Items
Tag is exactly
doctor
-
 2022-06-10
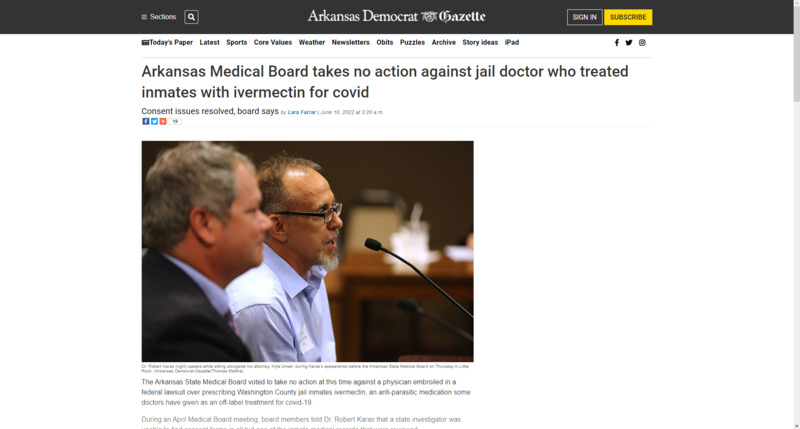
2022-06-10Arkansas prison doctors and ivermectin
This is a story detailing Arkansas' Medical Board dismissing charges against a Washington County prison doctor for treating prisoners with ivermectin. Arkansas' Medical Board has not explicitly denounced the drug as a treatment for COVID-19, and many physicians prescribe the drug. This particular physician treated several unknowing prisoners with ivermectin in order to combat rising covid cases in the Washington County Jail in April. This dismissal of charges by the Medical Board reveals a deeper skepticism of the pandemic in Arkansas and a willingness of the board to allow physicians to treat their patients as they ultimately see fit with minimal regulations. I feel it also reveals a deeper understanding of Arkansas' prison system due to the prisoners not being informed of what was given to them, and therefore without consent. -
 2022-06-23
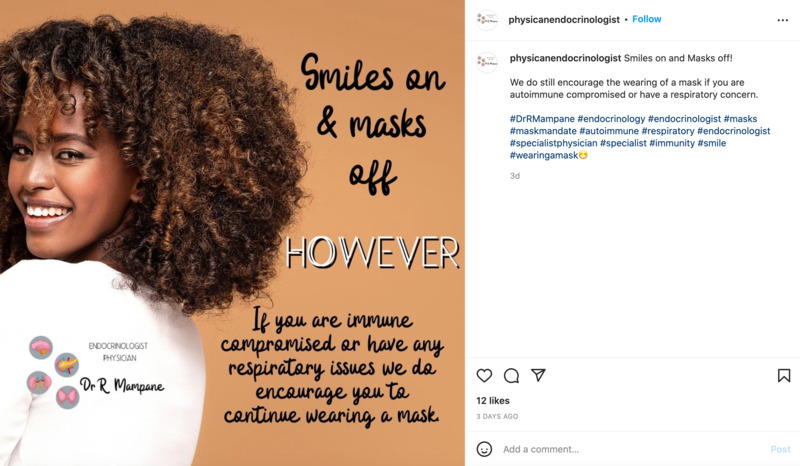
2022-06-23Smiles on and masks off
This is an Instagram post from physicianendocrinologist. This is about a changing mask policy at the endocrinologist office that posted this. It encourages people that are immunocompromised to wear masks though. -
 2022-02
2022-02Wear a Mask: Fa'aaoga Puni Fofoga
With the rise of covid cases in American Samoa at the beginning of this year in February, the Department of American Samoa Health Department partnered up with the American Samoa government to make sure that the people of American Samoa are well aware of what to do to combat COVID. It is one of the many flyers and ads released by the ASDOH for the public of American Samoa. They are released in both the English and Samoan languages. This flyer is for people to wear a mask and in the Samoan language, fa'aaoga puni fofoga. -
 12/21/2020
12/21/2020Who you callin "doctor"
A comic strip about Covid-19 -
 2022-04-19
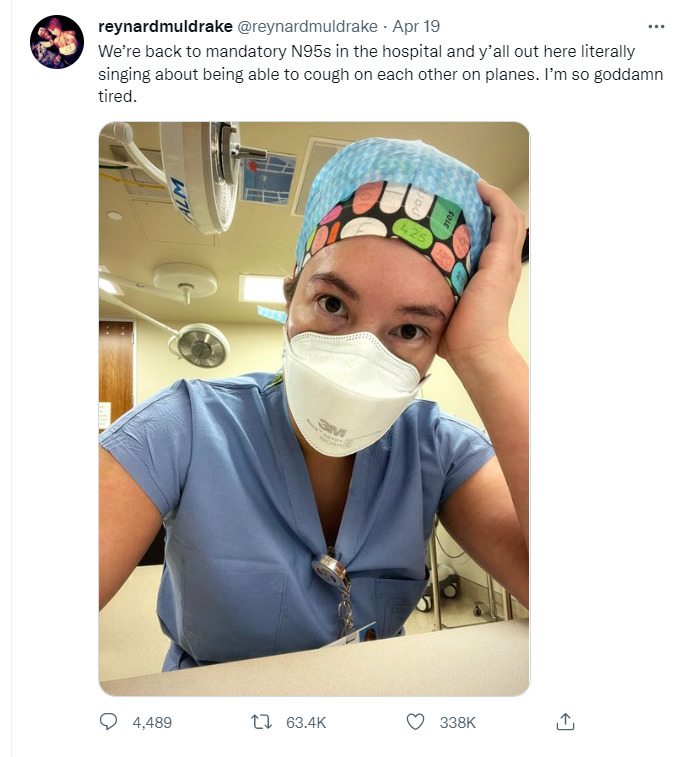
2022-04-19Twitter post in response to masks no longer being federally required on planes
A Twitter user, who works in a hospital, shares her frustrations after masks are no longer federally required on planes. Many people are happy about this ruling, but others, especially those on the "frontlines" in the hospitals, are expressing their frustrations with people acting as if the pandemic is over. -
 2020-04-02
2020-04-02April Fool's!
