain experience for my career. I didn’t know that I would grow accustomed to death and grief as fast as I have in the past year. COVID has shown me what it means to work hard and what struggles I can encounter in my career before I have even graduated and hold my diploma in hand. I currently work on the same unit I held my internship on as it has been converted into a COVID care unit. I go into work and experience exposure situations day by day but wouldn’t change my career for anything. The corona virus has taught me so much about what it means to be a nurse and take on healthcare as a career. In a few months as I graduate I will be prepared to take on whatever challenges it may have. -
 2020-12-23
2020-12-23COVID-19 The Good, The Bad, and The Deadly….
COVID-19 The Good, The Bad, and The Deadly…. When the COVID-19 pandemic struck I was in the spring semester of my second year of nursing school. Being naïve and not having experienced a pandemic before, I expected COVID-19 to breeze in and out like the flu every year. What I didn’t expect was a deadly virus that would leave behind it a path of death, despair, and devastation. One of the biggest areas in my life that was impacted by COVID was my education. As classes moved to virtual platforms there was a major learning curve for both students and professors. CDC guidelines and social distancing made it difficult to find areas on campus to study and next to impossible to study in groups. My friends and I worried about our lack of clinical experiences and how that was going to impact our future. Since I had virtually no clinical hours during my specialty rotations, not only was I unsure of my skills, I was also unsure of where I wanted to take my nursing career. Returning to work over winter break was also very challenging. I am a patient care assistant and medication technician at an assisted living facility. All throughout the summer I worked with the threat of COVID looming above my head like a dark cloud. It was the first time in my life that I felt people really depended on me. I understood that my actions impacted the health of others. Fortunately, my residents all remained safe. However, I was not prepared for my return a few months later. The residents were no longer allowed to have visitors and they started testing positive for COVID. At one point we started to run low on personal protective equipment, but we were still trying to take all the precautions that we could to keep us and our residents safe. It was heart breaking to be the one holding a residents hand as they passed away due to coronavirus. My job became a lot more difficult having to communicate with families and watching their final moments with their loved ones. The residents that were lucky enough to not contract the virus were lonely and couldn’t understand why they had to quarantine. They felt abandoned and afraid. It was a very trying time for all my coworkers since we were all working overtime due to our staffing shortages. Working overtime was both physically and mentally draining. Even on my days off I was called in because staff members were getting sick and