Items
topic_interest is exactly
contact tracing
-
 2020
2020International Discussion
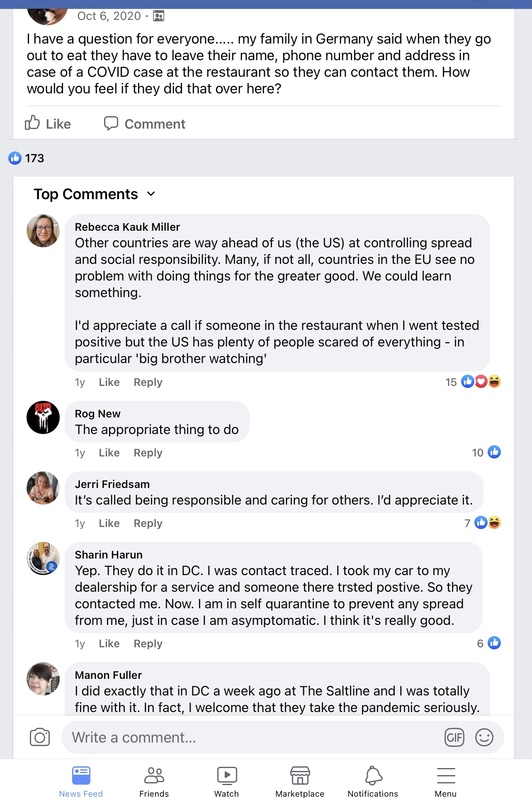
This conversation was interesting to me because it is an example of how the internet has been able to give people an idea of what the pandemic has been like in other parts of the world. It also presents a strategy some leadership enacted to control the spread of the virus. -
 2021-04-04
2021-04-04News Article: How a local response to COVID-19 helped slow deaths on the White Mountain Apache nation
By Amanda Morris of the Arizona Republic: When someone on the Fort Apache Indian Reservation receives a confirmed diagnosis of COVID-19, health care workers from the Whiteriver Indian Hospital jump into action. They personally visit the individual's home to test other household members, perform health evaluations on everyone there and trace any other potential contacts at risk for COVID-19 exposure. Health care workers in the community say that could be one reason why, even though the rate of confirmed COVID-19 cases among White Mountain Apache tribal members is nearly triple the state's rate, the death rate is much lower and continues to fall. Over 90% of COVID-19 cases in the White Mountain community are investigated within 24 hours of testing, according to Ryan Close, the director of the Department of Preventative Medicine at the Whiteriver hospital, which is the only hospital on the 1.67 million-acre reservation. "I feel like what we did made a huge difference," Close said. "We evaluated and admitted people aggressively and early. The tribe deserves an incredible amount of credit for mobilizing staff ... to make this response possible, because at some point it would have been very difficult to maintain without their considerable help." The quick response may have also helped the tribe turn the tide against rapid community spread of the virus, which scientists say could have been fueled by a single variant found only in the White Mountain tribal communities. The variant carried a mutation in the spike protein, which scientist theorize could have made it spread more rapidly than other strains of the virus. The number of confirmed COVID-19 cases among White Mountain Apache tribal members accounts for 24% to 28% of their population, according to Close, but the cumulative death rate among known cases is only 1.2%. By comparison, the statewide rate of infection was 11.5% with a 2% death rate among known cases. And over the winter, Close said the rate for the tribe dropped even lower, to about 0.5%. In a community with a high number of individuals with underlying health conditions, the low death rate and work of the tribe has been "remarkable," said David Engelthaler, director of the Translational Genomics Research Institute's infectious disease division in Flagstaff. The death rate also stands out as unusually low when compared with death rates in other Indigenous communities. Indigenous populations have been disproportionally affected by the pandemic. CDC data shows that Indigenous people are 3.5 more likely to be diagnosed with COVID-19 and almost twice as likely to die from COVID-19 than white people. Close credits a proactive strategy to combat COVID-19 that involved rapid contact tracing, in-person health evaluations and frequent outreach to high-risk COVID-19-positive individuals as well as early treatment with monoclonal antibodies and other antiviral therapies. Volunteers and health workers from the White Mountain Apache community were on the Whiteriver hospital's contact tracing team and high-risk COVID-19 outreach team, which Close said helped the team connect better with the people and work faster. One essential part of the team are the tribe's community health representatives, or CHRs, who are members of the community that serve as a cultural bridge between patients and medical establishments. JT Nashio, director of the Community Health Representatives for the tribe, said the "visceral connection" that CHRs have to the community helps them bring cultural awareness to the way questions are asked for contact tracing, which makes the process more effective and allows officials to better distribute information. "On top of that, quite simply, they know how to get around. It’s a big reservation and not all homes are easy to find," Nashio said. "But when you’ve lived here your whole life, you know where to find people. That became invaluable during the tracing and testing push during case surges." Virus mutation may have made it more transmissible When COVID-19 hit the White Mountain Apache nation, it spread rapidly. The community's first documented case was on April 1, 2020, from someone who had likely recently visited the Phoenix area, unknowingly caught COVID-19 and returned, according to Engelthaler. Within the first few weeks, Close said the community experienced a handful of deaths. "We soon had incidence rates that were skyrocketing. Case counts were going up very, very quickly," Close said. It's unclear why the disease spread so rapidly in the community, but the initial strain of COVID-19 that hit the community carried a mutation that Engelthaler believes could have made it more transmissible. "They were seeing the virus just rip through and have an 80 to 90 to 100 percent attack rate," he said. TGen partnered with the tribe and the U.S. Indian Health Services early on to provide tests to diagnose a case of COVID-19 and provide genetic analysis of the virus from each case. It showed one strain of the virus circulating in the tribal community that wasn't present anywhere else in the state. "This virus moved much faster than anything else we were seeing in Arizona at the time," Engelthaler said. "So we actually believe that we had one of these variant strains in Arizona that was causing very large numbers of cases, but it was secluded and maintained really only in that tribal population." The mutation, called the H245Y mutation, occurred in the spike of the virus, which Englethaler said is a "very sensitive" part of the virus where mutations can have a significant impact. Because of the low death rate, Engelthaler said TGen researchers would like to investigate the mutated strain of coronavirus seen among tribal members to see if it is also associated with a lower fatality rate. He acknowledged that other strains of the virus have since entered the community and that the actions of health care workers in the community and at the Whiteriver hospital is also responsible for the lower death rates. 