A comic strip about Covid-19 -
 2020-08-04
2020-08-04The new doctor
A comic strip about Covid-19 White House Interviews More Alternative Doctors Dr. Strange: I saw 14 million possibilities and you screwed up all of them. President Trump: Strange. Weird. No thank you. No more reality TV guys, Dr. Phil. Cat in the Hat: The more you read, the more... President Trump: "Read"?? Bye, Dr. Seuss. I thought you were already on my staff. Who are you? Dr. Fauci: Um, Dr. Antoine Caufi. President Trump: Sounds fishy. You're hired. -
 08/21/2020
08/21/2020Caroline Birks Brown Oral History, 2020/05/31
In this interview conducted by Christina Lefebvre, Dr Caroline Birks Brown describes the drastic changes she saw while working in a hospital. She discusses patient care, the hospitals rapid response to converting floors to ICUs, and the way the hospital delt with staffing enough nurses to provide sufficient care to patients. She discusses how Spanish speaking doctors and nurses were asked to volunteer to work to avoid depersonalization and how other branches, like social workers, stepped up to provide the best care possible under the circumstances. Dr Caroline also touches on the possibility of young people getting covid and her thoughts on the patterns of the groups of people getting sick. She reenforces her appreciation of nurses and also discusses the politicization of the virus. The interview ends with her thoughts on what could have been done differently, politically and socially, to control the spread of the virus. As a mother, she talks about distanced learning and its effects on children and the importance of socialization. The last topic is about lessons she hopes we have learned. -
 08/04/2020
08/04/2020Anonymous Oral History, 2020/08/04
Anonymous oral history of Dr who is treating patients and a Massachusetts hospital. He talks about working with residents and students and how work life has changed because of the Covid-19 pandemic. He discusses one such patient who is an employee at his hospital who contracted Covid-109 and was dealing with the implications of it. He mentions that the patient is of Salvadoran decent and had to learn how to take steps and even talk after being on a ventilator. The doctor interviewed is optimistic about what this is teaching medical students and residents about their job profession and finishes the interview with his opinions about how the government response was complicated and lacking. However, at a societal level the interviewee states, the nation is handling the pandemic, well. -
 04/25/2021
04/25/2021Lou Fraise Oral History, 2021/04/25
Dr. Lewis Fraise details his service as a geriatric doctor during the Korean War and Vietnam War. He mentions his service in both Washington D.C. and Korea and continues to break down how the Coronavirus actually infects one's body and the response of the government as the pandemic ensued. Dr. Fraise criticizes the actions of Donald Trump and states that the spread of more medically-accurate information would have led to a better outcome in terms of the early stages of the pandemic. -
 2020-04-20
2020-04-20Mask Bag
This image captures a bag of masks that a doctor (my mom) carried with her during the pandemic. -
 2021-10-21
2021-10-21HIST30060 Vaccine Sticker
This photo is a picture of the sticker that the doctors would give out once you got your vaccine shot. My doctor peeled off the sticker and handed it to me, and I quickly put it on an old receipt in my bag because I wanted to keep it. Outside of the last few years, diseases often did not really play a role in 21st century Australia, but now the sticker shows how some people have a sense of pride around being vaccinated. My partners doctor placed the sticker directly onto his shirt, and he was quite happy to wear it the whole way home. In addition, the Victorian government logo on the bottom shows how the government is endorsing vaccinations for the public. HIST30060. -
 2020-05-15
2020-05-15Take Charge of Your Health
A blog post from Banner Health on how to take charge of your own healthcare. -
 2021-10-05
2021-10-05Pandemic 2020
The pandemic affected many of our day to day lives. To start off it isolated us from socializing with friends, family, coworkers and others. It restricted us from doing our normal daily activities and routines. It made us miss important events and milestones that we can’t take back. For me the pandemic was very difficult, although the pandemic has not ended, the start of the pandemic was the biggest hardship. To start off, I had just started a new job that required me to help others get through the pandemic. I was assisting about 12 dr offices in scheduling patients. This was overwhelming to say the least and caused stress and anxiety. Many of us were facing challenges that can be stressful, overwhelming, and cause strong emotions in adults and children. Public health actions, such as social distancing, were necessary to reduce the spread of COVID-19, but that could make us feel isolated and lonely and could increase stress and anxiety. I know for me it was very hard not to be around my family. I’m very close with my family and not being able to see them and hang out with them definitely took a toll on me. For starters I was not able to be in the delivery room with my sister who was pregnant at the time and I was not able to meet my niece in person for months. The first time I met her was through FaceTime, which was not the same as being able to hold my first niece. Adults struggled adapting to new social routines—from choosing to skip in person gatherings, to consistently wearing masks in public. Daily activities that one would normally do were taken. For me my daily activity was the gym and with the pandemic it caused a shut down and once it reopened it was difficult to adjust to the new “normal”. -
 2021-09-22
2021-09-22EM Oral History, 2021/09/22
It is important to strengthen the amount of first hand accounts of the pandemics for future reference and historical purposes. -
2021-08-25T13:03
Going to the doctor during the pandemic
Me and my mother drove down to Dell Children's hospital as we always do for our PT. Wednesday are busy days for them, so we parked on the second floor of the parking garage. My knees were feeling bad that day so we took the elevator. A family of three were also taking the elevator, and since the max capacity was four people we had to wait. We walked into the medical center (fully masked of course) but before we could leave the entryway we had to have our temperatures taken (mine was 97.1, like always) and answer a few questions "Have you had any symptoms? Fever? Headache? Coughing? Sore throat? Is anybody in your house being currently tested for COVID?" and since all the answers "no" we could enter. I've had a few days where I felt fine enough to go but because I had a headache I couldn't. The waiting room wasn't packed by any sense of the word, but since we had to make sure to keep our distance from other people we couldn't sit down anywhere. My PT (Physical Therapist) called me in, and we exercised for an hour, fully masked, which makes it a lot more uncomfortable, also making sure to keep our distance from everybody else. I went out afterwards and my mom and I went in our car, put some hand sanitizer on, and left to repeat the process next week. -
 2021-07-18
2021-07-18Shifting Back
My family was certainly filled with hope and a bit of relief when our county’s numbers began to steady at 30 cases a day with a positivity rate below 0.5 by June. However, we didn’t let down our guard. My husband’s best friend since childhood is an MD with the county and in May told us the Delta variant is here. We asked what that means and he said “well, outdoors you should be okay, but wear a mask indoors and don’t let anyone breathe on you.” He said this knowing we’re vaccinated and that our two kids, one being his goddaughter, are not old enough to get the vaccine. Numerous times since summer started I ruefully told my husband and mom “enjoy it while we can” because I think we all knew a spike would come once California lifted its COVID restrictions on June 15. It’s taken only a few weeks for LA to return to 1000 cases per day, and where we live in OC, daily cases have jumped from 30 a day to 150 a day in two weeks. Yesterday, the case count was 250 for one day. The variant is here. LA is taking swift action. Effective today, LA’s mask mandate is back in place for unvaccinated and vaccinated alike. It was immediately noticeable when we picked up dinner at King’s Hawaiian. The outdoor tent is up for to go orders pick up and mask mandate signs are posted. Honestly, if people just accepted the practice of wearing masks, I really do think it could help us return to pre June 15 levels. The report I read this week indicated that 100% (which sounds crazy, but it was cited) of the COVID hospitalizations in LA county are unvaccinated. It’s so strange to me that it is the unvaccinated who are so against wearing masks. I’m honestly wearing my mask to protect them, statistics seem to indicate if I get Delta, it should be mild. I just wish my kids could get the vaccine. Oh well, here’s to hoping the mask mandate comes back in the OC, too. -