were unable to come in. It was mentally exhausting because every day I would come in to work and be nervous to walk in to report and see who had passed in the hours I was gone. COVID-19 also brought about some remarkable changes. I have spent a lot more time with my family as we have discovered our new passion-hiking. My co-workers and I have a new appreciation for one another and take the time to have meals together and support one another to make sure we are doing okay mentally. I have been part of innovative changes like my COVID-19 remote patient monitoring job and positive experiences at the COVID vaccine clinic. I have seen the medical and scientific communities collaborate on treatment guidelines and the development of a vaccine. It has also been an incredible period for change and innovation. -
 2021-02-08
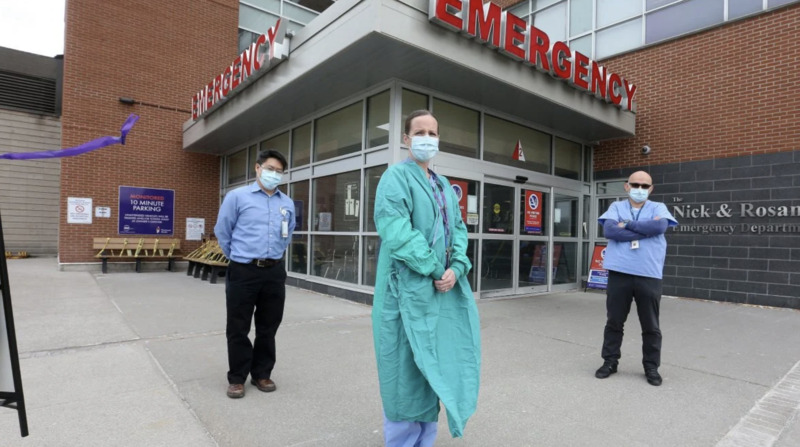
2021-02-08Recognize Their Courage and Sacrifices
Evaluating the financial impact of the pandemic on the country, House representatives are asking the government to remember and acknowledge those working on the frontlines and their families. The Bloc Québécois demands the government "significantly and sustainably increase Canada health transfers before the end of 2020." -
 2021-02-02
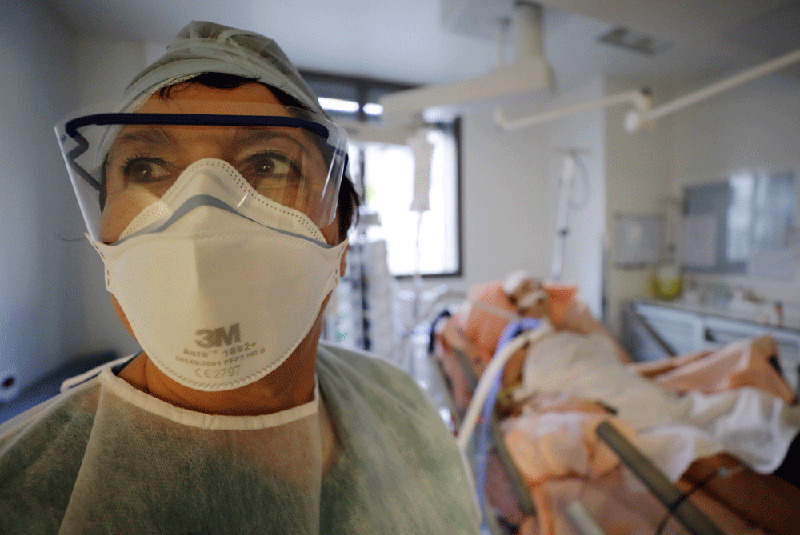
2021-02-02Inadequate Sick Leave Jeopardizes Canadian Health Workers and Patients
Due to inadequate medical supplies, lack of vaccines, and inability to slow down the spread of the virus, the pandemic rages on. To make matters worse, over half of Canadian workers lack sufficient sick leaves, which contribute to more outbreaks and the dangers of contracting COVID-19. -
 2021-02-07
2021-02-07Supporting Healthcare Workers with Meals & Food Services
Everyone can surely agree that healthcare workers are our everyday heroes. Healthcare workers are the ones who had voluntarily trained and continue to medically assist those who need it without discrimination. All this while risking their own safety and well-being during a deadly pandemic. They are no strangers to long work hours while also having to always stay alert and ready, because quality care can greatly influence someone’s life. Due to most of their time taking care of patients, one can easily see how it can drain their own health as well. Hospitals are not exactly known for their top tier food options either. For these reasons, organizations like Meals for Heroes had worked with food services to help these essential workers with their meals. With the COVID-19 pandemic closing many businesses as well due to safety regulations, we have also been seeing the same businesses (as well as bigger ones) pitch in with meals and more affordable meal plans. Some places are even giving healthcare workers food for free. https://www.uab.edu/fightcovid19/impact/meals-for-heroes https://alabamanewscenter.com/2021/01/20/meals-for-heroes-will-continue-serving-meals-to-frontline-health-care-workers-fighting-covid-19/ https://www.thrillist.com/news/nation/free-food-for-healthcare-workers -
 2021-01-07
2021-01-07THE COLOR OF CORONAVIRUS: COVID-19 DEATHS BY RACE AND ETHNICITY IN THE U.S.