'The earlier you treat an illness, the better' Close's biggest concern was that an outbreak would cause a "tsunami" of sick COVID-19 patients that would run the risk of overwhelming the Whiteriver hospital, which does not have an intensive care unit. Any patients that require intensive care need to be transported to other hospitals in the state. "We're a small hospital, we cannot take a wave of all very acute patients because there aren't enough ventilators in the hospital," Close said. "There aren't enough helicopters in the state to transport people out from our facility to a higher level of care." Within the first few weeks, Close said the community experienced a handful of deaths, and patients who had the poorest outcomes were the ones who self-presented at the hospital — often meaning they waited until they felt sick enough to go to the hospital. "People don't always bring themselves in early enough," Close said. "The earlier you treat an illness, the better." In response to this phenomenon, the hospital started a high-risk outreach program the third week of April. Health care workers regularly visited the homes of anyone who tested positive for COVID-19 and was at high risk for a poor outcome. Close recalls multiple days when he evaluated patients and found their oxygen levels dangerously low, even though they felt fine. It's a condition associated with COVID-19 known as "silent hypoxia," or "happy hypoxia." "They had no sense that they were even ill. They went on to get pretty sick in the hospital, but they survived and you can't help but think to yourself, 'Yeah, that's a life saved,'" Close said. "That person, if they had stayed home another day or another two days would not have done as well. They would have ended up on a ventilator or something." The Arizona Republic previously reported that the effects of the high-risk outreach program and contact tracing led to a fatality rate among tribal members of 1.6% last June, which was less than the state's rate of 2.5% and country's at 2.7% at the time. But the effect of the outreach program became even more pronounced over the winter, as the tribe and health workers gained access to monoclonal antibody treatments, according to Close. He said the high-risk outreach team started referring patients for antibody treatment in December as part of their protocol after the therapy received emergency use approval from the Food and Drug Administration. Hospital staff at the Whiteriver hospital then administered the antibody treatment. "We give that to people who are asymptomatic or mildly ill to prevent hospitalization," Close said. "The evidence currently suggests that reduces the risk that they're going to get sicker and get hospitalized and reduces the risk that they're going to die." Though there's no data proving the antibody treatments made a difference, Close said that after health care workers started using them, the community's COVID-19 death rate fell to 0.5%. Hospital workers also gave antiviral therapies, such as remdesivir, to patients early and often. "We probably overtreated some people," he said. "But the good news is it definitely led to significant reductions in mortality." Lessons for the future Close believes the different programs were so successful because health care workers were often able to test, trace, diagnose and treat individuals all in the same day — a feat he said was only possible because of how closely integrated hospital workers and community health workers were. "There were no barriers in communication between the public health arm of our response and the clinical care arm of our response," Close said. "It's really a case for an integrated health care system." As the tribe emerges from the pandemic and tribal members get vaccinated against the virus, Close said the hospital may start exploring other health conditions where it can use the high-risk outreach team, which is already trained and experienced in clinical evaluations. "The goal is to take what we've learned from COVID and now apply it to things that are not COVID-related," Close said. Another valuable lesson Close hopes to carry forward is how much of a difference visiting residents in their homes can make and how important building trusting relationships with the community is. Nashio said going door to door to trace and monitor COVID-19 cases was a natural step for CHRs, who had already gone door to door in the past for other community health campaigns. "We know firsthand how difficult it can be to not only connect with patients over the phone but communicate effectively over the phone," Nashio said. "When the community sees their CHRs coming to their door, it helps decrease the stigma of the disease." In addition to performing checkup evaluations and providing information, Nashio said CHRs can also provide food, medical supplies, cleaning supplies or services like grocery shopping and running basic errands. Not every tribal member has reliable internet or phone service, nor access to transportation, so Close said going door to door can be a good way to reach, and help, everyone. "Meeting patients where they are is invaluable," Close said. Amanda Morris covers all things bioscience, which includes health care, technology, new research and the environment. Send her tips, story ideas, or dog memes at amorris@gannett.com and follow her on Twitter @amandamomorris for the latest bioscience updates. Independent coverage of bioscience in Arizona is supported by a grant from the Flinn Foundation. -
 2021-02-15
2021-02-15One of my COVID-19 Case Investigations Experiences