 2020-06-06
2020-06-06Top Banner leader discusses Banner Health COVID-19 data during press conference
A press release from Banner Health recapping Dr. Marjorie Bessel's press conference on June 6, 2020. -
2021-08-06
Bruh Momo
The start of Covid really hitting was about February of 2020. We all went in cheerful for the new year but all it brought was plague. Covid only started a little before 2020 I think, my dad, friends, and myself all ended up getting sick around the end of 2019, probably about December or sooner when it was starting to get cold. The first things they did was give me medicine for pink eye, from my eyes being pink and veiny. Besides for that I didn´t really feel bad at all, i just had a cough that would kick in every so often, usually after activities. That all ended about two weeks into taking medicine and nasal drops. -
 2020-05-14
2020-05-14Banner Health revamping doctors' offices in the wake of COVID-19 with virtual waiting room
An article describing Banner Health System's move towards virtual waiting rooms for doctors' visits. -
 2021-05-07
2021-05-07Story of civic warrior 2 nd wave in india
Daily diary of a covid doctor for last 2 months…. The message towards the end of 2nd wave of pandemic The last 2 months of 2nd wave of the pandemic have been the most hectic in all aspects emotionally, physically, personally. Finally got some time to pen down my experience towards the end of this 2 wave. Working in territory care hospital as an intensivist, managing own start-up Providing doctors on call for a home visit, tele and video consultation, free consultation for underprivileged people. Every day waking up after hardly 2 to 3 hours of sleep. I will would see 10 to 15 miss calls, Finish teleconsultation as much as possible and then do a home visit for few patients on the way to hospital, Home visit for covid patients has been a totally different experience, these were the patients under the most stressed condition not getting hospital beds, their family physician had stopped seeing them due to fear of self infection. with proper PPE protection treating patients at home successfully is so self satisfactory as a doctor which only COVID warriors like us can understand. Then reaching my COVID ICU where the sickest patients in the city are there, managing such a sharp surge in critical cases has been a Herculean task, time is key in critical care setup, the timely decision to give ventilator support or ECMO support saved few lives. thankfully I have the best doctors, nurses, paramedics, housekeeping, and management guys who make our work easy. Those grueling 8 hours In PPE without food water or toilet. And the most important was talking with the family of those sick patients, ask any 1 of our covid warriors every1 has hundreds of sad story of each family. This used to break us emotionally. Coming out of covid ICU, the number of missed calls for teleconsultation was pending. I would finish them while having lunch In the evening. During the peak of this my wife working as anesthesia Doctor at BHU got infected for 2 nd time, And lost 2 elder family member due to COVID, But the patient's family expectations from me kept me doing my work, and didn't visit my sick wife or attended the funeral of any of my relatives. Then in late-night had kept free teleconsultation slot for my native hometown Sindri, Dhanbad patients. And also underprivileged patients from pan India. After finishing calls, night again would start home visit for covid patients which would go till 2 to 3 am in the morning. Then finally to find a nap of few hours till the next day of battle. This is the story of lakhs of lakhs of covid warriors like me. But think about us now we are also getting burnt out, So request all people not to relax after 2 nd wave, get vaccinated use mask maintain social distancing even after govt unlocks, it's not over yet………... Dr Animesh Kumar Mishra Critical care medicine specialist Apollo Gleneagles Hospital. Founder of DCHS healthcare solutions. 9176138128 -
 2020-06-04
2020-06-04The Doctors and the Community
I'm submitting a picture of doctors, including my uncle and members of the community gathered outside of the SUNY Downstate Medical Center University Hospital, to celebrate the discharge of a patient who beat Covid-19. -
 2021-04-11
2021-04-11Alarm grows over impact of states banning trans youth treatment
Medical experts and LGBT advocates are sounding the alarm over the physical and mental health risks to the transgender community after at least 19 state legislatures, including Arkansas, have proposed or passed bills seeking to ban trans youth treatment. Proponents of the bills have argued that the legislation is in place to protect children from making irreversible decisions about their bodies. But earlier this week, doctors and LGBT organizations defended treatments such as puberty blockers and hormone therapy, and warned about a potential increased suicide rate among trans youth if such legislation is enacted. -
 2021-04-17
2021-04-17RIP Dr. Wayne John Edwards
This is a screenshot from the Black Alberta Instagram page about the passing of Dr. Wayne John Edwards to COVID-19, as the description stated: "Dr. Wayne John Edwards is the seventh Albertan health-care worker - and the second doctor to die from COVID-19 since the beginning of the pandemic, according to Alberta Health. Edwards died at the Chinook Regional Hospital in Lethbridge on Tuesday at the age of 66. #BlackAlberta #YEG #YYC #edmonton #calgary #alberta #albertacanada #calgaryalberta #edmontonalberta #albertacanada🇨🇦" According to the comments of the post, Dr. Edwards was a respected and beloved family psychiatrist, the comments were full of love and respect for Dr. Edwards, he will surely be missed. -
 2020-01-04
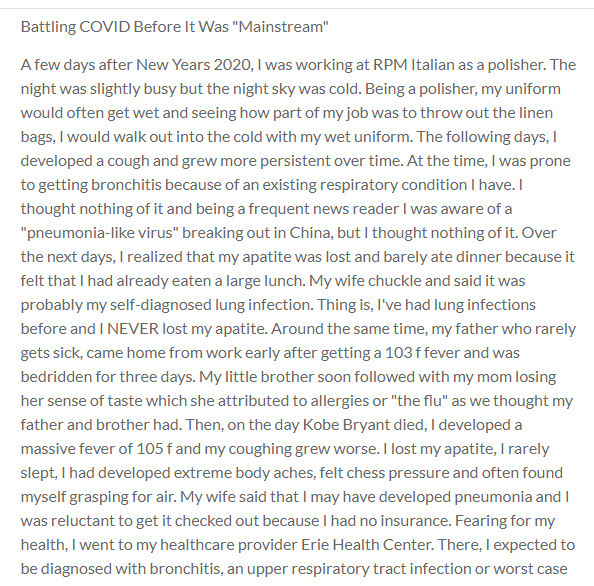
2020-01-04Battling COVID Before It Was "Mainstream"
A few days after New Years 2020, I was working at RPM Italian as a polisher. The night was slightly busy but the night sky was cold. Being a polisher, my uniform would often get wet and seeing how part of my job was to throw out the linen bags, I would walk out into the cold with my wet uniform. The following days, I developed a cough and grew more persistent over time. At the time, I was prone to getting bronchitis because of an existing respiratory condition I have. I thought nothing of it and being a frequent news reader I was aware of a "pneumonia-like virus" breaking out in China, but I thought nothing of it. Over the next days, I realized that my apatite was lost and barely ate dinner because it felt that I had already eaten a large lunch. My wife chuckle and said it was probably my self-diagnosed lung infection. Thing is, I've had lung infections before and I NEVER lost my apatite. Around the same time, my father who rarely gets sick, came home from work early after getting a 103 f fever and was bedridden for three days. My little brother soon followed with my mom losing her sense of taste which she attributed to allergies or "the flu" as we thought my father and brother had. Then, on the day Kobe Bryant died, I developed a massive fever of 105 f and my coughing grew worse. I lost my apatite, I rarely slept, I had developed extreme body aches, felt chess pressure and often found myself grasping for air. My wife said that I may have developed pneumonia and I was reluctant to get it checked out because I had no insurance. Fearing for my health, I went to my healthcare provider Erie Health Center. There, I expected to be diagnosed with bronchitis, an upper respiratory tract infection or worst case scenario pneumonia. However, when the doctor saw my condition and heard my symptoms he said that it wasn't: pneumonia, bronchitis or a lung infection. Baffled I said then what do I have and he responded with: "mhmmmmm do you have asthma?" I said I did when I was younger but I out grew it. His response: "That's it. It's asthma". Unsatisfied, I said its not it because I haven't had any asthma complications in over a decade. He later said that a lung operation I had when I was three days old might be the culprit. Once again, I questioned it. He conceded and asked if I wanted to get x-rays done. I agreed and went to Northwestern Medical Center with Erie covering the costs. I got my