This data sheet looks at the affects of Covid-19 mortality rates by race in North America. They do not interpret the data but the site says the following: We call on state and local health departments to release timely data about COVID-19 deaths with as complete racial and ethnic detail as is possible. As the data reporting improves, so too will our understanding of the devastating impact of this disease. This will inform states and communities about how to direct resources more equitably as well. -
 2021-01-28
2021-01-28B.C. couple accused of flying to Yukon to get COVID-19 shots face six months in jail
Vancouver couple faces up to six months of jail or fines due to them traveling to the Yukon territory to get vaccinated, skipping the line. The vaccines were reserved for First Nations which have less access to healthcare. -
 2021-01-27
2021-01-27OC health care worker dies after receiving 2nd COVID-19 vaccine shot; official cause of death pending
With any rushed medical treatment unforeseen consequences can occur. As the vaccine is released in the 10s of millions I pray Tim Zook's story is a completely isolated incident. -
 2021-01-25
2021-01-25"The Pandemic Is Finally Softening. Will That Last?" - The Atlantic
This Atlantic Monthly article, written by Robinson Meyer, details the race to vaccinate millions of Americans in the face of loosening mitigation efforts, new COVID-19 strains, and supply bottlenecks. According to Meyer, with the advent of several COVID-19 vaccines, some states and municipal governments across the country have loosened their quarantine restrictions in the belief that vaccination and lower death rates make lockdowns unnecessary. This is not true, and this loosening of restrictions may precipitate further surges in COVID-19 cases, especially as new strains from the UK and South Africa become endemic. Fewer vaccine doses will be delivered by Pfizer, due to an agreement signed by the Trump administration. -
 2021-01-25
2021-01-25Vaccine Localism Defines Who Belongs
This article says the NH state government has changed its policy to define NH residents for vaccine purposes as NOT including second home owners, non-resident landlords, and other non-full-time residents. This matches policy in Vermont and Maine, both of which have cited vaccine scarcity as a reason to prioritize their own full-time residents (and presumably voters). Who "belongs" has been a hot question in New Hampshire since long before the Coronavirus emerged, but Covid-19 has emphasized existing fault lines. Lots of people with second homes moved more full-time to New Hampshire starting in March 2020, escaping areas with higher infection rates but being perceived as virus vectors by locals, particularly in areas that usually only see tourists in the summer. Vaccine scarcity has created an us against them mentality. NH is prioritizing those most at risk of death - which means those in nursing homes and congregate care facilities (did anyone know that word prior to coronavirus?) and first responders, but in the state with the 4th largest elderly population, that leaves a lot of people over 65 and living at home as second in line. The Governor had already put ski patrol in the list of first responders (so ski areas could open), so letting second home owners get vaccinated seemed to again prioritize those with more money over those more at risk. Little of any of this affects me directly - I'm already in a lower vaccine category due to being younger and healthier than the state average. But in a state where 21 years residence still marks you as an outsider since your family is not from NH, the increased "localism" feels potentially dangerous. While prioritizing full-time residents make sense to me, what will be the next line drawn and will I be okay with that one? How do existing biases in NH affect our vision of "who belongs"? -
 2021-01-24
2021-01-24SE NM’s Hospital COVID-Bed Capacity
This information displayed on this webpage contains an interactive map with corresponding data summary of the dedicated COVID beds and general capacity of hospitals in southeastern New Mexico for January 24th, 2021. This snapshot demonstrates a reasonably live and present condition of the availability for urgent and emergent COVID medical care within that geographic region and at that date and time. -
 2021-01-22
2021-01-22Navajo Nation COVID-19 Vaccine
Navajo Department of Health directive on Vaccine roll-out. -
 2021-01-20
2021-01-20The Trials and Tribulations of Getting This Shot
It's important so that people realize that just because a vaccination is approved for use, it does not mean that it's readily available -
 2020-12-13
2020-12-13A Choice of Monetary Support or Raising your Children?