I work as a medical investigator for my county, and I'm primarily tasked with asking detailed medical interviews and surveys of local patients (cases) who have recently tested positive for COVID-19. The second call I wanted to share regards an elderly case who had been admitted to the ICU shortly before I spoke with her. Her COVID-19 infection began approximately six weeks before our call, and she had long since recovered. Her husband, however, had not. He passed away in a local hospital, and she had only recently begun adjusting to her new life without him. She described him as the kindest man she had ever known, and stopped the interview several times to share heartbreaking stories of the wonderful things he had done for her and their family over more than six decades of marriage. She explained she had fallen in her backyard, broken her hip, and laid in the cold rain for about two hours before anyone found her. That's what landed her in ICU, NOT a COVID infection. She cried several times during our two-hour call, and I occasionally joined her. She explained that she had no COVID-19 symptoms, but still tested positive when the hospital administered their required test. I explained shedding and what that meant for her circumstances, which was the first time she remembered having been told that information. As she had not been contacted before to complete the survey, she graciously agreed to speak with me long enough to do so, all the while laid-up in ICU with a broken hip and awaiting a very unknown future. Among her greatest hopes that day was to make it through surgery well enough to go home to her son's gourmet cooking. She hadn't seen anyone but medical staff since her admit as the hospital disallowed visitors at that time. After we disconnected, I sent a Get Well gift to her hospital. She spoke several times of her Christian faith and belief in her husband's salvation, so I had a carved wood angel sent to her room from the hospital gift shop. We never spoke again, but I hope she understands how much she helped me that day by letting me help her in some small way. -
 2021-02-15
2021-02-15One of my COVID-19 Case Investigations Experiences
I work as a COVID-19 medical investigator for the Arizona county in which I live. I recently called on a monolingual Spanish speaker who turned out to be a retirement-age mother of adult children and infant grandchildren. The first time we spoke, she very politely agreed to complete our medical interview by phone, and I began working through the initial demographics section. As she answered my questions, she began asking questions of her own regarding her potential experience and that of her family, all of whom were ill by that time or presumed to be positive due to extended close contact. The pace and tone of her speech evolved as her volume increased, and her intense emotional distress required no common language to comprehend. The primary source of her concern was her adult daughter who lived at another location with her two children. Our case feared her daughter had to have immediate help to even dial a phone, much less to care for herself and her children. The case wanted to break isolation at her home to travel to her daughter' home to aid her child and grandchildren, but, with the interpreter's help, we worked through her fears, established an action plan that allowed the case and her husband to stay home, and connected her daughter with medcal professionals to evaluate her circumstances and need for urgent intervention. The case and I agreed those needs superseded the interview as she was both aware and isolated, and we agreed to speak the following day. On callback, her emotions had completely turned around in that day, her daughter had been evaluated over the phone, acquired the information and guidance she needed, and the case believed her child and grandchildren were now safe and well. Throughout the roughly 90-minute translated interview, she repeatedly expressed her gratitude for our having called and helped her family and information and guidance. Despite the number of times our patients/cases have expressed anger, outrage, suspicion, or worse at our medical investigation and contact tracing efforts, this series of calls made them worthwhile. -
 06/02/2020
06/02/2020Canada's Nunavut: A vast territory with few people - and no coronavirus
Nunavut remains the only state-level jurisdiction in North America not to record a single case of the virus that has sickened millions and killed more than 375,000 people worldwide. Every other Canadian province and territory and every U.S. and Mexican state has reported at least a few. -
 2020-12-14
2020-12-14Canada Crushing the Curve
A video showcasing Canada's early success in preventing the spread of the pandemic compared to the US -
 2020
2020Contact Tracing Explained
An infographic of how and why contact tracing is done. -
 2020-11-18
2020-11-18With Cases Surging, Colleges Turn To Students For Help
As COVID-19 cases at universities surge, universities have started to hire students to help with contact tracing. -
 2020-07-23
2020-07-23COVID-19 Contact Tracing Notice - Healthcare Worker
This was an email sent to my brother, who is a third year Doctor of Optometry student at the University of Melbourne. One of his classmates had tested positive for Covid-19, and he had been in the same lab room doing practicals together during this time. His whole class was asked to self-isolate for a two-week period, and his exams for the semester were pushed back as well. Although he does no directly deal with Covid-19 related patients, as a healthcare worker, he must come in close contact with people on a greater basis than almost any other profession. He isolated for the required period and was tested twice, thankfully with a negative result both times. Each test required 1-2 days turnaround. This object shows the steps organisations are taking to ensure proper contact tracing and in taking care both their patients and students. It also shows how healthcare workers, who come in close physical contact with others, are inherently at high risk and need to be extra careful not to catch or spread diseases. HIST30060.