x-rays done and I decided to go have lunch with my wife. Then, I started coughing, lost my apatite and developed a fever. We took an uber and went home were I collapsed on my bed and was knocked out cold in a nice sleep for 20 hours. The cough never went away until late February when talks of a potential lockdown to contain COVID was being discussed. I never thought much of what I had that winter until my mom got an anti-body test where she came out positive for the anti-bodies. The same day we watched a COVID special on Netflix and they highlighted the COVID symptoms. The ones that stuck out to me was: loss of apatite, chest pressure, fatigue, coughing, short-breaths, fever and trouble focusing. I clicked everything and realized: "Holy shit. I must've had COVID before it was cool" (ironically). Ever since my illness as I described, my mind has become more "foggy" with me having trouble focusing, remembering and even stuttering more often. Trouble focusing has been mentioned as a COVID complication in your post-battle with the infection. Fast forward to February 2021, I went back to Erie to get my yearly physical done expecting to hear my sugar levels were off the charts. Except, my doctor walked in and first thing he said was: "so you had problems breathing in last year January?" I gave him a stare and asked "you don't think that I had..." and he interrupted and said "sir, you either had COVID before we knew what it was or you had some exotic virus" mentioning the latter in a sarcastic tone. There I realized, how chill I took COVID and literally brushed it off multiple times as a lung infection and nothing serious when in reality it was. Had I known what I had was COVID at the time that I had it, I would have been panicking and picturing death at my door. Often, your mindset can be just as dangerous as the illness itself. -
 2021-04-09
2021-04-09Small Sense of Normalcy
My daughter often has medical procedures and my husband and I have a system of working together to care for her during hospital stays and surgeries. Since the pandemic, there have been tons of restrictions and we are not able to physically support each other. Only one parent can go inside for appointments and procedures. Only one parent can stay in an inpatient room at a time. We had the appointment scheduled for over a month, but did not get the news that some restrictions had been lifted until the day before the procedure. My schedule is more flexible than my husband's so the original plan was for me to take our daughter and FaceTime him for the doctor consult. Luckily, my husband was able to get off work on short notice and we both were able to be there at the hospital! The only restriction was that only one parent could go back into recovery room and parents could not switch out. We did not receive good news, so it was good my husband and I were able to be together. -
 2020-05
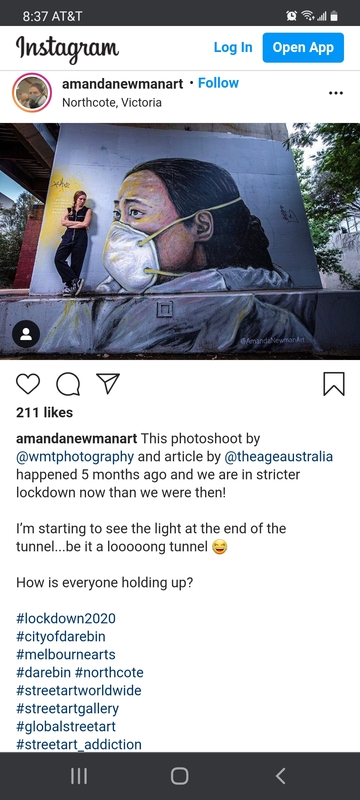
2020-05Pandemic Street Art: Amanda Newman mural of Ai Fen
Artist Amanda Newman created a mural of senior Doctor Ai Fen if the Wuhan Central Hospital. The image is on a pillar of a railway overpass in Urquhart Street, Northcote. Newman chose the doctor as her subject because she was silenced, reprimanded, and accused of spreading rumors during the beginning stages of the COVID-19 outbreak in December 2019. -
 2021-04-04
2021-04-04Putting off Medical Appointments for fear of COVID
I myself did not see a doctor or make any appointments until August of 2020, roughly 5 months into the pandemic. I attended my well woman’s exam, something I get yearly. The article I have added here was written by a doctor. He talks about in the beginning of the pandemic, it was critical to only see the patients that needed to be seen, as there was still so much unknown. He goes on to talk about how the risks from postponing exams outweigh the risk of catching COVID-19. This is a big part of my research, the unintended consequences of the COVID-19 pandemic. "A woman is more likely to die from an advanced-stage breast cancer than she is from COVID-19," said Therese Bevers, a medical director at a MD Anderson Cancer Center. The doctor who wrote the article said he consulted with other doctors to create a list of appointments you should stop putting off. These are: cancer screenings, checkups for “new red-flag symptoms,” follow ups for chronic diseases, mental health management, and sexual health management. It is clear that these issues are important for human health upkeep, and they shouldn’t be avoided due to COVID-19 anymore. We have yet to see just how many health issues have been ignored during this pandemic. -
 2021-02-27
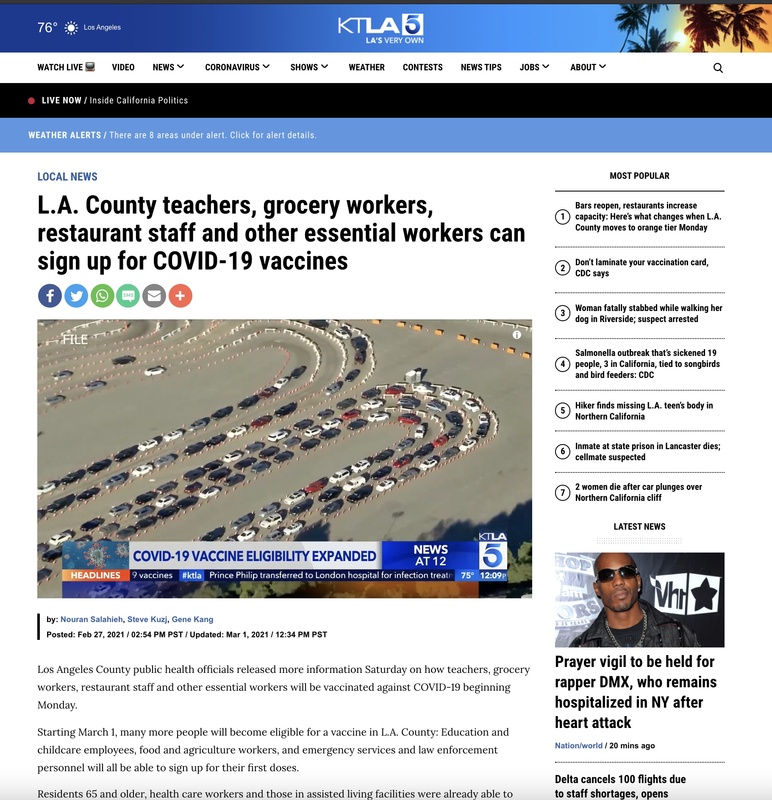
2021-02-27L.A. County teachers, grocery workers, restaurant staff and other essential workers can sign up for COVID-19 vaccines
Los Angeles Country prioritized teachers, grocery workers, restaurant staff, and other essential workers in their vaccine rollout, making them eligible the beginning of March. Given the high level of exposure these positions involve, this is necessary to protect essential workers and limit the spread of Covid-19. Also prioritized are transportation workers, homeless individuals and those in prisons, as they are often in close contact with groups of people. Not all states are following this prioritization of essential workers despite the CDC recommendations, focusing instead on factors such as age to guide their rollout. By protecting teachers, service industry workers, and others in contact with large numbers of people every day, we can slow the spread of Covid-19. -
 2021-03-11
2021-03-11Healthcare providers honor Covid-19's One Year Anniversary
This article is about the one-year anniversary of Covid-19 and how healthcare providers are celebrating and honoring the occasion. Healthcare workers and EMS providers have spent the past year on the front-lines of the Covid response. They have sacrificed much and have seen unprecedented horrors during this pandemic. This article features several social media posts from various healthcare agencies. In all of these posts, they acknowledge the patients and providers that we have lost in the past year, but also celebrate the efforts of the providers in trying to help the public during this pandemic. -
 2021-03-26
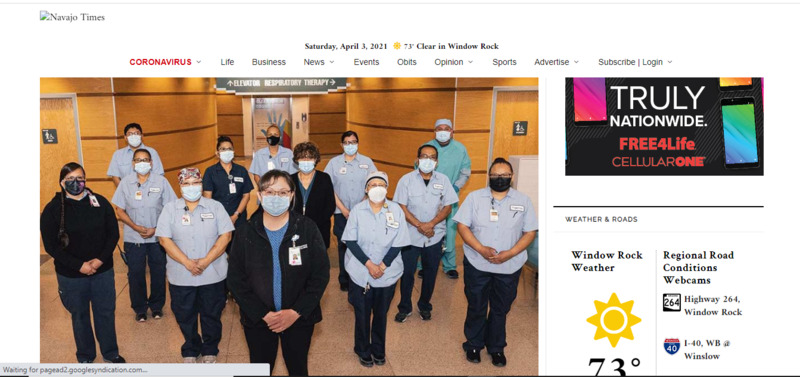
2021-03-26‘They became warriors’: Reflections from the front lines as Tséhootsooí Medical Center workers share experiences
By Rima Krisst | Mar 26, 2021 | CORONAVIRUS, People | Tséhootsooí Medical Center workers share experiences Wilberta “Billy” Jackson, public health nurse III This pandemic has been the longest roller coaster of stress, grief, and loss. I’ve kept my routine simple – sleep, eat, and exercise. And, more sleep. This has been and will probably be the most challenging time of our lives. I could focus on all the bad, but so much good has come from this, from community members stepping up, leaders rolling their sleeves up and getting dirty, how we came together to care for our elders, and so much more. Professionally, we’ve adjusted and readjusted a million times over and completely changed how we deliver health care. We’ve had information, guidance, and policies being added or changing every day and we still were able to deliver health care in a safe, efficient manner. At the beginning of the pandemic, our leaders were warning everyone about the health care system being overwhelmed. Most people thought about it in terms of hospitals running out of beds, but they didn’t think of it in terms of how an underfunded and shorthanded public health force would respond to a pandemic in a rural area with limited resources, and where a population’s most basic physiological and safety needs are not being met. When you don’t have access to clean water, food, shelter and security, you’re not able to prioritize prevention measures until your basic human needs are addressed. The resiliency of the Diné people is unrivaled. The days I’m struggling or feel like giving up, I hear my grandmother’s words, and that’s what keeps me going. And my mother’s surprise delivery of Navajo soul food meals. I’m a public health nurse, so it won’t come as a surprise that I’m excited about the COVID vaccines. We’ve already seen a substantial decline in cases, hospitalizations, and deaths, so we know it’s working. My hope is that our response to the next pandemic or health care crisis won’t be complicated by politics, lack of national strategy, lack of preparation, and misinformation. Stacey Burnside, Primary Care registered nurse What I have learned from this pandemic is to cherish every day and every person that you love. COVID-19 has impacted my family and me profoundly. I lost an uncle and an aunt to