This report done by the Center for American Progress really opened my eyes to the way mothers have been affected by the pandemic. For so many mothers, the pandemic forced them to choose between supporting their family by working, or leaving the workforce to become stay at home parents. For myself, I had no other choice than to become a stay at home mother because of the closing of schools and childcare. My son is a toddler, before pandemic he attended a private childcare two days a week and spent the other three with family members so I could work. By the quarantine in March, my job had “closed for the foreseeable future” and my son no longer could visit his family due to the risks. As most of the population has, mothers have made sacrifices this entire pandemic, they have struggled to provide, given up the little time away from home they had and stepped into numerous different roles to ensure their children are safe, cared for and learning. Now, I question if there could’ve been more help for the mothers around the country when the pandemic hit? Could the government relieved some of the stress of losing an income? Why was it a choice between money and the lives of their children? -
 2020-12-12
2020-12-12Nurse Fighting for Racial Equality in Healthcare
This is a video of a nurse who volunteered to go to New York and help out with the COVID-19 pandemic in hospitals. She was overwhelmed at the number of patients she had that were Hispanic, Black, Latino, and Middle Eastern, and other people of color. It was clear to her that they were being disproportionately affected by this pandemic and chose to march in protests along with them. The acts of Becca Cooper, and the stories she told her audience about, amplify the voices of marginalized groups by speaking out about it and making people aware of these communities and how heavily they are being affected. I think 2020 has also been a year of protests to fight for equal rights and that speaks out to my generation as well. I know a lot of people who have participated in these protests and it goes to show how my generation is standing up for what we believe in, much like Becca Cooper did for her patients. -
 2020-11-24
2020-11-24Conditions in Hospitals
An article from the Globe and Mail about the conditions hospitals workers experience. -
 2020-12-04
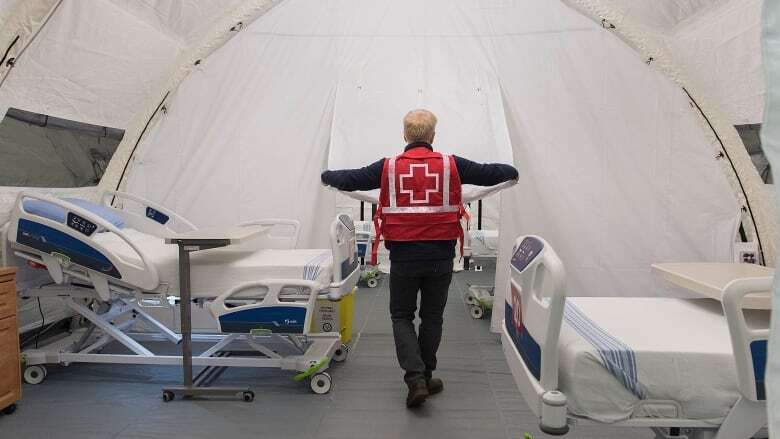
2020-12-04Field Hospital
A volunteer adjusts the opening to a tent in an indoor field hospital in Montreal -
 2020-04-11
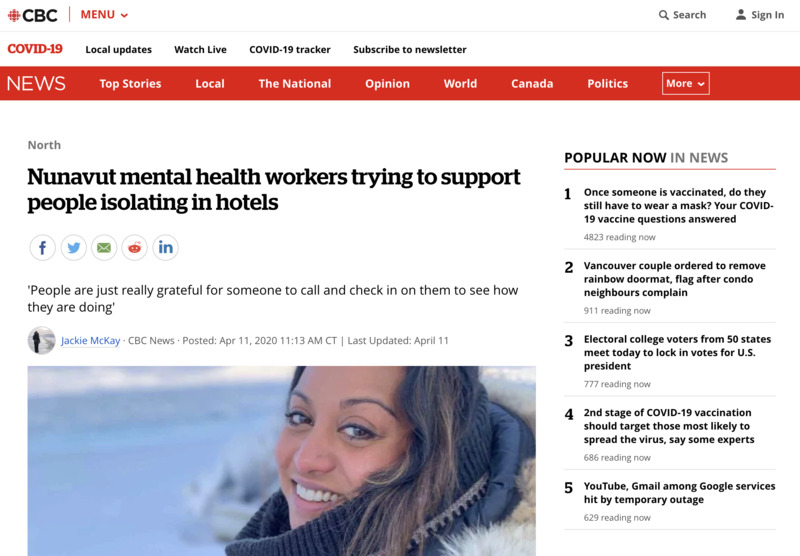
2020-04-11Mental Health Check-ins for People Isolating in Nunavut
An article from Canadian Broadcasting Corporation about mental health workers in Nunavut trying to support people in self-isolation -
 2020-09-24
2020-09-24Trudeau talks about the importance of health and safety of Canadians right now. Meanwhile...