COVID-19, and to this day, it is surreal that they are gone. As a primary care nurse, it is difficult to hear about losing a patient to COVID-19, and at the peak, it was almost a daily occurrence… The challenges that I faced during this pandemic were adapting to the changes in work roles and being separated from the people I love. The clinic that I worked in was closed when the pandemic hit the first peak, and I, along with my coworkers, was informed that we had to work in the Emergency Room. The moment that I saw a patient who needed me to be their nurse, despite having COVID-19, humbled me. That moment in the ER humanized COVID-19 for me and made me realize that I was put there for a reason. No matter what the situation is, nurses adapt, and the teamwork and strength we draw upon each other are phenomenal. A huge hit to me personally and professionally was losing a friend to suicide … dealing with grief, loss, and stress has been a daily thing. What has helped me is drawing strength from my God, husband and son, and family. There are many negatives to the pandemic, but one positive that many have seen is the love and strength we have found among our families. I am thrilled that we are at a point of a high vaccination rate in the Navajo Nation. I remember when I administered my first COVID-19 vaccine to a patient, it brought tears to my eyes, and I cried after work. Leah Chattin, respiratory therapist I’ve been a respiratory therapist since 2003. What I experienced throughout the first surge of COVID-19 here on Dinetah is not what you prepare for. I see the impact on my life as deep internal scars that I buried and to resurface those experiences is a nightmare. Imagine the inability to fully take a deep breath, something so simple we take for granted. Supporting my patients with breathing treatments, providing chest physical therapy, changing breathing devices constantly because the demand for oxygen escalates all in a 12-hour or more shift. All these specialized techniques to avoid the last option of intubation, allowing an artificial airway introduced to your trachea with an opening at the tip to provide mechanical breaths from a mechanical ventilator. Fear expressed from my patients was a frequent emotion. You are alone, isolated from your family, your loved ones, no familiar face to embrace, to celebrate your improvement or the worst, a decline despite the battle you have endured. I’d remind my patients not to give up… Instinct took over because I’m a mother too, a nurturer. I can remember softly stroking their hair, holding their hands, shedding tears, praying, putting myself in that empty place at bedside where your family should be gathered, processing the grief. Accepting loss was tremendously difficult. I lost myself because I did not decompress my emotions. My spirit slivered away slowly each time my patients faced rejection of our efforts to sustain life. How I endured and sustained my sanity was prayer requests. Prayer was undoubtedly my saving grace. This virus is fluidic, the path it took was unpredictable. I strongly believe we need to continue wearing a mask, following the CDC guidelines and begin or sustain our health and wellness. Putting into words my experience was not an easy effort, however it’s a pathway for healing. Every COVID patient I battled for will forever have a place in my heart. Sandra Fouser, nurse executive of the Primary Care and Specialty Clinics Seeing the virus cross the ocean and hit the heart of the Navajo Reservation forever changed our lives. As a health professional, I knew venturing into the unknown with limited protection meant some would survive and some wouldn’t. What I have learned working on the front lines – compassion, cohesiveness, companionship, strength, sadness and mental stress. We have been battered, beaten, praised, comforted and have also received recognition from all walks of life. I am proud to be a nurse. I believe the strength to endure comes from resiliency and the people we work with and the support of our families at home. As nurses, we cannot stand still. I feel it is in our blood to help and move forward. I have lost friends, coworkers, relatives and patients. The grief I feel is palpable, almost more than I can handle. Seeing my family, staff and patients suffer through illness and grief has been very challenging and heartbreaking. As a team, I believe when something happens to one of us, we all feel the effects, we grow closer and find comfort in each other. I see the vaccine as a progression toward eradicating the detrimental effects of this virus and giving us hope that there is a better tomorrow and that Hózhó will be restored. Dr. Karen Williams, hospitalist physician I am a Native physician (Mountain Maidu/Apache) and Indian Health Service Professional Scholar. When the pandemic started our hospitals were suddenly overwhelmed with large numbers of very ill patients needing oxygen. Some patients who worsened were placed on a “life support” or ventilators since they could no longer breathe on their own. Despite our best medical management efforts, including use of high-flow oxygen, there were patients who did not survive. I witnessed more death in a year than I have ever experienced in my career. This was traumatic for me because every day I came to work I felt like I was coming into a war zone. We saw people struggling to breathe and fighting for their life. We heard family members saying their goodbyes to their loved ones and crying over the phone. We held hands of those who took their last breath and witnessed co-workers not able to control their tears. If it were not for our team efforts, almost a military-style mentality, we could not have managed. As a hospitalist physician, the biggest challenge was ensuring that I had the most up-to-date medical knowledge to save a patient’s life. During the beginning of the pandemic many doctors throughout the country did not feel prepared. This was quickly overcome by learning medical strategies used by doctors throughout the world. The treatments used included steroids, anticoagulant medications, and high-flow oxygen. We had the support of our hospital’s incident command leadership and adapted to the changes. This included being able to offer our patients who needed oxygen a federal Drug Administration-approved “emergency use” medication called Remdesivir, and more recently Bamlavinimab for non-hospitalized patients My experiences on the front lines were psychologically and physically overwhelming … I sought support from elders and used my Native spirituality for strength. I also sought protection support from traditional Indian practitioners who set up a tipi and hogan outside the hospital for employees. I sometimes thought twice about the danger I was in. However, I acknowledged that I would never walk away. This is a result of my obligation to the Native community and the hundreds of patients I had gotten to know for so long. I “warriored up” in my mind and sought to do the best I could. I do not foresee an end to mask wearing, and now recognize how careful we all must be to protect each other. I saw too many elders get severely ill and even pass away from COVID as a result of young family members not being careful and bringing it home. I have encouraged community members and my own family to get the vaccine as soon as possible. I received two doses of the Pfizer vaccine and said a prayer in my Native way each time for protection. Natasha Topaha, certified medical assistant, Mobile Unit Overall, this year has been extremely challenging, but also has reinforced my personal strength and resiliency. I have had ongoing concerns throughout the epidemic regarding my kids’ isolation and their mental health. It has been difficult, but doable, to manage both working in health care and supporting my family both emotionally and physically. I had constant worry about bringing the virus home and infecting my family given that I was working in high risk areas and providing COVID testing, vaccines and social and mental health support to patients. I found that doing outdoor activities with my family, such as bike riding and hiking, helped me ease my stress and helped teach my children some healthy coping skills. And we could spend time together! I feel very happy and grateful in both receiving the vaccine and being able to provide it to patients and the community. I feel safer at work and at home now. Johnny Willeto Jr., facility manager/logistics chief The strength to endure comes from within yourself. For me this began in my childhood as the son of Delphine Damon Willeto and Johnny Willeto Sr., who nurtured me to become a great human being. They taught me to be a courageous, productive worker and know my