Nunavut MP Mumliaaq Qaqqaq shares photos of toxic mould from local homes via. Twitter, an issue ignored by the federal government in the wake of other health concerns during the COVID-19 pandemic. -
 2020-12-13
2020-12-13Doctors Can Work From Home Too
A cartoon of a nurse assisting a remote check-up -
 2020-07-20
2020-07-20Nunavut to get $18.9M from feds for COVID-19 response
Health and Finance Minister of Nunavut George Hickes announced the federal government's plan to give $18.9M for testing, PPE, paid sick leave, and COVID relief. -
 11/20/2020
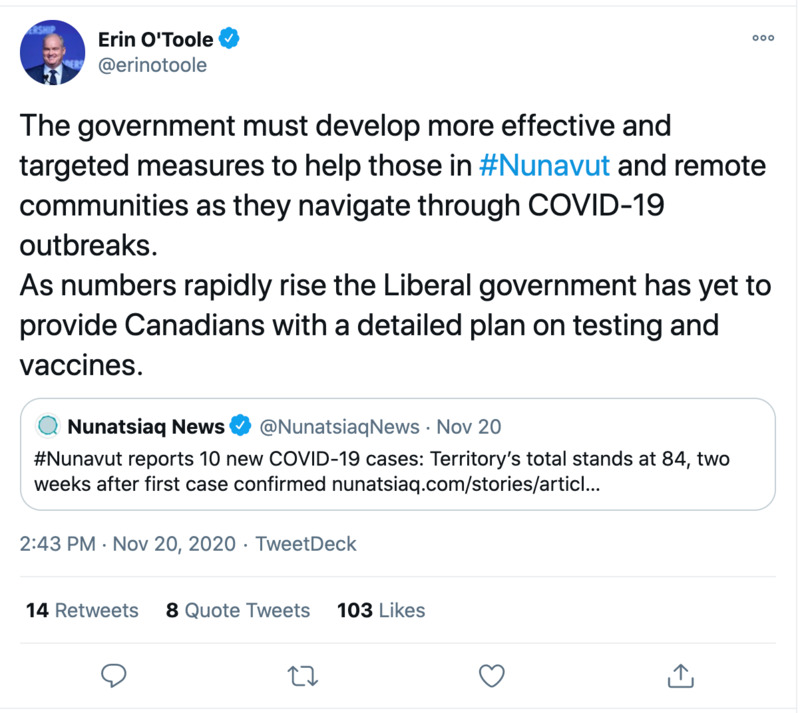
11/20/2020Progressive Conservative Party Leader Erin O'Toole on Twitter: The government must develop more effective and targeted measures to help those in #Nunavut and remote communities as they navigate through COVID-19 outbreaks.
Canadian Progressive Conservative Party (PC) leader Erin O'Toole responds to tweet from Nunatsiaq News reporting 10 new COVID-19 cases in Nunavut. -
 2020-11-19
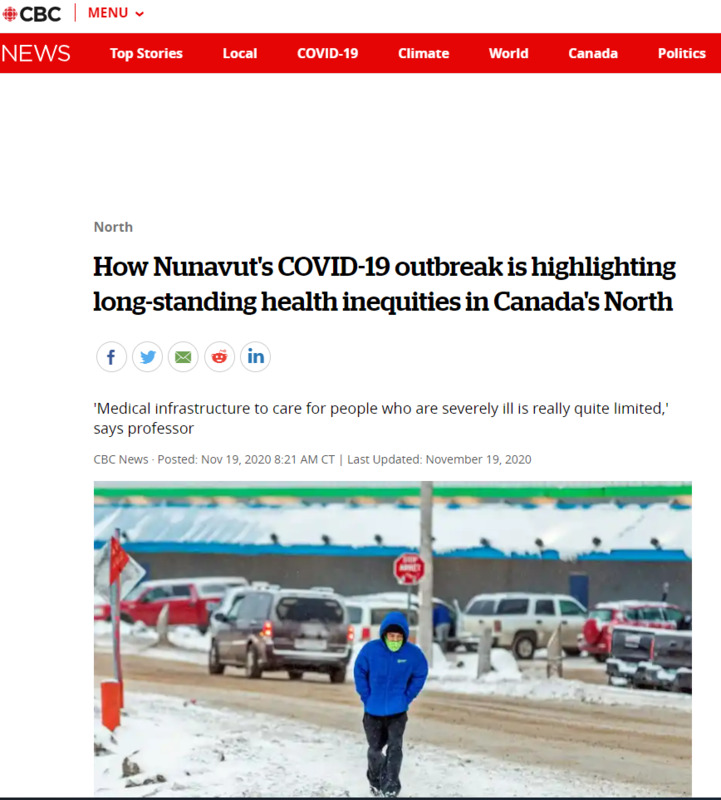
2020-11-19How Nunavut's COVID-19 outbreak is highlighting long-standing health inequities in Canada's North
Chief Public Health Officer Dr. Michael Patterson said in a press conference on Wednesday that Nunavut is reaching its limit in terms of what it can handle. Three contact-tracing teams are racing to reach out to people in the four communities which have cases of the virus: Arviat, Rankin Inlet, Whale Cove and Sanikiluaq. -
 2020-12-02
2020-12-02Stuck in a hotel during a Christmas pandemic, Neskantaga members wait for water crisis to end
Neskantaga has the longest-duration boil water advisory of any reserve in the country — 25 years and counting. Members of Neskantaga First Nation have been staying in Thunder Bay for over 40 days as water crisis continues. -
 2020
2020Nunavut Self Assessment Tool
An online self-assessment tool to determine if one should be tested for COVID-19 -