limitations. As a facilities manager, my main focus and responsibilities are the protection in the physical environment of all who walk through the doors of Fort Defiance Indian Health Board’s facilities. All we knew is that COVID-19 was airborne and surface communicated. I treated it as you would tuberculosis and ensured that my staff had adequate PPE to help protect them when they are tasked with working in the patient care areas. This responsibility was a big challenge when trying to procure medical equipment such as masks, gloves, safety glasses, gowns, scrubs, and so forth. Having an MBA has allowed me to flourish in this high stress environment and to adjust with adaptations to finding supplies and creating new relationships with trustworthy suppliers. Being in close proximity to patients who are struggling with getting well can be heart wrenching. Being able to fulfill my duties in the support role to the best of my ability for my community and teammates has allowed me to sleep well at night knowing that I gave it my all. I have lost a brother-in-law who contracted the virus in the Scottsdale area of Arizona. These were very difficult times because as Navajos we are accustomed to comforting each other by a hug or handshake. With COVID, gatherings are not safe, so having family meetings for planning the funeral is off and also the funeral usually consists of 10 minutes before the burial with only a few close family in attendance. One of the biggest assets I have gained is the spiritual belief in God and keeping the communication open by saying my prayers often – to be thankful for the blessings that have come my way or when asking for strength to endure the hardships. In my free time I isolate on the Willeto Sheep Ranch in Goatsprings Valley, Arizona, where I tend 120 sheep and goats. Being able to separate the everyday stress and recharge is paramount to going forward with courage and mental sharpness to make the right choices for the organization, patients and employees. The vaccines are an effective tool to help reduce the mortality of the virus on us and give us protection to this invisible enemy. Corinne Legah, Environmental Service supervisor Personally, I was scared when I first heard of the spread of the virus overseas. It was shocking how fast the virus traveled. In the beginning our team was needed to help keep the hospital sanitized and safe for patients. We reinforced training on the cleaning process for the airborne/droplet virus. I constantly stressed wearing PPE and hand washing. I am so proud of the team for stepping up by protecting our patients. They became warriors to fight the virus. I believe without my husband’s support and God I would not have been able to cope. I have lost friends and family from this virus. It saddens me that many of our people are now in the spirit world. Being a Native and growing up with Navajo beliefs, I had to be strong. My ancestors went through so much and our people are resilient. Prayer is our strength. I cried when I watched the news when the vaccine was given to the first person in the U.S. If everyone gets their vaccine we will be able to interact with family again. I am looking forward to that day! -
 2021-02-28
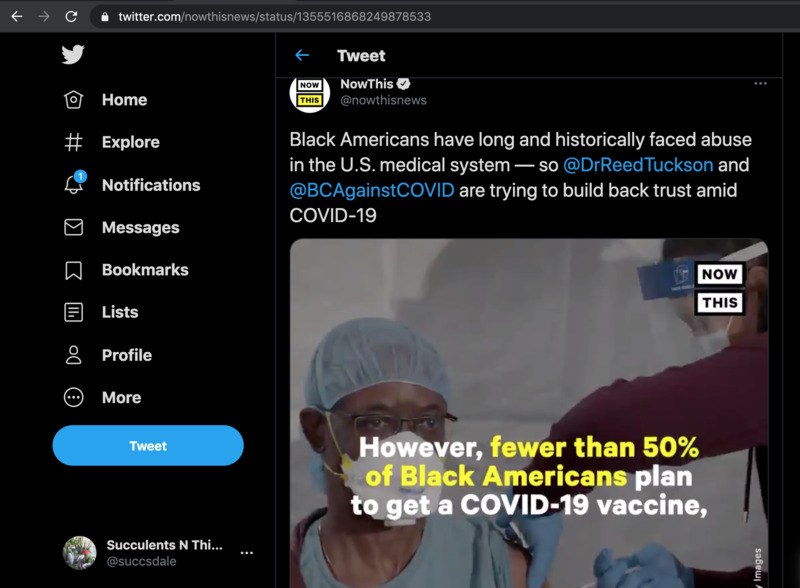
2021-02-28Building Trust in the Vaccine
When I was pregnant and going to birthing classes, I learned the terrifying rates of mortality for Black women giving birth. The numbers were horrifying, so there is no wonder to me why a high percentage of Black Americans do not plan on getting the COVID-19 vaccine. The American healthcare system has failed them. But a group of Black doctors are standing up to tell their communities that not taking the vaccine is to risk their life, and they deserve better. This video, shared to NowThisNews on twitter, describes what the doctors' message is and why it is so important. Black lives do matter, which is why these doctors are urging everyone to get the vaccine. The video states that more Black Americans have died from COVID than any other ethnic group. Hopefully, the vaccine will stop these deaths. -
 2021-02-07
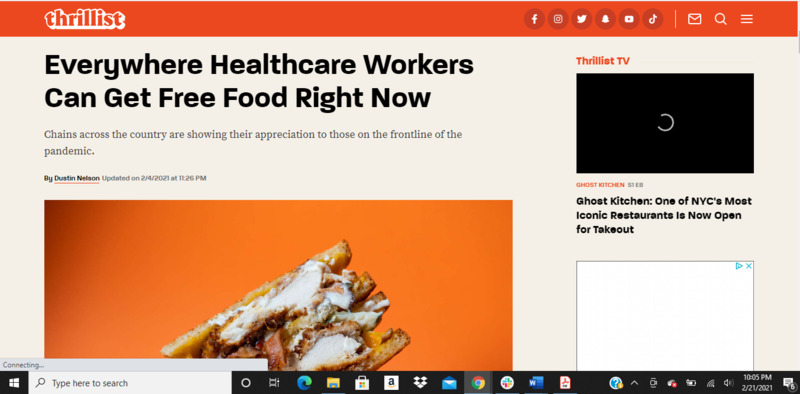
2021-02-07Supporting Healthcare Workers with Meals & Food Services
Everyone can surely agree that healthcare workers are our everyday heroes. Healthcare workers are the ones who had voluntarily trained and continue to medically assist those who need it without discrimination. All this while risking their own safety and well-being during a deadly pandemic. They are no strangers to long work hours while also having to always stay alert and ready, because quality care can greatly influence someone’s life. Due to most of their time taking care of patients, one can easily see how it can drain their own health as well. Hospitals are not exactly known for their top tier food options either. For these reasons, organizations like Meals for Heroes had worked with food services to help these essential workers with their meals. With the COVID-19 pandemic closing many businesses as well due to safety regulations, we have also been seeing the same businesses (as well as bigger ones) pitch in with meals and more affordable meal plans. Some places are even giving healthcare workers food for free. https://www.uab.edu/fightcovid19/impact/meals-for-heroes https://alabamanewscenter.com/2021/01/20/meals-for-heroes-will-continue-serving-meals-to-frontline-health-care-workers-fighting-covid-19/ https://www.thrillist.com/news/nation/free-food-for-healthcare-workers -
2020-10
Quarantine Tattoo
In August I got a tattoo that I did not want and did not like for seemingly no reason. Then in October I mentioned this to my psychiatrist and was promptly diagnosed with bipolar disorder. I had gotten my tattoo during a manic episode. The typical risk-taking behavior that I would do in my day to day life became more drastic and dramatic during COVID. When I am not manic I'm very careful with regard to the pandemic so the pandemic made my behavioral differences more pronounced and more obvious to a doctor. Due to the pandemic, I was able to receive a diagnosis and begin treatment. Had there not been a pandemic I likely would not have sought treatment as I would have continued to assume that these behaviors were just a normal part of my personality. -
 2020-05-28
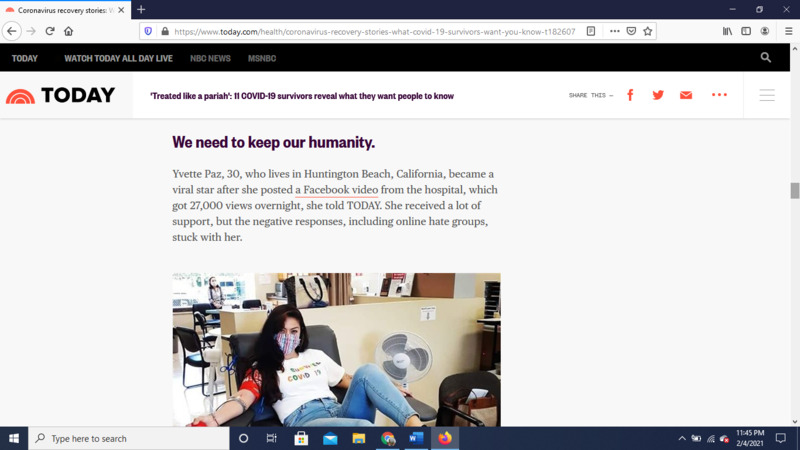
2020-05-28“Treated like a pariah': 11 COVID-19 survivors reveal what they want people to know
This article presents the sometimes-unspoken stigma that accompanies having Covid-19. It invited survivors to share what they want people to know, because, according to the article, “for many people living through this, sharing their story is the only way they feel validated as they wait for researchers to wade through the unknowns.” The article expresses feelings of isolation from some who are avoided now that they have had Covid. Others share that there is a sense of blame thrust upon them, by those who feel as though they are at fault for getting sick. Still others disclose the subpar treatment by their health providers. Their lessons include: the disease can turn severe quickly, Covid-19 shouldn’t be about politics, don’t let your guard down, warn your friends and family, it is not just the flu, people need to have empathy, the suffering is real, be your own advocate, precautions aren’t foolproof, researchers and doctors are trying their best, and be grateful. Overall, these stories remind us that even when a person survives, they have healing yet to go. -
 2021-01-27
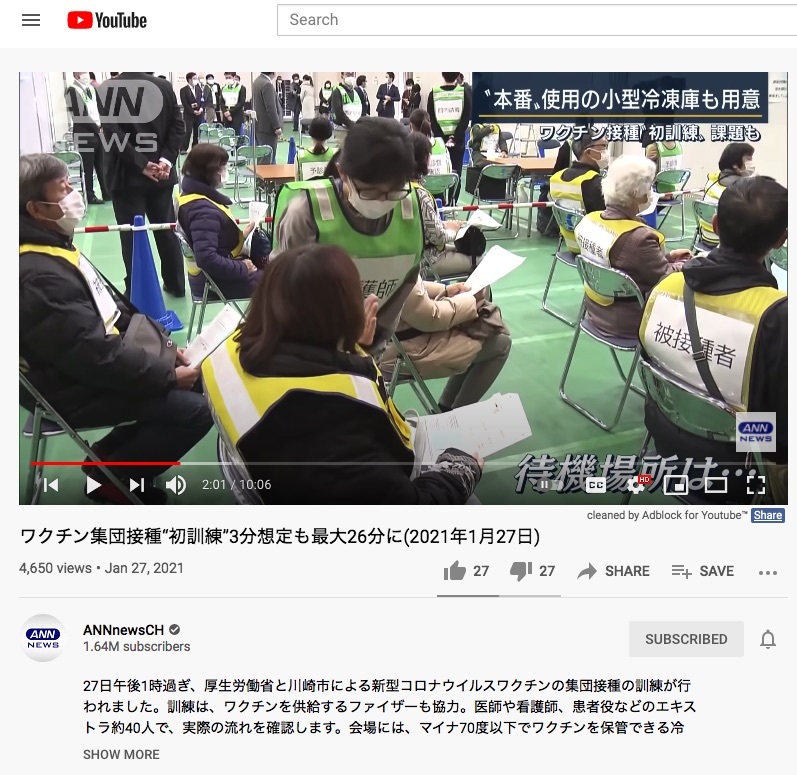
2021-01-27ワクチン集団接種“初訓練”3分想定も最大26分に(2021年1月27日) – Vaccine mass vaccination "first training" assumed 3 minutes and up to 26 minutes (January 27, 2021)
This was a news video where Kawasaki city in Japan conducted a practice round of vaccination process. Personally, I do get the reason why the practice is happening; however, Japan still doesn't have a set date of when vaccinations will actually happen. This news and event itself could lead to people having high hopes of getting vaccinations soon when in reality, it could take much longer. Unlike U.S., Japan does not have a culture of drive through, meaning people physically have to go to locations for the vaccines. Also, having large gatherings like this I personally think should be avoided and maybe they should have videotaped it and posted on YouTube on how to get vaccinated, instead of many people physically going to the place and learning how to be vaccinated. I have translated the video. After 1:00 pm on the 7th, the Ministry of Health, Labor and Welfare and Kawasaki City conducted a training for mass distribution of the new coronavirus vaccine. The training also cooperated with Pfizer, which supplies vaccines. About 40 vounteers of doctors, nurses, and patients checked the actual flow. At the venue, there was also a freezer where vaccines could be stored at a minus temperature 70 degrees or less. The Ministry of Health, Labor and Welfare has already conveyed the message of mass distribution to each local government. First, at the reception, complete the temperature measurement and identity verification, and fill in the questionnaire about your health condition and chronic illness. Next, a pre-examination will be conducted to see if the doctor can actually vaccinate, and if there are no problems, vaccination will be given. You will then need to wait 15-30 minutes to receive a vaccinated certificate and follow up for any side effects. According to the Ministry of Health, Labor and Welfare, it takes 3 minutes per person from pre-examination to vaccination, and if it takes 7 hours, 280 people can get the vaccine a day. However, it is said that some people took up to 26 minutes from the pre-examination to the vaccination in the training. Kawasaki City College of Nursing, President Noboru Sakamoto: "I was a simulation patient today, but I feel like I would continue asking questions like ‘I am really scared of allergies from this vaccination’. People who are receiving the vaccination are most likely afraid so we would need to consider and adjust the fact that people will ask questions, for future vaccination sessions” the issue of selecting a venue was also pointed out. Kawasaki City College of Nursing, President Noboru Sakamoto: "I think it's okay if it's a gymnasium, but when it comes to elementary, junior high and high schools, we use it in regular class for students. Once vaccination starts, we have to use it for at least half a year or a long period of time. Given that it is unbearable, we will not be able to use gymnasiums that are used for education every day.” Some local governments cannot prepare large venues. In Izu Oshima, which has a population of about 7,500, we plan to vaccinate at the Oshima Medical Center, the only medical institution on the island. Oshima Town Welfare Health Division, Tetsuya Yoshizawa, Chief: "We plan to have Saturdays and Sundays, which are holiday medical treatment days, considering the system of medical staff. If that is not enough, we are considering about one day from the weekday. However, the trouble is that we have to vaccination twice. This is just new for us.” The vaccine will be shipped by ship, but the schedule may be affected depending on the weather. Tetsuya Yoshizawa, Chief of the Oshima Town Welfare Health Division: "Of course, depending on the weather conditions, it may be canceled. If we can't see when the vaccine will arrive, it's hard to prepare.” Vaccines are first transported from warehouses that can be stored at ultra-low temperatures to hospitals equipped with freezing facilities. However, since the number of facilities equipped with freezing facilities is limited, we plan to refrigerate the facilities and transport them to each vaccination site and facilities for the elderly. The government plans to secure 10,000 ultra-low temperature freezers and aims to complete the installation by the end of May. At a facility for the elderly in Chiba City, we have begun to consider whether vaccination can be done at the facility. This is because elderly people with dementia are admitted and it is difficult to take them to the vaccination site. Chiba Workers Welfare Association, Megumi Kadowaki, Director of Nursing Care: "If possible, it is safest to ask a" family doctor "and inject the vaccine." However, whether the family doctor is given permission to inject the new corona vaccine is still unknown. In addition, Ms. Kadowaki wants the procedure for vaccination to be as simple as possible. Chiba Workers Welfare Association, Megumi Kadowaki, Long-term Care Manager: "Employees are doing their best to prevent infection and protect users of the center, so I would like you to reduce the new office work as much as possible" because there are still those who cannot visit the vaccination. Dr. Tomitsuka is visiting the clinic in Ota-ku, Tokyo. There are currently 60 patients on-site. In the middle of this month, Ota-ku recruited doctors to register as vaccination doctors for patients, including me. He says he intends to join, but he is worried about carrying the vaccine. Director of Seseragi Clinic Tamagawa Taro Tomitsuka: "The biggest fear is that the vaccine's effect is lost after transportation because the environment of minus several ten degrees cannot be maintained. At the end, I have to vaccinate it. I am accustomed to storing and transporting the vaccine. I really want people who are used in transporting and maintaining the temperature to do it.” It is said that cooperation with doctors will become more important in the future toward the first vaccination. Director of Seseragi Clinic Tamagawa / Taro Tomitsuka: "I think it's safer and more secure if you leave it to your family doctor, but on the other hand, it's a vaccination that requires speed, so you can involve local doctors well.” Minister Kono met with the presidents of the National Mayors' Association. Minister Kono, in charge of vaccination: "I told you that vaccination of the elderly will be after April 1st at the earliest. 7日午後1時過ぎ、厚生労働省と川崎市による新型コロナウイルスワクチンの集団接種の訓練が行われました。訓練は、ワクチンを供給するファイザーも協力。医師や看護師、患者役などのエキストラ約40人で、実際の流れを確認します。会場には、マイナ70度以下でワクチンを保管できる冷凍庫も用意されました。 厚労省は、すでに、集団接種のイメージを各自治体に伝えています。まず受付で、検温や本人確認などを済ませ、健康状態や持病などを問診票に記入。次に、実際に医師が接種できるかどうかを診る予診を行い、問題がなければワクチン接種を行います。その後、接種済みの証明書を受け取り、副反応が出ないかの経過観察のため、15~30分、待機する必要があります。 厚労省は、予診から接種まで1人3分で、7時間行えば、一日280人が、ワクチンを打つことができるとしています。ただ、訓練では予診から接種まで、最大で26分かかった人もいたといいます。 川崎市立看護短期大学・坂元昇学長:「きょうは模擬患者だったが、つい本音で『これってアレルギーが怖いんですね』とか、お医者さんを目の前にすると、そういう話が延々と続いてしまう。受けられる方は不安だろうから、たくさん質問するというものを今後、どうやって調整するか」 会場選びの課題も指摘されました。 川崎市立看護短期大学・坂元昇学長:「体育館だったらなんでもいいやと思われるが、小中高校になると、通常の授業で使う。いったん予防接種が始まれば、少なくとも半年とか、長い期間、使わざる負えないということを考えると、日々、教育で使うような体育館等は使えないだろう」 大きな会場が用意できない自治体もあります。人口約7500人の伊豆大島では、島内唯一の医療機関・大島医療センターで接種を行う予定です。 大島町福祉けんこう課・吉澤哲也課長:「医療従事者の体制等も考えて、休日の診療日にあたる土曜、日曜を予定。それで対応しきれない場合は、平日いずれかの曜日1日くらいを考えている。ただ、厄介なのが2回、接種しなければいけないというところで。いかんせん何もかも初めてなので」 ワクチンは船で運ばれる予定ですが、天候次第でスケジュールに影響が出る可能性もあります。 大島町福祉けんこう課・吉澤哲也課長:「当然、天候状況によっては“欠航”ということもある。我々もワクチンが、いつごろ手元に届くのか、その辺が見えてこないと、準備のほうもなかなか進めるに進められない」 ワクチンは、超低温保存ができる倉庫から、まずは、冷凍設備が整った病院などに運ばれます。ただ、冷凍設備が整った施設は限られているため、その後は、冷蔵で、各接種会場や高齢者施設などに運ばれていく予定です。政府は、超低温冷凍庫を1万台確保する方針で、5月中の設置完了を目指しています。 千葉市にある高齢者施設では、施設で接種ができないかと検討を始めました。入所しているのが認知症の高齢者で、接種会場へ連れていくことが難しいためです。 千葉勤労者福祉会・門脇めぐみ介護部長:「できれば“かかりつけ医”が問診をして、ワクチンを接種してしただくのが一番、安心」 ただ、かかりつけ医に新型コロナのワクチンの接種許可が下りるかは、まだ、わからないといいいます。さらに、門脇さんは、接種までの手続きなどを、なるべく簡潔にしてほしいと訴えます。 千葉勤労者福祉会・門脇めぐみ介護部長:「職員は、感染対策と利用者さんを守ることで精いっぱいなので、新たに生じる事務作業は極力減らしていただきたい」 接種会場に足を運べない人は、まだいます。東京都大田区で訪問診療を行っている富塚医師。訪問診療している患者は現在60人います。今月中旬には、大田区から患者にワクチン接種をする医師として登録するよう呼び掛けられました。応じるつもりだといいますが、ワクチンを運ぶことに不安があるといいます。 せせらぎクリニック多摩川・富塚太郎院長:「マイナス数十度の環境が保てなくて、ワクチンの効果が運搬後になくなっているというのが最大の恐怖。最後は私が打つ。ワクチンの保存と運搬は慣れた人にしていただきたいのが本音」 初めてのワクチン接種に向け、今後は、医師の連携が、より大切になってくるといいます。 せせらぎクリニック多摩川・富塚太郎院長:「かかりつけ医に任せていただければ、より安全・安心で、対処できると思うけど、一方で、速さを求められているワクチン接種なので、うまく地域の医者を巻き込んでいただければなと」 河野大臣は、全国市長会会長らと会談しました。 “ワクチン接種”担当・河野大臣:「高齢者のワクチン接種が、早くても4月1日以降になるとお伝えした。 -
2020-03-13
My Thoughts on The Virus
I have read many statistics and learned much about this virus and I have come to a conclusion that it is dangerous and what doctors have been saying since the start is totally correct, I heard that it won't stop until almost everyone on earth has gotten it, and that is slowly becoming a reality, but i also heard that the mortality rate will remain at 1% no matter what which has also shown to be true. The one thing that bothers me though is that scientists said it could last up to 2 years, which is starting to sound realistic and not extremely exaggerated. My final thoughts in this virus are that we should all do our best to stay safe and listen to doctors. -
2021-01-26
Statistics about Covid
The internet says there was been 99.9 million cases and 2.15 million deaths globally. But in the US the was been 25.3M cases and 421K deaths. I personally don't trust the Covid death count completely because there has been a lot of rumors that they are counting people who die from heart attacks and things like that to the count of the Covid death count. I am not sure why, but I have heard that the more covid deaths counted the more money the doctors get. My life through the pandemic was weird. I got a lot of time on my hands to workout and train for football and bulk up, but on there other hand school is so much harder for me. Everybody else loves because they can cheat, but my mom would kill me ( if I got caught ). -
2021-01-19
My feelings on the rules and procedures that we have to take.