 2020-12-13
2020-12-13Nunavut Health Facilities Map
A Map showing all the active health facilities in Nunavut -
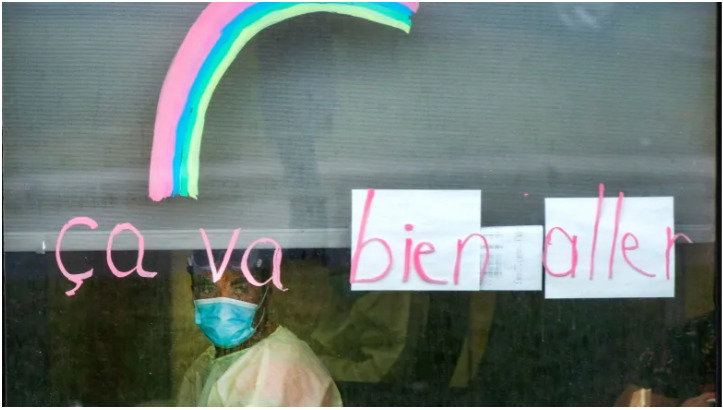 2020-06-06
2020-06-06Stress in Long-Term Care
An article from the Canadian Broadcasting Corporation about stress and overwork in healthcare workers who have been redeployed into long-term care homes -
 2020-03-23
2020-03-23Canadian Federation of Nurses Unions Demands for worker protections
A document describing the official position of the CFNU on reasonable precautions that should be put into place to prevent nurses and other healthcare workers getting Covid-19 -
 2020
2020Coalition Poids - COVID-19
The Québec organization Coalition des Poids is dedicated to creating environments that facilitate healthy life choices. Aware of the potential negative impacts the government lockdown would have on our health, this company produced graphics to inform and help the public maintain their health during the pandemic. The illustrations encourage Canadians to take care of their physical health through proper nourishment, physical activity, and sleep. -
 2020-06
2020-06Restoring Trust: COVID-19 and The Future of Long-Term Care
Established by the President of the Royal Society of Canada in April 2020, the RSC Task Force on COVID-19 was mandated to provide evidence-informed perspectives on major societal challenges in response to and recovery from COVID-19. The report begins by reviewing the research context and policy environment in Canada’s long-term care sector before the arrival of COVID-19. It summarizes the existing knowledge base for far-sighted and integrated solutions to challenges in the long-term care sector. The report then outlines profound, long-standing deficiencies in the long-term care sector that contributed to the magnitude of the COVID-19 crisis. -
 2020-11
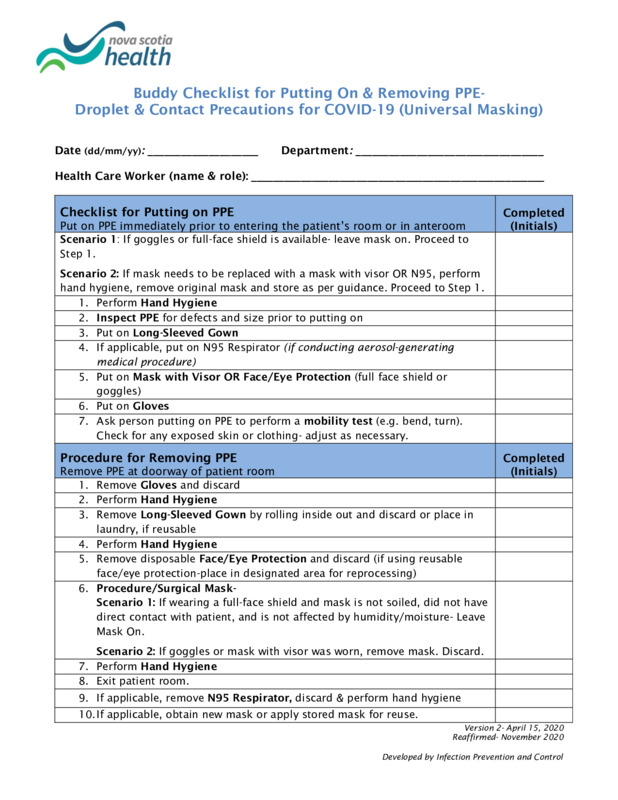
2020-11Checklist for Putting On & Removing PPE