I think the rules and procedures we have to take to be safe during this pandemic are reasonable and fair. I think this because everyone wants to be safe and healthy especially doctors so when many doctors are telling us specific things to follow i'm going to think about why this i benefiting me and keeping me safe. Like wearing a mask, people say they don't work but doctor's on the other hand say they are very useful and will protect you from the virus that is in fact airborne. Staying six feet this is another big one, this distance is the correct and closest distance you can be from someone without picking up any viruses. These are the two biggest rules and procedures that I think we should follow and that work. -
2021-01-18
My experience with getting the Covid vaccine
For 24 hours I felt something weird on my arm but the doctor told me to move it around so I can get into my body. The area of the shot felt sore, just like any other vaccine. After a week it barely felt like anything. It just felt like any other vaccine. -
 2020-12-13
2020-12-13Doctors Can Work From Home Too
A cartoon of a nurse assisting a remote check-up -
 2020
2020Wellness Support Line
The demands of the pandemic are having a serious impact on the emotional, psychological and physical wellbeing of healthcare workers across the country. The Canadian Medical Association wishes to support frontline workers by providing them with access to a Wellness Support Line to ensure they have high-quality and tailored mental health services for all their needs. -
 2020-05-26
2020-05-26Isolation Gown Photograph
Hospital CEO Patrick Gaskin takes a photo in an isolation gown created by Barbarian Sportswear in Kitchener, Ontario. Barbarian Sportswear began manufacturing isolation gowns in response to the need for PPE. -
 2020-11-20
2020-11-20Alberta Health Services Photo
This is a photograph of a Canadian ICU physician calling a patient's family to inform them of the patient's passing. The photo highlights the impact of the second wave which has hit Alberta badly in November and December 2020. -
 2020-10-01
2020-10-01Interview by Dr. Juilee Decker and Alicia Evans, educator and Fiber Artist
Alicia Evans describes her busy life before COVID. She was a professor at City University New York as well as a fiber artist and medical actor. She describes how her work changed due to COVID, and how virtual learning has changed the way things are taught. She shares her art and stories about how she is impacting lives through her work and art. -
 2020-11-05
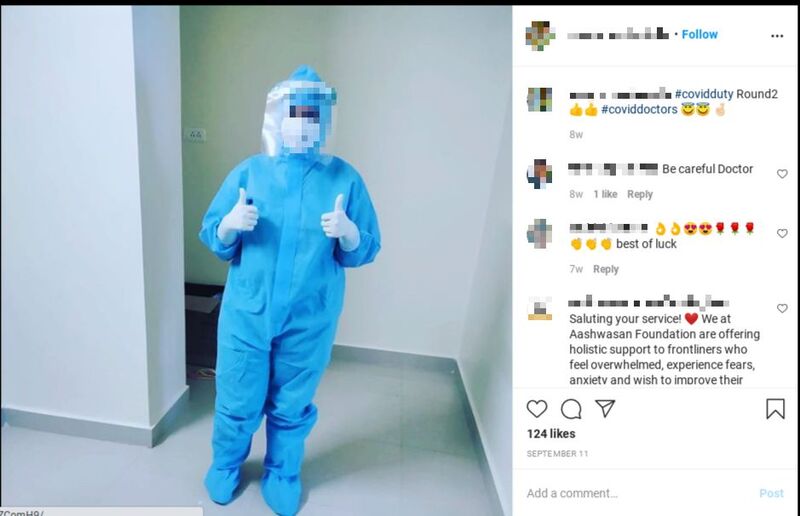
2020-11-05Doctor Shares Photo Of Himself Ready To Work On The Covid Floor
A doctor shares a photo as he prepares for a shift of taking care of coronavirus patients. He is in full PPE. -
 2020-04-27
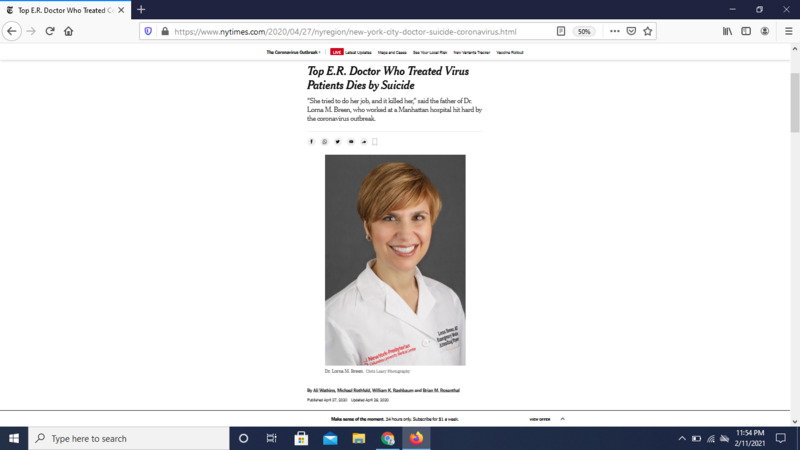
2020-04-27Doctor cannot come to terms with the things she saw, takes her own life
An emergency room doctor in New York committed suicide while staying with family in Virginia. Her family say she had become detached, and spoke of the horrors she saw while working with coronavirus victims. Her family would like her to be remembered as a hero. The doctor's family has set up a foundation that gives mental health support to health care providers. -
 2020-10-07
2020-10-07Young Doctor Dies of Covid
This doctor worked in the emergency department at a hospital and refused PPE repeatedly because there was such a shortage of it. The article addresses the fact that so many medical professionals have died because of inadequate PPE. -
2020-10-27T12:06
An Unexpected Return
After being out sick for a week filled with chills, doctors appointments, the smell of soup, and the feeling of my warm blanket, I finally returned to school on Friday. I could see the empty classrooms, hear the quiet rooms, smell the hand sanitizer, touch the desks and door handles with precaution, and taste the uneasiness in the room. I heard whispers of people talking about “the coronavirus”. I saw people wiping down their desks and chairs. I smelt of constant cleaning supplies. I felt my heart beating faster than normal. This were all new senses that were coming to me in one day. I was confused and scared of the uncertainty of it all. I was barely comprehending and my mind was filled with thoughts and heat full of emotion. Little did I know, that was my last day of school. -
2020-10-05
Covid-19 and The Media
This article serves to inform the public of President Trump’s current condition after being diagnosed with Covid-19. It talks about how the doctors taking care of Trump contradict themselves when talking about his health condition and it leaves people wondering if he is in a worse state than they are making him out to be. I chose this article because I haven’t heard anything about Trump since he was diagnosed with Covid-19 and I wanted to know the latest news on his condition. This article shows how much of an impact Covid-19 is currently having in our Country. The President getting diagnosed with a disease right before the election can obviously have massive repercussions in the political world and America as a whole. This article is important because it lets people see the current state of our President in this crucial time and see the severity of what's going on. There is no bias that I could find in this article because the headlines, wording, sources, and even the pictures all have a very neutral standpoint. The article is simply presenting the facts and evidence they gathered from various sources. The responsibility of the media during the Covid-19 pandemic is to inform people of the situation around the world and spread the importance of safety. The pandemic has obviously started a lot of conflicts that can be seen all throughout the media, but the main priority of all people should be ensuring the safety of themselves and others around them.