Checklist for healthcare workers when putting PPE on and taking it off. Important to remember that many healthcare workers did not have to don PPE before the pandemic and needed guidance. -
 2020
2020Guiding Principles for Redeployment to Long Term Care
This is the guiding document for the redeployment of healthcare workers to long-term care from the Ontario Hospital Association. These are crucial to understanding how redeployment worked in Ontario. -
 2020-03-25
2020-03-25At least 2 Toronto hospitals begin rationing protective gear as COVID-19 crisis deepens
Early news article about rationing PPE. -
 2020-05-12
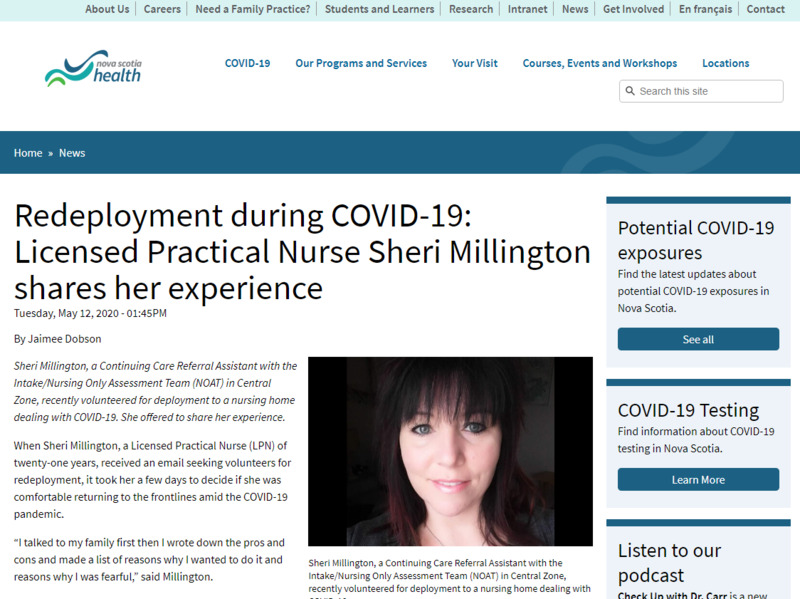
2020-05-12Redeployment during COVID-19: Licensed Practical Nurse Sheri Millington shares her experience
A nurse from Nova Scotia writes about her experience being redeployed into a nursing home. -
 2020-04-25
2020-04-25Ontario allows redeployment of staff
The Ontarian Government allowed hospitals and long-term care homes to redeploy staff to new roles and duties for the better care of the vulnerable. -
 2020-12-09
2020-12-09Authorization of the Pfizer-BioNTech Vaccine
Tweet by Health Canada confirming that the Pfizer-BioNTech vaccine has been approved. -
 2020-12-10
2020-12-10'We need trust': How a COVID-19 vaccine came so quickly
News article that details why the vaccine has come so quickly and assuring Canadians that the vaccine has not been rushed. -
 2020-10-19
2020-10-19"It's very scary at WGH right now," says employee
This is a news article about the conditions at the Whitehorse General Hospital. The article highlights the staffing and shortage issues that are causing unsafe conditions in the hospital. -
 2020-04-03
2020-04-03Inside a COVID-19 Unit
Video interviewing staff in a Sunnybrook COVID unit. The staff talk about the dedication of the team and the need to rely on one another for support and guidance.
